Scopus, KCI, KoreaMed

Search
- Page Path
- HOME > Search
- Epigallocatechin gallate increases fatty acid oxidation but not 24-hour survival in lipopolysaccharide-induced endotoxic shock in mice
-
Takayuki Irahara
 , Ryusuke Katsuki
, Ryusuke Katsuki , Dai Oishi
, Dai Oishi , Tsuguaki Terashima
, Tsuguaki Terashima , Md. Monirul Islam
, Md. Monirul Islam , Umme Salma
, Umme Salma , Shohag Majumder
, Shohag Majumder , Ridwan Ahmed
, Ridwan Ahmed , Eizo Watanabe
, Eizo Watanabe
- Ann Clin Nutr Metab 2026;18(1):27-33. Published online March 30, 2026
- DOI: https://doi.org/10.15747/ACNM.25.0036
-
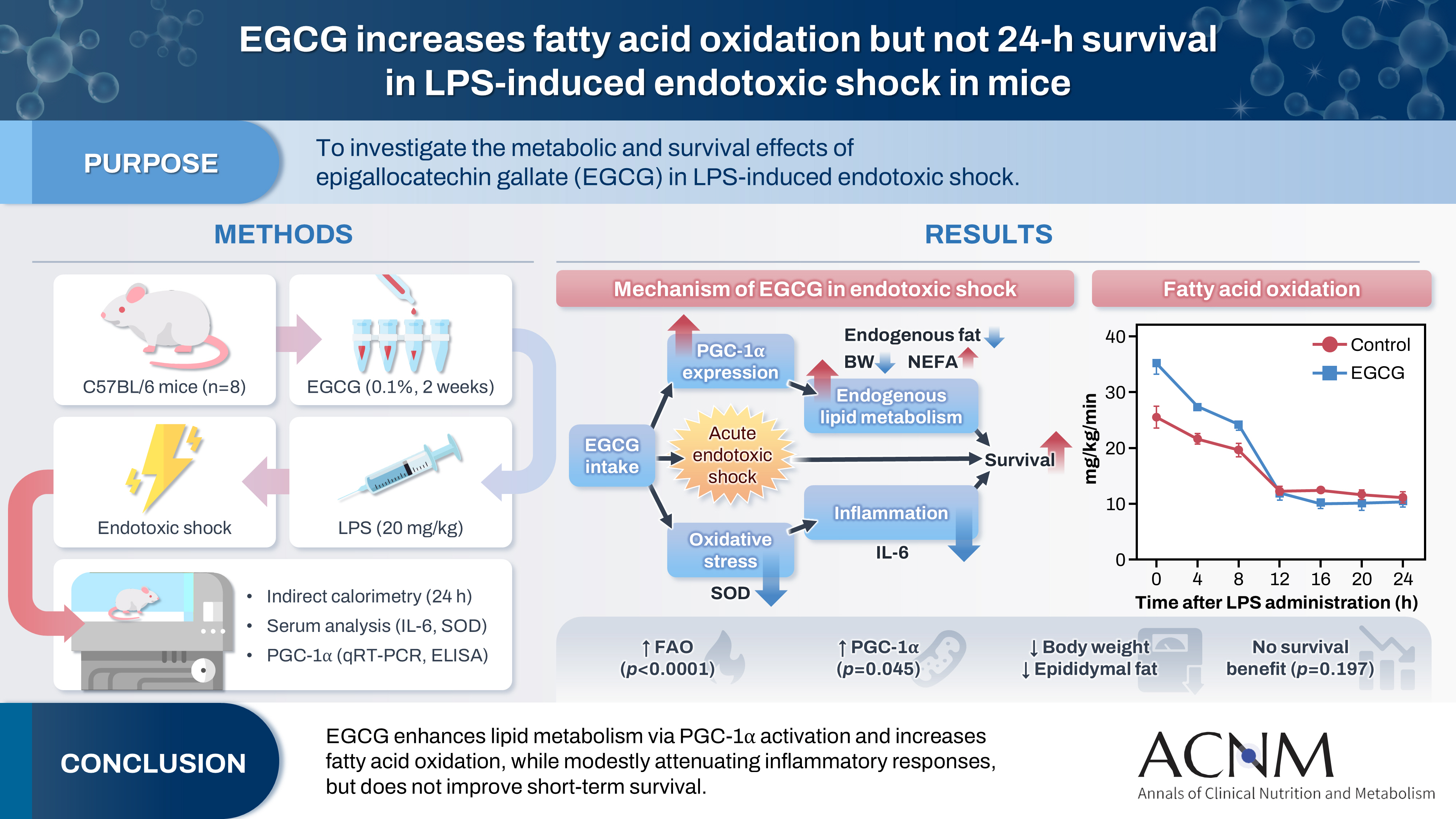
 Graphical Abstract
Graphical Abstract
 Abstract
Abstract
 PDF
PDF 
- Purpose
This study aimed to explore the effects of epigallocatechin gallate (EGCG) in critically ill patients using a mouse model.
Methods
C57BL/6 mice were divided into control and EGCG groups (n=8 per group). The EGCG group received a 0.1% EGCG solution for 2 weeks, after which the mice were intraperitoneally injected with a lethal dose of lipopolysaccharide to induce acute endotoxic shock. Indirect calorimetry was performed for 24 hours. Changes in body weight, epididymal fat weight, and survival were measured, together with serum lipid levels, interleukin-6 (IL-6), and superoxide dismutase (SOD) concentrations. The expression of peroxisome proliferator-activated receptor gamma coactivator 1-alpha (PGC-1α) was determined using quantitative real-time polymerase chain reaction, and its serum concentration was subsequently measured.
Results
Indirect calorimetry showed a significant increase in fatty acid oxidation (P<0.0001) in the EGCG group, along with significant decreases in body weight and epididymal fat weight (P<0.01 and P<0.05, respectively). Survival did not differ significantly between groups (P=0.197). Serum lipid levels, IL-6, and SOD showed numerical differences, although these differences were not statistically significant. Furthermore, hepatic PGC-1α expression showed a tendency toward upregulation, and serum PGC-1α levels were significantly higher (P<0.05).
Conclusion
EGCG stimulates endogenous lipid metabolism through PGC-1α activation and may suppress inflammatory responses; therefore, it may represent a potentially useful nutrient for acute nutritional therapy.
- 2,400 View
- 26 Download

- Association between decreased dietary intake during hospitalization and long-term weight loss in postoperative gastric cancer patients over 75 years of age: a retrospective cohort study
-
Daiki Tabe
 , Isao Miyajima
, Isao Miyajima , Akira Tsukada
, Akira Tsukada
- Ann Clin Nutr Metab 2025;17(1):75-84. Published online April 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0004
-
 Abstract
Abstract
 PDF
PDF - Purpose
Weight loss following gastrectomy is a significant concern, and maintaining adequate nutrition is necessary, especially given the growing number of older adult patients. This study examined the relationship between postoperative food intake and long-term weight loss in postgastrectomy patients aged ≥75 years.
Methods
Out of 88 patients who underwent gastrectomy for gastric cancer at our institute, 46 were aged ≥75 years. These patients were divided into two groups: one with an average energy intake exceeding 50% of the basal metabolic rate and one with an intake below 50% of the basal metabolic rate. The percentage change in body weight up to 6 months post-surgery was compared between the groups.
Results
In the group with higher dietary intake, the rate of weight change at 3 and 6 months postoperatively was lower, and fewer patients received postoperative adjuvant chemotherapy.
Conclusion
Poor postoperative food intake may serve as a predictor of weight loss up to 3 months following surgery in postgastrectomy patients aged ≥75 years. -
Citations
Citations to this article as recorded by- Strengthening collaboration: introducing the contributions of Japanese Society for Surgical Metabolism and Nutrition to Annals of Clinical Nutrition and Metabolism
Ye Rim Chang
Ann Clin Nutr Metab.2025; 17(2): 95. CrossRef
- Strengthening collaboration: introducing the contributions of Japanese Society for Surgical Metabolism and Nutrition to Annals of Clinical Nutrition and Metabolism
- 1,744 View
- 33 Download
- 1 Crossref

- Muscle Protein Metabolism in Critically Illness
-
Min Chang Kang

- Surg Metab Nutr 2020;11(2):35-39. Published online December 30, 2020
- DOI: https://doi.org/10.18858/smn.2020.11.2.35
-
 Abstract
Abstract
 PDF
PDF - Most patients experience a considerable amount of muscle wasting during critical care. A decrease in muscle mass causes weakness which inevitably leads to delayed recovery. Since muscle also plays an important role in protein metabolism, metabolic instability increases as muscle mass decreases. Accordingly, various treatments have been attempted to maintain muscle mass and function in critically ill patients; however, it is still difficult to prevent muscle loss. It is known that muscle wasting in critical illness is primarily due to increased muscle protein breakdown rather than a decrease in muscle protein synthesis. Nutritional therapy and rehabilitation are fundamentally important, but additional anabolic agents may be needed to overcome anabolic resistance. In this review, we will learn about muscle protein metabolism in critically ill patients and how various treatments affect muscle protein metabolism.
-
Citations
Citations to this article as recorded by- Combined intravenous bolus amino acid supplementation and mobilization on early muscle loss in critically ill adults: A randomized controlled trial
Lizl Veldsman, Guy A. Richards, Daniel Nel, Tertius A. Kohn, Renée Blaauw
Journal of Parenteral and Enteral Nutrition.2026; 50(2): 170. CrossRef - Reply to “Mechanical tension and autophagy suppression: Unmasking the confounders in ICU muscle preservation strategies”
Lizl Veldsman, Guy A. Richards, Daniel Nel, Tertius A. Kohn, Renée Blaauw
Journal of Parenteral and Enteral Nutrition.2026;[Epub] CrossRef - Low protein content of plant-derived nutrition limits the protein transition in hospitalized patients: Results from an observational study
M.A. van Bree, B.C. Schouten, E.S. Wolters, M.R. Soeters, H.M. Kruizenga
Clinical Nutrition ESPEN.2025; 69: 311. CrossRef - Combined Protein, Probiotics, and Exercise Therapy for Sarcopenia: A Comprehensive Review
Ryuk Jun Kwon, Mohammad Al Mijan, Soo Min Son, Wanho Yoo, Taehwa Kim
Cells.2025; 14(17): 1375. CrossRef - Double-Edge Effects of Leucine on Cancer Cells
Burkitkan Akbay, Zhannur Omarova, Alexander Trofimov, Bayan Sailike, Orynbassar Karapina, Ferdinand Molnár, Tursonjan Tokay
Biomolecules.2024; 14(11): 1401. CrossRef - Compartmental analysis: a new approach to estimate protein breakdown and meal response in health and critical illness
Nicolaas E. P. Deutz, Mariëlle P. K. J. Engelen
Frontiers in Nutrition.2024;[Epub] CrossRef - Amino acid kinetics in the critically ill
Nicolaas E.P. Deutz, Krista L. Haines, Paul E. Wischmeier, Mariëlle P.K.J. Engelen
Current Opinion in Clinical Nutrition & Metabolic Care.2024; 27(1): 61. CrossRef
- Combined intravenous bolus amino acid supplementation and mobilization on early muscle loss in critically ill adults: A randomized controlled trial
- 6,400 View
- 59 Download
- 7 Crossref

- Parenteral Glutamine Supplementation, Is It Optimal or Not?
- Dong Woo Shin
- Surg Metab Nutr 2018;9(1):5-10. Published online June 30, 2018
- DOI: https://doi.org/10.18858/smn.2018.9.1.5
-
 Abstract
Abstract
 PDF
PDF Glutamine is a conditionally essential amino acid in the body because it falls into a shortage of supply during the catabolic state. Glutamine plays a key role in the gut function, immune system, and other essential processes in the body. A number of small randomized controlled trials have demonstrated positive clinical outcomes of a glutamine treatment, such as the ICU length of stay, and hospital mortality with glutamine supplementation. On the other hand, recent reports of large scale randomized controlled trials assessing the efficacy of glutamine supplementation demonstrated some negative effects and the main conclusions were a trend toward an increased 28-day mortality and significantly increased hospital stay and 6-month mortality in those who received glutamine. With such results, many academic societies have recommended that IV and enteral glutamine should not be used in a critical care setting based on the moderate quality of evidence available. The indiscriminate use of glutamine supplementation in critically ill patients with any type of organ failure can have deleterious effects. Nevertheless, more sophisticated and well-controlled larger studies will be needed to confirm how these moderate quality results are corrected and suggest the optimal usage of glutamine. More recent clinical trials have focused on specific populations and demonstrated benefits in burn and elective surgery patients with glutamine supplementation. The poor correlation between the plasma glutamine concentration and tissue concentration evoke scattered knowledge about glutamine treatments. A better understanding of the glutamine metabolism and proper guidelines for supplementation are expected.
-
Citations
Citations to this article as recorded by- Neurocritical Care Nutrition: Unique Considerations and Strategies for Optimizing Energy Supply and Metabolic Support in Critically Ill Patients
Jae Hyun Kim, Yoon Hee Choo, Moinay Kim, Hanwool Jeon, Hee-Won Jung, Eun Jin Ha, JIWOONG OH, Youngbo Shim, Seung Bin Kim, Han-Gil Jung, So Hee Park, Jung Ook Kim, Junhyung Kim, Hyeseon Kim, Seungjoo Lee
Journal of Neurointensive Care.2023; 6(2): 84. CrossRef
- Neurocritical Care Nutrition: Unique Considerations and Strategies for Optimizing Energy Supply and Metabolic Support in Critically Ill Patients
- 2,102 View
- 5 Download
- 1 Crossref


 E-submission
E-submission KSPEN
KSPEN KSSMN
KSSMN ASSMN
ASSMN JSSMN
JSSMN
 First
First Prev
Prev


