Indexed in:
Scopus, KCI, KoreaMed
Scopus, KCI, KoreaMed

Most download articles
- Page Path
- HOME > Browse articles > Most download articles
Most-download articles are from the articles published in 2024 during the last three month.
Review
- Recent advances in refeeding syndrome in critically ill patients: a narrative review
-
Sang Woo Ha
 , Suk-Kyung Hong
, Suk-Kyung Hong
- Ann Clin Nutr Metab 2024;16(1):3-9. Published online April 1, 2024
- DOI: https://doi.org/10.15747/ACNM.2024.16.1.3
-
 Abstract
Abstract
 PDF
PDF - Purpose: The aim of this article is to provide a narrative review of the most recent studies on refeeding syndrome (RS) in critically ill patients and to summarize recent advancements that can be referenced in the treatment of these patients.
Current concept: RS in critically ill patients is a potentially lethal nutrition-related condition leading to sudden death. Initiation of food intake after a period of fasting can trigger rapid electrolyte uptake due to increased insulin release, leading to a decline in serum electrolytes with thiamine. This depletion may cause severe complications, such as cardiac arrhythmias, respiratory failure, seizures, and even death. The incidence of RS varies significantly, ranging from 7.4%–89%. Despite updates in diagnostic criteria over time, there remains a crucial need for criteria applicable to critically ill patients with underlying disorders such as metabolic derangement and organ dysfunction. To prevent RS, it is strongly recommended to start food intake after a fast at 20%–25% of estimated goals, gradually increasing the intake over several days. Close monitoring and electrolyte supplementation—especially of phosphorus, potassium, magnesium, and thiamine—are crucial, especially in critically ill patients. If electrolyte imbalances persist, slowing down or halting the progression of nutrition should be considered.
Conclusion: Clinicians should continue their efforts to promptly identify high-risk patients and to provide prevention and treatment for RS, particularly during the initiation of nutritional therapy in critically ill patients. Developing evidence-based protocols through further well-designed research is essential for effectively managing critically ill patients at risk of RS. -
Citations
Citations to this article as recorded by- Actualización en terapia médica nutricional del paciente críticamente enfermo: avances, desafíos y evidencia reciente
Nestor David Caicedo-Buitrago, Mateo Londoño-Pereira, Claudia Milena Ardila Melendez, Ricardo Merchán, Fernando Pereira-Paternina, Cristian Pinilla, Sonia Gamboa, Alejandra Cabral, Janeth Barbosa Barbosa, Maria del Pilar Morales, Bladimir Gil
Acta Colombiana de Cuidado Intensivo.2026; : 100612. CrossRef - Nutrition in the critically ill in resource-limited settings/low- and middle-income countries
Mervyn Mer, Martin W. Dünser
Current Opinion in Clinical Nutrition & Metabolic Care.2025; 28(2): 181. CrossRef - Nutritional Management of Liver Failure in the Intensive Care Unit
Zsófia Verzár, Rudolf Kiss, Csaba Pál Bálint, Annamária Pakai, Tímea Csákvári
Medicina.2025; 61(7): 1210. CrossRef - Comprehensive care of the patient with Refeeding Syndrome
Magdalena Kwiatkowska, Dominika Krupnik, Fabian Wesołek, Agnieszka Jonczyk, Łukasz Krzych
Polish Journal of Surgery.2025; 97(5): 64. CrossRef
- Actualización en terapia médica nutricional del paciente críticamente enfermo: avances, desafíos y evidencia reciente
- 64,167 View
- 1,598 Download
- 4 Crossref

Guideline
- Nutritional support for critically ill patients by the Korean Society for Parenteral and Enteral Nutrition — part I: a clinical practice guideline
-
Seung Hwan Lee
 , Jae Gil Lee
, Jae Gil Lee , Min Kwan Kwon
, Min Kwan Kwon , Jiyeon Kim
, Jiyeon Kim , Mina Kim
, Mina Kim , Jeongyun Park
, Jeongyun Park , Jee Young Lee
, Jee Young Lee , Ye Won Sung
, Ye Won Sung , Bomi Kim
, Bomi Kim , Seong Eun Kim
, Seong Eun Kim , Ji Yoon Cho
, Ji Yoon Cho , A Young Lim
, A Young Lim , In Gyu Kwon
, In Gyu Kwon , Miyoung Choi
, Miyoung Choi , KSPEN Guideline Committee
, KSPEN Guideline Committee - Ann Clin Nutr Metab 2024;16(3):89-111. Published online December 1, 2024
- DOI: https://doi.org/10.15747/ACNM.2024.16.3.89
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Purpose: Nutritional support for adult critically ill patients is essential due to the high risk of malnutrition, which can lead to severe complications. This paper aims to develop evidence-based guidelines to optimize nutritional support in intensive care units (ICUs).
Methods: The Grading Recommendations, Assessment, Development and Evaluation process was used to develop and summarize the evidence on which the recommendations were based. Clinical outcomes were assessed for seven key questions.
Results: We recommend the following: (1) initiate enteral nutrition (EN) within 48 hours after treatment as it is associated with improved outcomes, including reduced infection rates and shorter ICU stays; (2) early EN is preferred over early parenteral nutrition due to better clinical outcomes; (3) the use of supplementary parenteral nutrition to meet energy targets during the first week of ICU admission in patients receiving early EN is conditionally recommended based on patient-specific needs; (4) limited caloric support should be supplied to prevent overfeeding and related complications, particularly in the early phase of critical illness; (5) higher protein intake is suggested to improve clinical outcomes, such as muscle preservation and overall recovery; (6) additional enteral or parenteral glutamine is conditionally recommended against due to the lack of significant benefit and potential harm; and (7) fish oil-containing lipid emulsions is conditionally recommended due to their potential to enhance clinical outcomes, including reduced infection rates and shorter ICU stays.
Conclusion: These evidence-based recommendations can improve clinical outcomes and support healthcare providers in making informed decisions about nutritional interventions in the ICU. -
Citations
Citations to this article as recorded by- Case Report: Optimizing wound care: tailored nutritional strategies with immune- modulating enteral nutrients
Fiji Antony, Wafaa Ayesh
Frontiers in Nutrition.2026;[Epub] CrossRef - Actualización en terapia médica nutricional del paciente críticamente enfermo: avances, desafíos y evidencia reciente
Nestor David Caicedo-Buitrago, Mateo Londoño-Pereira, Claudia Milena Ardila Melendez, Ricardo Merchán, Fernando Pereira-Paternina, Cristian Pinilla, Sonia Gamboa, Alejandra Cabral, Janeth Barbosa Barbosa, Maria del Pilar Morales, Bladimir Gil
Acta Colombiana de Cuidado Intensivo.2026; : 100612. CrossRef - Rationale for Determining Energy Requirement in Hospitalized Patients: A Narrative Review
Suk-Kyung Hong, Kyung Mo Kim
Pediatric Gastroenterology, Hepatology & Nutrition.2026; 29(3): 212. CrossRef - Early supplemental parenteral nutrition and risk of subsequent enteroatmospheric fistula in high-risk open abdomen patients with persistent enteral nutrition intolerance: a landmark propensity score-matched cohort study
Wenyue Wang, Tian Xie, Chen Chen, Fen Chen, Dongliang Yang, Pengfei Wang, Yousheng Li
Frontiers in Medicine.2026;[Epub] CrossRef - Enteral Nutrition Versus a Combination of Enteral and Parenteral Nutrition in Critically Ill Adult Patients in the Intensive Care Unit: An Overview of Systematic Reviews and Meta-Analysis
Paraskevi Papanikolaou, Xenophon Theodoridis, Androniki Papaemmanouil, Niki N. Papageorgiou, Alexandra Tsankof, Anna-Bettina Haidich, Christos Savopoulos, Konstantinos Tziomalos
Journal of Clinical Medicine.2025; 14(3): 991. CrossRef
- Case Report: Optimizing wound care: tailored nutritional strategies with immune- modulating enteral nutrients
- 28,463 View
- 826 Download
- 5 Crossref

Reviews
- Mental health and micronutrients: a narrative review
-
Hyun Wook Baik

- Ann Clin Nutr Metab 2024;16(3):112-119. Published online December 1, 2024
- DOI: https://doi.org/10.15747/ACNM.2024.16.3.112
-
 Abstract
Abstract
 PDF
PDF - Purpose: It aims to summarizes the evidence for the association between specific individual nutrients and mental disorders, focusing on vitamin B12 and related B vitamins, vitamin D, probiotics, and zinc.
Current concept: Vitamin D deficiency is linked to depression, anxiety, and cognitive decline. Vitamin D enhances serotonin synthesis, has anti-inflammatory and neuroprotective effects, and regulates the hypothalamic-pituitary-adrenal axis and circadian rhythms. Vitamin B12 deficiency causes neurological dysfunction, mood disorders, cognitive decline, and psychotic symptoms, especially in the elderly. Vitamin B12 is involved in myelin formation, neurotransmitter synthesis, and preventing homocysteine-related neurodegeneration. Zinc deficiency affects neurotransmitters, neurogenesis, and antioxidant function, contributing to depression, anxiety, and cognitive impairment. Zinc supplementation improves symptoms and increases brain-derived neurotrophic factor levels. The gut-brain axis involves bidirectional communication between the gut microbiome and the central nervous system via the vagus nerve, enteric nervous system, immune system, and neuroendocrine pathways. Probiotics can modulate the gut microbiome to improve depression, anxiety, stress response, and cognitive function by influencing neurotransmitter production, reducing inflammation, and supporting the gut-brain connection.
Conclusion: Nutritional interventions, including vitamin D, B12, zinc, and probiotics, show promise as adjunctive therapies or preventive strategies for mental disorders. These nutrients have specific mechanisms of action on brain function and the gut-brain axis. Further research is needed to establish optimal dosage, timing, and administration methods for these nutritional approaches in supporting mental health. -
Citations
Citations to this article as recorded by- The Mouth–Mind Connection: Interplay of Oral and Mental Health in Older Adults
Alice Kit Ying Chan, Joanna Cheuk Yan Hui, Lindsey Lingxi Hu, Chun Hung Chu
Geriatrics.2026; 11(1): 8. CrossRef - Plasma vitamin profiles and their associations with metabolic health and mental wellbeing in midlife Asian women
Karen M. L. Tan, Mya Thway Tint, Rafael Medeiros Cabral, Ryan Lau, Michelle Z. L. Kee, Vandana Garg, Maria De Iorio, Sheryl S. L. Tan, Johan G. Eriksson
Scientific Reports.2026;[Epub] CrossRef - A nutritional blend of taurine, vitamins B6, B9, and B12 improves motivated behaviors in healthy adults—a double-blinded randomized clinical trial
Veeda Michelle Anlacan, Roland Dominic G. Jamora, Laura-Florina Krattinger, Evelina De Longis, Mickaël Hartweg, Myriam Steinmann, Laura Trovò
Frontiers in Nutrition.2026;[Epub] CrossRef - Vitamin D Supplementation in Adults with Depressive Disorder: A Retrospective Record Review of a Patient Panel
Janine Panker, Stacy Schoenbach, Pema Jessica Marcello, Julie Thompson, Sean Convoy
The Journal for Nurse Practitioners.2026; 22(6): 105785. CrossRef - Understanding the Connection Between Diet, Food Systems and Mental Health: A Qualitative Exploration of a Caribbean Small Island Developing State
Catherine R. Brown, Cornelia Guell, Madhuvanti M. Murphy
Nutrients.2026; 18(9): 1427. CrossRef - Associations between antioxidant vitamin intake and mental health in Swedish adolescents: a cross-sectional study
Martina Pensa, Karin Kjellenberg, Emerald Heiland, Örjan Ekblom, Gisela Nyberg, Björg Helgadóttir
European Journal of Nutrition.2025;[Epub] CrossRef - A Study of Nutritional and Sensory Qualities of Pea Protein Isolate Beverages with a View to Their Potential Use in Patients with Psychiatric Disorders
Lasma Plocina, Ilze Beitane
Foods.2025; 14(17): 2991. CrossRef - The association between animal‑based and plant‑based protein intake with sleep quality, mood, anxiety, depression and stress among elderly: a cross-sectional study
Batoul Ghosn, Hanieh Abbasi, Parisa Nezhad Hajian, Leila Azadbakht
BMC Public Health.2025;[Epub] CrossRef - Pediatric Culinary Medicine: Current Status, Challenges and Opportunities
Michelle Loy, Ashish Chogle, Hanna Tracy, Neha R Santucci, Khyati Mehta, Liane S. Sadder, Rima Jibaly, Alain J. Benitez, Maria R. Mascarenhas
Current Gastroenterology Reports.2025;[Epub] CrossRef - ВІТАМІН В12, ДЕПРЕСІЯ І ЦУКРОВИЙ ДІАБЕТ 2 ТИПУ (огляд лiтератури)
Вікторія Сергієнко, Вероніка Сегін, Олександр Сергієнко
Problems of Endocrine Pathology.2025; 82(4): 54. CrossRef
- The Mouth–Mind Connection: Interplay of Oral and Mental Health in Older Adults
- 65,535 View
- 848 Download
- 10 Crossref

- Dysphagia and quality of life: a narrative review
-
Jung Mi Song

- Ann Clin Nutr Metab 2024;16(2):43-48. Published online August 1, 2024
- DOI: https://doi.org/10.15747/ACNM.2024.16.2.43
-
 Abstract
Abstract
 PDF
PDF - Purpose: Dysphagia is a chronic health condition that causes impairment of eating and drinking functions. It occurs in various diseases such as stroke, neurodegenerative disease, brain tumor, and head and neck cancer, and can also occur during the normal aging process.
Current concept: As patients experience symptoms of dysphagia, they no longer feel the pleasure of eating, depression and anxiety increase, and self-esteem decreases. Prolonged loss of appetite can lead to malnutrition, which can lead to death due to serious complications such as aspiration pneumonia and airway obstruction. Dysphagia reduces quality of life by affecting basic activities of daily living, limitations in social life, nutritional deficiencies, and mood disorders.
Conclusion: Accordingly, I plan to conduct a literature review on the quality of life of patients with dysphagia. First, to determine the relationship between quality of life and sociodemographic, physical health, and mental health characteristics of patients with dysphagia. I also aim to review quality of life measurement tools and intervention programs for patients with dysphagia. -
Citations
Citations to this article as recorded by- Nursing interventions including psychological support and quality of life determinants in patients with dysphagia following stroke
Aihua Liu, Xuehong Liu, Ping Zhou
Journal of Research in Medical Sciences.2026;[Epub] CrossRef - Incidence and Risk Factors of Dysphagia After Cardiac Surgery: A Scoping Review
Christos Kourek, Vania Labropoulou, Emilia Michou, Stavros Dimopoulos
Journal of Clinical Medicine.2025; 14(12): 4279. CrossRef - Psychometric Properties of the Spanish Version of the Swallowing Quality of Life Questionnaire in Fibromyalgia Patients
Irene Calles-Plata, Araceli Ortiz-Rubio, Laura Pérez-Gisbert, Irene Torres-Sánchez, Andrés Calvache Mateo, Marie Valenza, Alejandro Heredia-Ciuró
Healthcare.2025; 13(22): 2948. CrossRef - Association Between Swallowing Dysfunction and Multidimensional Quality of Life Among Community-Dwelling Healthy Korean Older Adults: A Pilot Cross-Sectional Study
Hyun-Ah Jang, Jun-Seon Choi
Healthcare.2025; 13(22): 2964. CrossRef
- Nursing interventions including psychological support and quality of life determinants in patients with dysphagia following stroke
- 22,407 View
- 442 Download
- 4 Crossref

Guidelines
- A practical guide for enteral nutrition from the Korean Society for Parenteral and Enteral Nutrition: Part III. preparation of enteral nutrition formulas
-
In Seok Lee
 , Ye Rim Chang
, Ye Rim Chang , Bo-Eun Kim
, Bo-Eun Kim , Youn Soo Cho
, Youn Soo Cho , Sung-Sik Han
, Sung-Sik Han , Eunjung Kim
, Eunjung Kim , Hyunjung Kim
, Hyunjung Kim , Jae Hak Kim
, Jae Hak Kim , Jeong Wook Kim
, Jeong Wook Kim , Sung Shin Kim
, Sung Shin Kim , Eunhee Kong
, Eunhee Kong , Ja Kyung Min
, Ja Kyung Min , Chi-Min Park
, Chi-Min Park , Jeongyun Park
, Jeongyun Park , Seungwan Ryu
, Seungwan Ryu , Kyung Won Seo
, Kyung Won Seo , Jung Mi Song
, Jung Mi Song , Minji Seok
, Minji Seok , Eun-Mi Seol
, Eun-Mi Seol , Jinhee Yoon
, Jinhee Yoon , Jeong-Meen Seo
, Jeong-Meen Seo , for the KSPEN Enteral Nutrition Committee
, for the KSPEN Enteral Nutrition Committee - Ann Clin Nutr Metab 2026;18(1):3-9. Published online March 30, 2026
- DOI: https://doi.org/10.15747/ACNM.26.0046
-
 Abstract
Abstract
 PDF
PDF - Purpose
This guideline was developed to provide evidence-based recommendations for the safe preparation and handling of enteral nutrition (EN) formulas in order to improve patient safety and promote standardized clinical practice in Korea.
Methods
The key questions addressed the selection of open versus closed feeding systems, the safe preparation and handling of EN formulas, precautions related to blenderized tube feeding (BTF), and essential labeling requirements. Recommendations were drafted and refined through multidisciplinary expert consensus under the auspices of the Korean Society for Parenteral and Enteral Nutrition (KSPEN).
Results
The choice of feeding system should be determined according to the patient’s condition, risk of infection, and anticipated duration of feeding. Closed feeding systems are recommended because they reduce contamination risk and nursing workload, whereas open feeding systems require strict adherence to aseptic technique. For open or reconstituted EN formulas, hang time at room temperature should not exceed 4 hours, whereas closed feeding systems should follow the manufacturer’s recommended hang time. For BTF, administration time should be limited to 2 hours to minimize bacterial growth, and their use is contraindicated in medically unstable or immunocompromised patients. Accurate labeling, including patient identifiers, formula information, administration route, and hang time, is essential to prevent administration errors.
Conclusion
These guidelines provide a practical framework for the safe preparation and management of EN formulas. Adherence to standardized preparation protocols, including appropriate feeding system selection and strict hygiene practices, is essential for reducing complications and improving the safety of EN therapy.
- 1,282 View
- 55 Download

- The 2024 Korean Enhanced Recovery After Surgery guidelines for hepatobiliary and pancreatic surgery
-
Kwangpyo Hong
 , Hongbeom Kim
, Hongbeom Kim , Hyung Sun Kim
, Hyung Sun Kim , Hae Won Lee
, Hae Won Lee , Ho Joong Choi
, Ho Joong Choi , YoungRok Choi
, YoungRok Choi , Jae Do Yang
, Jae Do Yang , Sung-Moon Jeong
, Sung-Moon Jeong , Dae Wook Hwang
, Dae Wook Hwang , Do Joong Park
, Do Joong Park , Sang-Jae Park
, Sang-Jae Park , The Korean Enhanced Recovery After Surgery (ERAS) Committee within the Korean Society of Surgical Metabolism and Nutrition
, The Korean Enhanced Recovery After Surgery (ERAS) Committee within the Korean Society of Surgical Metabolism and Nutrition - Ann Clin Nutr Metab 2025;17(3):172-180. Published online December 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0034
-
 Abstract
Abstract
 PDF
PDF - Purpose
The Korean Enhanced Recovery After Surgery (ERAS) Committee within the Korean Society of Surgical Metabolism and Nutrition has developed comprehensive guidelines for hepatobiliary and pancreatic (HBP) surgery by adapting established international protocols. These guidelines provide evidence-based recommendations specifically tailored to the Korean healthcare system and address perioperative management for both pancreatoduodenectomy and hepatectomy.
Methods
The HBP subcommittee reviewed existing international ERAS guidelines and conducted an adaptation process. Key questions were identified based on national survey results from Korean HBP surgeons and were prioritized according to clinical relevance. The committee focused on elements supported by moderate- to high-quality evidence with strong recommendation grades. Literature searches were conducted through January 2025, and evidence quality was evaluated using GRADE methodology. Four key questions underwent formal assessment, and eight additional questions were adapted from international guidelines.
Results
Twelve key questions were selected and addressed, covering critical perioperative care domains: prehabilitation, preoperative nutritional assessment and support, anti-thrombotic prophylaxis, prophylactic abdominal drainage, preoperative biliary drainage, smoking and alcohol cessation, pre-anesthetic medication, minimally invasive surgical approaches, prophylactic nasogastric intubation, postoperative glycemic control, perianastomotic drainage management, and early mobilization protocols. Each recommendation was assigned specific evidence levels and graded for strength. High-quality evidence supported strong recommendations for the routine avoidance of prophylactic drainage in uncomplicated hepatectomy, early drain removal after pancreatoduodenectomy in low-risk patients, elimination of routine nasogastric decompression, and the implementation of early mobilization strategies.
Conclusion
These Korean-adapted ERAS guidelines for HBP surgery are expected to standardize perioperative care, reduce postoperative complications, shorten hospital stays, and enhance overall patient outcomes across Korean healthcare institutions. -
Citations
Citations to this article as recorded by- Adapting Enhanced Recovery After Surgery for hepatobiliary and pancreatic surgery: a Korean perspective
Sang Hyun Shin
Ann Clin Nutr Metab.2026; 18(1): 1. CrossRef
- Adapting Enhanced Recovery After Surgery for hepatobiliary and pancreatic surgery: a Korean perspective
- 3,303 View
- 88 Download
- 1 Crossref

Original Article
- Triglyceride-glucose index predicts future metabolic syndrome in an adult population, Korea: a prospective cohort study
-
Min-Su Park

- Ann Clin Nutr Metab 2024;16(3):168-172. Published online December 1, 2024
- DOI: https://doi.org/10.15747/ACNM.2024.16.3.168
-
 Abstract
Abstract
 PDF
PDF - Purpose: The triglyceride-glucose (TyG) index has been proposed as a reliable surrogate marker for insulin resistance. This study aimed to assess the utility of the TyG index in predicting the future presence of metabolic syndrome (MetS) in an adult population.
Methods: A total of 3,241 adults aged 40–70 years were included in this cross-sectional study. MetS was diagnosed based on the modified National Cholesterol Education Program Adult Treatment Panel III criteria, which requires the presence of at least three of the following components: abdominal obesity, elevated blood pressure, dysglycemia, hypertriglyceridemia, and low high-density lipoprotein cholesterol.
Results: In comparison to the homeostasis model assessment of insulin resistance (HOMA-IR), the TyG index exhibited superior diagnostic performance, with a higher area under the receiver operating characteristic curve of 0.854 vs. 0.702 for HOMA-IR. The 95% confidence interval for the TyG index was narrower, reflecting a more consistent predictive ability. Sensitivity for the TyG index was 79.7%, while specificity was 79.3%, compared to HOMA-IR, which showed a sensitivity of 52.7% and specificity of 78.3%.
Conclusion: The TyG index is a highly effective and robust tool for identifying individuals at risk for MetS, demonstrating superior sensitivity and predictive accuracy over HOMA-IR. This index could be a valuable clinical marker for early detection of MetS, aiding in the prevention and management of associated metabolic disorders. -
Citations
Citations to this article as recorded by- Triglyceride Glucose Index Is More Robust Surrogate Biomarker for Predicting Type 2 Diabetes Mellitus Than HOMA-IR in Population Attending Aulaqi Specialized Medical Laboratories, Yemen
Mohammed Hajar, Sami Ahmed, Basem Abdulfattah
American Journal of Laboratory Medicine.2026; 11(1): 9. CrossRef - Potential Associations of TyG Index and TG/HDL Ratio with Semen Parameters in Infertile Men
Ekrem Başaran, Ahmet Yıldırım Balık, Arda Taşkın Taşkıran, Dursun Baba, Muhammet Ali Kayıkçı
Sağlık Bilimlerinde Değer.2026; 16(1): 98. CrossRef - Association of the DeRitis ratio with insulin resistance in non-obese adults ‒ a cross-sectional study from South India
Sachin Kumar, Vignessh Raveekumaran, Sethuraj Selvaraj, K.S. Chenthil
European Journal of Clinical and Experimental Medicine.2026; 24(1): 122. CrossRef - Elevated triglyceride-glucose index and risk of thymoma-associated myasthenia gravis: a prospective analysis from the UK Biobank
Kangle Zhu, Jingwei Shi, Jingwei Zhao, Yi Zhao, Yao Zhang, Wuji Zhang, Mingjun Wei, Chu Zhou, Rusong Yang, Zhengcheng Liu, Zhuo Liu, Zhixiang Shen
Cardiovascular Diabetology.2025;[Epub] CrossRef - Association Between Triglyceride-Glucose Index and HbA1c in Prediabetes: A Preliminary Evaluation of a Potential Biomarker
Dharani A, Aravind Raj
Journal of MedVerse Research & Practice.2025; : 32. CrossRef
- Triglyceride Glucose Index Is More Robust Surrogate Biomarker for Predicting Type 2 Diabetes Mellitus Than HOMA-IR in Population Attending Aulaqi Specialized Medical Laboratories, Yemen
- 16,464 View
- 143 Download
- 5 Crossref

Guidelines
- A practical guide for enteral nutrition from the Korean Society for Parenteral and Enteral Nutrition: Part I. prescribing enteral nutrition orders
-
Ye Rim Chang
 , Bo-Eun Kim
, Bo-Eun Kim , In Seok Lee
, In Seok Lee , Youn Soo Cho
, Youn Soo Cho , Sung-Sik Han
, Sung-Sik Han , Eunjung Kim
, Eunjung Kim , Hyunjung Kim
, Hyunjung Kim , Jae Hak Kim
, Jae Hak Kim , Jeong Wook Kim
, Jeong Wook Kim , Sung Shin Kim
, Sung Shin Kim , Eunhee Kong
, Eunhee Kong , Ja Kyung Min
, Ja Kyung Min , Chi-Min Park
, Chi-Min Park , Jeongyun Park
, Jeongyun Park , Seungwan Ryu
, Seungwan Ryu , Kyung Won Seo
, Kyung Won Seo , Jung Mi Song
, Jung Mi Song , Minji Seok
, Minji Seok , Eun-Mi Seol
, Eun-Mi Seol , Jinhee Yoon
, Jinhee Yoon , Jeong Meen Seo
, Jeong Meen Seo , for KSPEN Enteral Nutrition Committee
, for KSPEN Enteral Nutrition Committee - Ann Clin Nutr Metab 2025;17(1):3-8. Published online April 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0002
-
 Abstract
Abstract
 PDF
PDF - Purpose
This study aimed to develop a comprehensive practical guide for enteral nutrition (EN) designed to enhance patient safety and reduce complications in Korea. Under the leadership of the Korean Society for Parenteral and Enteral Nutrition (KSPEN), the initiative sought to standardize EN procedures, improve decision-making, and promote effective multidisciplinary communication.
Methods
The KSPEN EN committee identified key questions related to EN practices and organized them into seven sections such as prescribing, delivery route selection, formula preparation, administration, and quality management. Twenty-one experts, selected based on their expertise, conducted a thorough literature review to formulate evidence-based recommendations. Drafts underwent peer review both within and across disciplines, with final revisions completed by the KSPEN Guideline Committee. The guide, which will be published in three installments, addresses critical elements of EN therapy and safety protocols.
Results
The practical guide recommends that EN orders include detailed elements and advocates the use of electronic medical records for communication. Standardized prescription forms and supplementary safety measures are outlined. Review frequency is adjusted according to patient condition—daily for critically ill or unstable patients and as dictated by institutional protocols for stable patients. Evidence indicates that adherence to these protocols reduces mortality, complications, and prescription errors.
Conclusion
The KSPEN practical guide offers a robust framework for the safe delivery of EN tailored to Korea’s healthcare context. It emphasizes standardized protocols and interdisciplinary collaboration to improve nutritional outcomes, patient safety, and operational efficiency. Rigorous implementation and monitoring of adherence are critical for its success. -
Citations
Citations to this article as recorded by- Rationale for Determining Energy Requirement in Hospitalized Patients: A Narrative Review
Suk-Kyung Hong, Kyung Mo Kim
Pediatric Gastroenterology, Hepatology & Nutrition.2026; 29(3): 212. CrossRef - Bridging evidence and clinical practice: a practical guide for enteral nutrition from the Korean Society for Parenteral and Enteral Nutrition
Suk-Kyung Hong
Ann Clin Nutr Metab.2025; 17(1): 1. CrossRef
- Rationale for Determining Energy Requirement in Hospitalized Patients: A Narrative Review
- 8,640 View
- 234 Download
- 2 Crossref

- The 2024 Korean Enhanced Recovery After Surgery guidelines for colorectal cancer
-
Kil-yong Lee
 , Soo Young Lee
, Soo Young Lee , Miyoung Choi
, Miyoung Choi , Moonjin Kim
, Moonjin Kim , Ji Hong Kim
, Ji Hong Kim , Ju Myung Song
, Ju Myung Song , Seung Yoon Yang
, Seung Yoon Yang , In Jun Yang
, In Jun Yang , Moon Suk Choi
, Moon Suk Choi , Seung Rim Han
, Seung Rim Han , Eon Chul Han
, Eon Chul Han , Sang Hyun Hong
, Sang Hyun Hong , Do Joong Park
, Do Joong Park , Sang-Jae Park
, Sang-Jae Park , The Korean Enhanced Recovery After Surgery (ERAS) Committee within the Korean Society of Surgical Metabolism and Nutrition
, The Korean Enhanced Recovery After Surgery (ERAS) Committee within the Korean Society of Surgical Metabolism and Nutrition - Ann Clin Nutr Metab 2024;16(2):22-42. Published online August 1, 2024
- DOI: https://doi.org/10.15747/ACNM.2024.16.2.22
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - The Korean Enhanced Recovery After Surgery (ERAS) Committee within the Korean Society of Surgical Metabolism and Nutrition was established to develop ERAS guidelines tailored to the Korean context. This guideline focuses on creating the most current evidence-based practice guidelines for ERAS based on systematic reviews. All key questions targeted randomized controlled trials (RCTs) exclusively. If fewer than two RCTs were available, studies using propensity score matching were also included. Recommendations for each key question were marked with strength of recommendation and level of evidence following internal and external review processes by the committee.
-
Citations
Citations to this article as recorded by- Development of the Korean enhanced recovery after surgery audit program
Soo-Hyuk Yoon, Jae-Woo Ju, Ho-Jin Lee, Jeesun Kim, Min Jung Kim, Ji Won Park, Do Joong Park, Seung Yong Jeong
Scientific Reports.2025;[Epub] CrossRef - Optimizing postoperative pain management in minimally invasive colorectal surgery
Soo Young Lee
Annals of Coloproctology.2024; 40(6): 525. CrossRef
- Development of the Korean enhanced recovery after surgery audit program
- 12,427 View
- 176 Download
- 2 Crossref

Original Articles
- Association between the calcium-to-phosphorus ratio and early hypophosphatemia in preterm infants receiving parenteral nutrition in Korea: a retrospective cohort study
-
Miseon Han
 , Jin Ok Kyun
, Jin Ok Kyun , Yoong-A Suh
, Yoong-A Suh , Jang Hoon Lee
, Jang Hoon Lee
- Ann Clin Nutr Metab 2026;18(1):44-53. Published online March 30, 2026
- DOI: https://doi.org/10.15747/ACNM.25.0039
-
 Graphical Abstract
Graphical Abstract
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material 
- Purpose
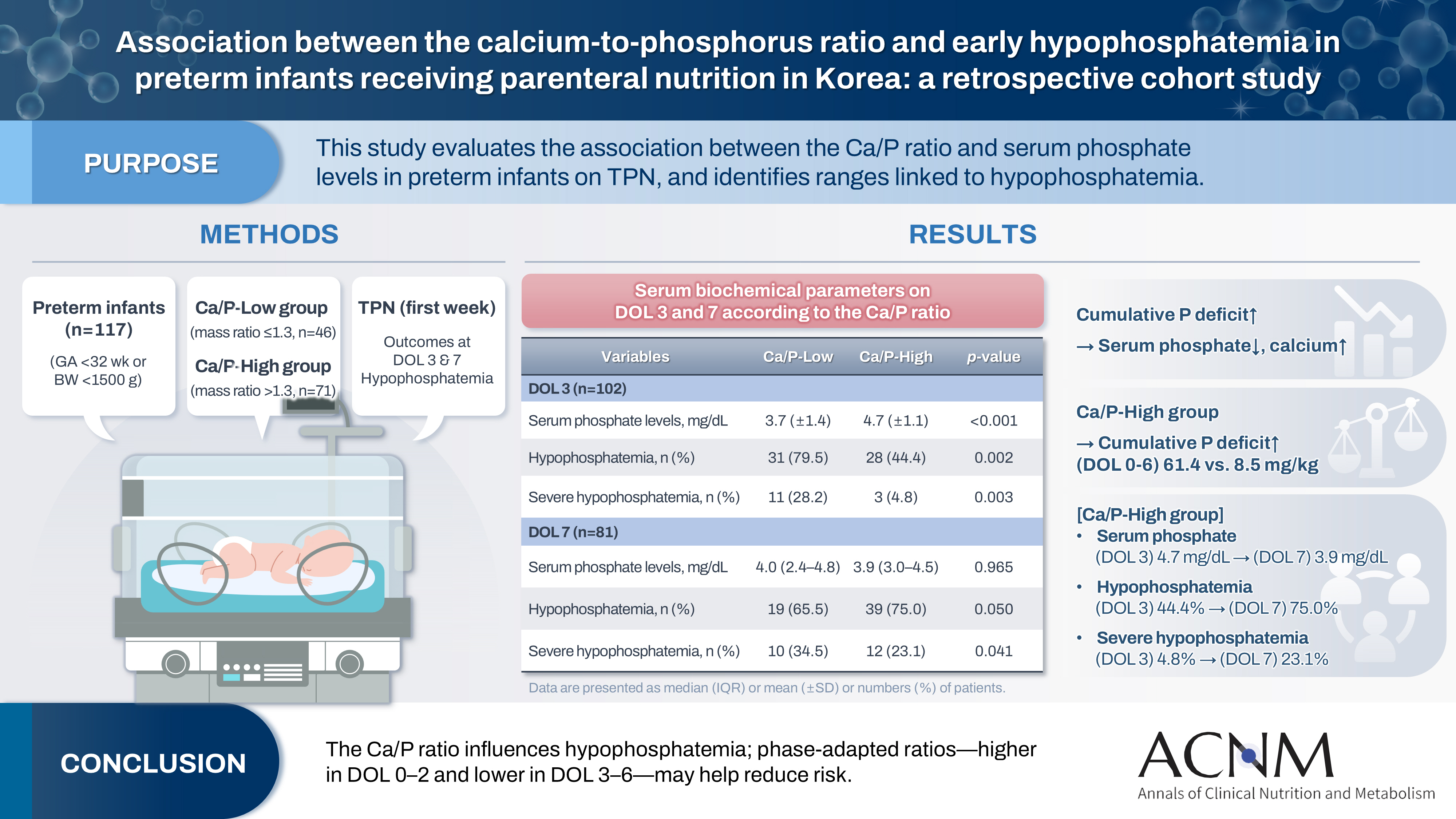
This study aimed to evaluate the association between the calcium-to-phosphorus (Ca/P) ratio and serum phosphate levels in preterm infants receiving total parenteral nutrition (TPN) and to explore Ca/P ratio ranges associated with hypophosphatemia.
Methods
We retrospectively reviewed the medical records of preterm infants admitted to the neonatal intensive care unit at Ajou University Hospital between January 2022 and June 2024. The review focused on TPN composition and serum electrolyte changes during the first week of life. Based on the cumulative Ca/P ratio during this period, infants were categorized into two groups: Ca/P-Low (mass ratio ≤1.3) and Ca/P-High (mass ratio >1.3).
Results
A total of 117 preterm infants were included in the analysis (Ca/P-Low group, n=46; Ca/P-High group, n=71). During the first week of life, the cumulative phosphorus deficit was significantly greater in the Ca/P-High group (61.4 mg/kg vs. 8.5 mg/kg; P<0.001). By day of life (DOL) 7, both hypophosphatemia and severe hypophosphatemia had increased markedly in the Ca/P-High group compared with DOL 3. In the Ca/P-High group, the incidence of hypophosphatemia increased from 44.4% on DOL 3 to 75.0% on DOL 7, while the incidence of severe hypophosphatemia increased from 4.8% to 23.1%.
Conclusion
These findings suggest that parenteral nutrition strategies may benefit from phase-adapted Ca/P ratios rather than a fixed ratio during the first week of life. A higher ratio may be considered during DOL 0–2, whereas a lower ratio may be considered during DOL 3–6, particularly when overall calcium and phosphorus supply is suboptimal.
- 1,033 View
- 24 Download

- Epigallocatechin gallate increases fatty acid oxidation but not 24-hour survival in lipopolysaccharide-induced endotoxic shock in mice
-
Takayuki Irahara
 , Ryusuke Katsuki
, Ryusuke Katsuki , Dai Oishi
, Dai Oishi , Tsuguaki Terashima
, Tsuguaki Terashima , Md. Monirul Islam
, Md. Monirul Islam , Umme Salma
, Umme Salma , Shohag Majumder
, Shohag Majumder , Ridwan Ahmed
, Ridwan Ahmed , Eizo Watanabe
, Eizo Watanabe
- Ann Clin Nutr Metab 2026;18(1):27-33. Published online March 30, 2026
- DOI: https://doi.org/10.15747/ACNM.25.0036
-
 Graphical Abstract
Graphical Abstract
 Abstract
Abstract
 PDF
PDF 
- Purpose
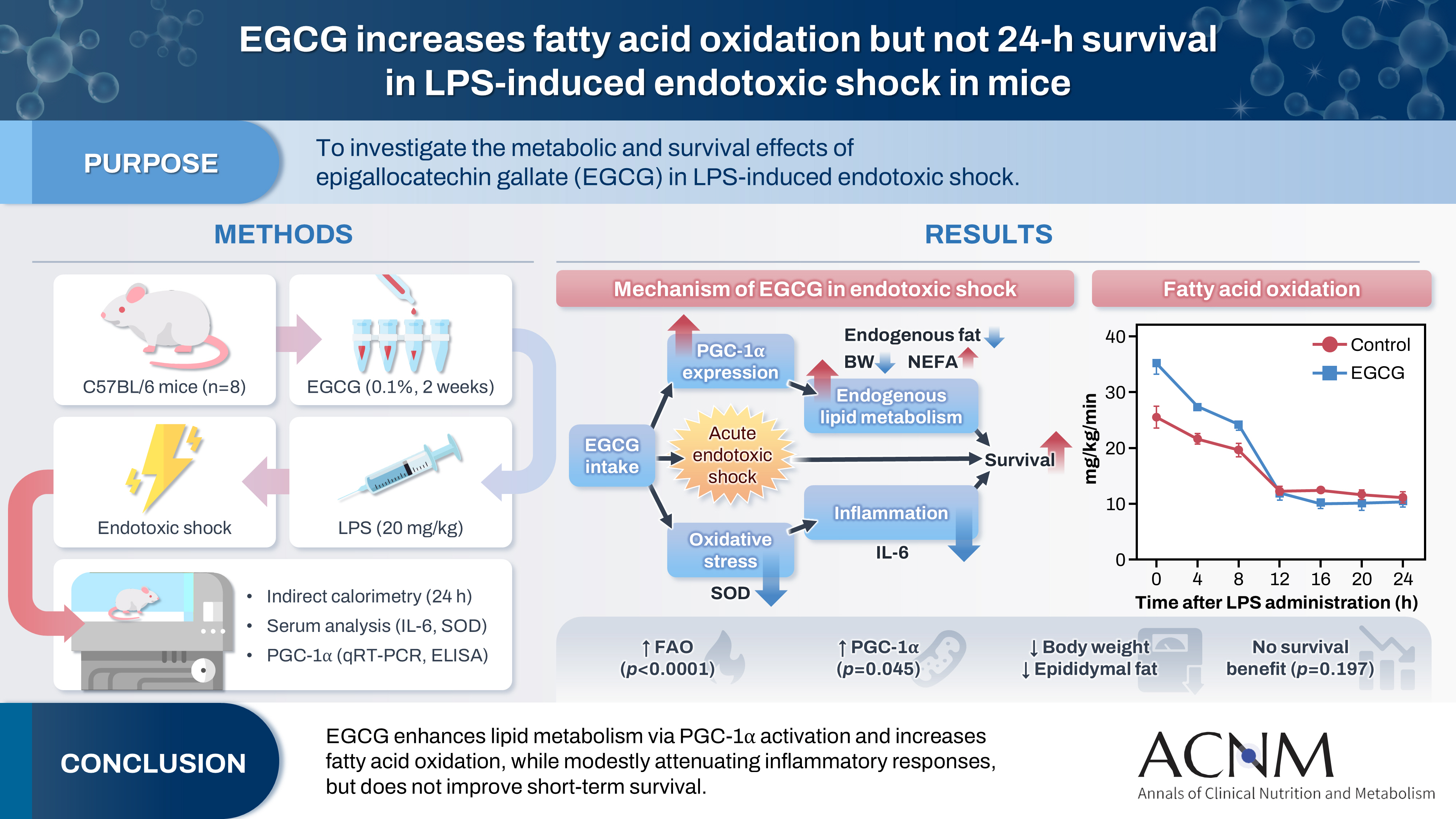
This study aimed to explore the effects of epigallocatechin gallate (EGCG) in critically ill patients using a mouse model.
Methods
C57BL/6 mice were divided into control and EGCG groups (n=8 per group). The EGCG group received a 0.1% EGCG solution for 2 weeks, after which the mice were intraperitoneally injected with a lethal dose of lipopolysaccharide to induce acute endotoxic shock. Indirect calorimetry was performed for 24 hours. Changes in body weight, epididymal fat weight, and survival were measured, together with serum lipid levels, interleukin-6 (IL-6), and superoxide dismutase (SOD) concentrations. The expression of peroxisome proliferator-activated receptor gamma coactivator 1-alpha (PGC-1α) was determined using quantitative real-time polymerase chain reaction, and its serum concentration was subsequently measured.
Results
Indirect calorimetry showed a significant increase in fatty acid oxidation (P<0.0001) in the EGCG group, along with significant decreases in body weight and epididymal fat weight (P<0.01 and P<0.05, respectively). Survival did not differ significantly between groups (P=0.197). Serum lipid levels, IL-6, and SOD showed numerical differences, although these differences were not statistically significant. Furthermore, hepatic PGC-1α expression showed a tendency toward upregulation, and serum PGC-1α levels were significantly higher (P<0.05).
Conclusion
EGCG stimulates endogenous lipid metabolism through PGC-1α activation and may suppress inflammatory responses; therefore, it may represent a potentially useful nutrient for acute nutritional therapy.
- 2,541 View
- 26 Download

Guideline
- A practical guide for enteral nutrition from the Korean Society for Parenteral and Enteral Nutrition: Part II. selection and initiation of enteral feeding routes
-
Ja Kyung Min
 , Ye Rim Chang
, Ye Rim Chang , Bo-Eun Kim
, Bo-Eun Kim , In Seok Lee
, In Seok Lee , Jung Mi Song
, Jung Mi Song , Hyunjung Kim
, Hyunjung Kim , Jae Hak Kim
, Jae Hak Kim , Kyung Won Seo
, Kyung Won Seo , Sung Shin Kim
, Sung Shin Kim , Chi-Min Park
, Chi-Min Park , Jeongyun Park
, Jeongyun Park , Eunjung Kim
, Eunjung Kim , Eunmi Sul
, Eunmi Sul , Sung-Sik Han
, Sung-Sik Han , Jeong Wook Kim
, Jeong Wook Kim , Seungwan Ryu
, Seungwan Ryu , Minji Seok
, Minji Seok , Jinhee Yoon
, Jinhee Yoon , Eunhee Kong
, Eunhee Kong , Youn Soo Cho
, Youn Soo Cho , Jeong Meen Seo
, Jeong Meen Seo , for KSPEN Enteral Nutrition Committee
, for KSPEN Enteral Nutrition Committee - Ann Clin Nutr Metab 2025;17(3):165-171. Published online December 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0037
-
 Abstract
Abstract
 PDF
PDF - Purpose
We developed evidence-based recommendations for selecting and initiating the enteral nutrition (EN) delivery route in adult and pediatric patients to improve safety and standardize practice in Korea.
Methods
Key questions covered feeding tube selection, methods to verify tube placement, confirmation in pediatric patients, and timing of EN following percutaneous endoscopic gastrostomy (PEG). Recommendations were drafted and refined through multidisciplinary expert consensus under the Korean Society for Parenteral and Enteral Nutrition (KSPEN).
Results
Feeding tube selection should be based on gastrointestinal anatomy, function, and expected EN duration. Short-term feeding is recommended with nasogastric or orogastric tubes, whereas long-term feeding should use percutaneous or surgical routes such as PEG. Tube position must always be verified before use, preferably with radiography or pH testing; auscultation alone is unreliable and should not be used. In pediatric patients, radiographic confirmation remains the gold standard, although pH testing and insertion-length assessment may be considered when imaging is not feasible. After PEG, EN can be initiated safely within 4 hours in both adults and children without increasing complications if trained staff monitor for leakage or infection.
Conclusion
This guideline offers a structured framework for safe and timely EN tailored to patient characteristics. Early verification and multidisciplinary collaboration help reduce complication, improving outcomes of EN therapy.
- 1,895 View
- 91 Download

Reviews
- Definition, assessments, and current research on sarcopenia in children: a narrative review
-
Min-Jung Bang

- Ann Clin Nutr Metab 2024;16(2):49-56. Published online August 1, 2024
- DOI: https://doi.org/10.15747/ACNM.2024.16.2.49
-
 Abstract
Abstract
 PDF
PDF - Purpose: Sarcopenia is a well-established prognostic factor for the clinical outcomes of adult patients with cancer and chronic diseases and correlates with increased intensive care unit admissions and prolonged hospital stays. However, research on sarcopenia in children is limited due to its undefined criteria and a lack of studies exploring its impact on clinical outcomes.
Current concept: The challenges in pediatric sarcopenia research include the absence of standardized body composition methods to quantify muscle mass and muscular function, as well as inconsistencies in definitions. Additionally, there is a lack of age- and gender-specific normative data, particularly for young children and infants. Most studies also lack assessments of muscle function, which can lead to bias and misclassification of sarcopenia. The field is further hindered by poor study quality, limited outcome-focused research, and a dearth of longitudinal data. While some studies suggest that various diseases can affect children’s lean muscle mass, few have linked changes in muscle mass to clinical outcomes.
Conclusion: The existing literature on pediatric sarcopenia and its relationship with medical and surgical outcomes is sparse and indicates poorer outcomes associated with sarcopenia. Although extensive research has established a link between sarcopenia and adverse outcomes in adults, information on its impact in pediatric populations remains scarce. Further studies are needed to elucidate the association between muscle mass and outcomes in pediatric surgical patients. -
Citations
Citations to this article as recorded by- Newer Insights on the Occurrence of Sarcopenia in Pediatric Patients with Cancer: A Systematic Review of the Past 5 Years of Literature
Georgios Kiosis, Despoina Ioannou, Kanellos Skourtsidis, Vasilis Fouskas, Konstantinos Stergiou, Dimitrios Kavvadas, Theodora Papamitsou, Sofia Karachrysafi, Maria Kourti
Cancers.2025; 17(19): 3188. CrossRef
- Newer Insights on the Occurrence of Sarcopenia in Pediatric Patients with Cancer: A Systematic Review of the Past 5 Years of Literature
- 5,660 View
- 117 Download
- 1 Crossref

- Postoperative gut dysbiosis and its clinical implications, with an emphasis on probiotic strategies in gastric cancer patients undergoing gastrectomy: a narrative review
-
Cheong Ah Oh

- Ann Clin Nutr Metab 2025;17(2):114-124. Published online August 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0023
-
 Abstract
Abstract
 PDF
PDF - Purpose
This review explores alterations in gut microbiota following gastrointestinal surgery, with a focus on gastrectomy for gastric cancer, and evaluates the therapeutic potential of probiotics in restoring microbial balance and reducing postoperative complications, including infections, inflammation, immune dysfunction, and cancer recurrence.
Current concept
Gastrointestinal surgery disrupts gut microbial homeostasis via surgical stress, oxygen exposure, altered bile flow, and perioperative antibiotic use. Gastrectomy, in particular, induces marked changes in the microbiota, including increased oral-origin and aerotolerant bacteria, decreased short-chain fatty acid–producing species, and elevated bile acid-transforming organisms. These alterations contribute to complications such as small intestinal bacterial overgrowth, surgical site infections, postoperative ileus, nutrient malabsorption, and potentially a higher risk of colorectal cancer. Probiotics—especially strains of Lactobacillus, Bifidobacterium, and Clostridium—have demonstrated beneficial effects by modulating the gut ecosystem, enhancing epithelial barrier integrity, and regulating immune and metabolic pathways. Randomized clinical trials support using probiotics in improving gastrointestinal recovery, reducing systemic inflammation, restoring microbial diversity, and shortening hospital stays after gastrectomy. Multi-strain probiotic formulations, particularly when administered perioperatively, show the greatest promise. However, safety concerns remain, especially for immunocompromised or critically ill patients, underscoring the need for rigorous clinical oversight and adherence to regulatory standards such as the European Food Safety Authority’s Qualified Presumption of Safety guidelines.
Conclusion
Postoperative dysbiosis is a modifiable factor in adverse surgical outcomes. Probiotic supplementation offers promising therapeutic potential in patients undergoing gastrectomy, though optimal strains, dosing, and timing remain to be determined. Tailored, evidence-based strategies may ultimately enhance both recovery and long-term outcomes after gastric cancer surgery. -
Citations
Citations to this article as recorded by- Interactions Between the Human Microbiome and Surgical Practice
Julia Kalinowski, Nada Nasr, Angelina Colamarino, Michelle Marie Esposito
Hygiene.2026; 6(1): 10. CrossRef - How gut microbiota modulate anesthetic drug response and perioperative outcomes
Dawei Wang
Drug Metabolism Reviews.2026; 58(2): 170. CrossRef - Meta-analysis of efficacy of probiotics in reducing postoperative infections and improving outcomes in gastrointestinal surgery
Muhammad Shamim
Frontiers in Surgery.2026;[Epub] CrossRef
- Interactions Between the Human Microbiome and Surgical Practice
- 11,193 View
- 81 Download
- 3 Crossref

- Pathogenesis, risk factors, and management of postoperative delayed gastric emptying after distal gastrectomy: a narrative review
-
Cheong Ah Oh

- Ann Clin Nutr Metab 2025;17(1):9-17. Published online April 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0007
-
 Abstract
Abstract
 PDF
PDF - Purpose
This narrative review elucidates the complex pathogenesis, key risk factors, and effective management strategies for postoperative delayed gastric emptying (DGE) following distal gastrectomy with D2 lymphadenectomy, a definitive procedure for middle and lower gastric cancer. It also explores opportunities for improved prevention and innovative treatment options.
Current concept
DGE significantly disrupts gastric motility and presents with symptoms such as early satiety, postprandial fullness, nausea, vomiting, and gastric atony. Although rarely fatal, DGE hampers oral intake, prolongs hospital stays, and diminishes quality of life. Current evidence indicates that DGE is a multifactorial disorder resulting from an interplay of vagal nerve disruption, damage to smooth muscle and interstitial cells of Cajal, imbalances in gastrointestinal hormones, and postoperative gut microbiome dysbiosis. Patient-specific factors, including advanced age, poor nutritional status, diabetes, and preoperative pyloric obstruction, along with surgical factors (most notably Billroth II reconstruction), further increase the risk of DGE. Management involves dietary modifications, prokinetic agents (such as metoclopramide and selective 5-HT4 agonists like prucalopride), and gastric decompression.
Conclusion
DGE is a challenging complication following gastrectomy that demands a deeper understanding of its underlying mechanisms to improve patient outcomes. Emerging therapies, including microbiota modulation and advanced pharmacological agents, offer promising new treatment avenues. -
Citations
Citations to this article as recorded by- Feasibility of embryonic-natural orifice transluminal endoscopic surgery for submucosal tumors with mucosal preservation in beagle model
Han Lin, Chuan-Shen Jiang, Dong-Gui Hong, Long-Ping Chen, Yan Zhuang, Wen Lin, Zan-Xuan Qiu, Xin-Yi Zheng, Meng-Yao Xu, Li-Li Wu, Yang-Xin Xie, Wen Wang, Xiao-Jian He, Da-Zhou Li
Frontiers in Surgery.2026;[Epub] CrossRef
- Feasibility of embryonic-natural orifice transluminal endoscopic surgery for submucosal tumors with mucosal preservation in beagle model
- 12,898 View
- 140 Download
- 1 Crossref

Editorial
- Nutritional therapy for critically ill children
-
Eunju Ha

- Ann Clin Nutr Metab 2024;16(2):21-21. Published online August 1, 2024
- DOI: https://doi.org/10.15747/ACNM.2024.16.2.21
- 3,293 View
- 167 Download

Reviews
- Effectiveness of perioperative rehabilitation and nutrition in esophageal cancer: a narrative review
-
Ryoma Haneda
 , Yuki Sakai
, Yuki Sakai , Kenichi Sekimori
, Kenichi Sekimori , Tomohiro Murakami
, Tomohiro Murakami , Eisuke Booka
, Eisuke Booka , Tomohiro Matsumoto
, Tomohiro Matsumoto , Hirotoshi Kikuchi
, Hirotoshi Kikuchi , Yoshihiro Hiramatsu
, Yoshihiro Hiramatsu , Hiroya Takeuchi
, Hiroya Takeuchi
- Ann Clin Nutr Metab 2026;18(1):18-26. Published online March 30, 2026
- DOI: https://doi.org/10.15747/ACNM.25.0021
-
 Abstract
Abstract
 PDF
PDF - Purpose
Esophageal cancer surgery requires robust perioperative management to reduce its high rate of complications. This review evaluates the clinical utility of comprehensive exercise and nutritional therapy, with a specific focus on initiatives led by the multidisciplinary Hamamatsu Perioperative Care Team (HOPE), established at Hamamatsu University Hospital to optimize patient safety and postoperative recovery outcomes.
Current concept
The HOPE protocol involves a diverse team, including surgeons, nurses, pharmacists, and dietitians, who collaboratively implement a multifaceted perioperative care bundle. These interventions include strict smoking cessation, intensive oral care, and immunonutrition incorporating n-3 fatty acids. A distinctive feature of this program is the integration of patient-reported treatment diaries and wearable fitness tracking devices (WFTs) to visualize daily activity, thereby helping to sustain patient motivation. Preoperative rehabilitation focuses on preventing sarcopenia through combined aerobic and resistance training, while postoperative care emphasizes immediate enteral nutrition and early mobilization. Retrospective analyses demonstrated that HOPE implementation reduced Clavien-Dindo grade III or higher infectious complications, pneumonia and surgical site infections, compared with historical controls. In addition, a propensity score–matched analysis showed that WFT users experienced lower pneumonia rates, shorter hospital stays, and better preservation of nutritional markers, including albumin and transthyretin, during the recovery phase compared with non-users.
Conclusion
The HOPE strategy illustrates that combining standard nutritional support and exercise therapy with digital tools enables individualized rehabilitation. This integrated approach reduces morbidity and preserves function, strongly suggesting that incorporation of wearable technology into established surgical care protocols represents a strategy for improving long-term outcomes in high-risk cancer patients.
- 739 View
- 16 Download

- Bedside support for neurologically impaired patients via nutritional evaluations, swallowing function assessments, and gastrointestinal function tests: a narrative review
-
Daisuke Masui
 , Naoki Hashizume
, Naoki Hashizume , Yoshinori Koga
, Yoshinori Koga , Hiroto Eto
, Hiroto Eto , Hiroki Yoshida
, Hiroki Yoshida , Shotaro Taki
, Shotaro Taki , Takato Aikoh
, Takato Aikoh , Shiori Tsuruhisa
, Shiori Tsuruhisa , Tomohiro Kurahachi
, Tomohiro Kurahachi , Naruki Higashidate
, Naruki Higashidate , Tatsuru Kaji
, Tatsuru Kaji
- Ann Clin Nutr Metab 2026;18(1):10-17. Published online March 30, 2026
- DOI: https://doi.org/10.15747/ACNM.25.0018
-
 Abstract
Abstract
 PDF
PDF - Purpose
Neurologically impaired patients often experience complex challenges in respiratory and nutritional management that may necessitate surgical intervention. Furthermore, some patients admitted to specialized facilities for neurologically impaired individuals do not receive adequate postoperative follow-up after being transferred. Kurume University Hospital has established a system of continuous routine rounds at such facilities. This review aims to describe the rationale, methods, and outcomes of multidisciplinary bedside support, with particular emphasis on nutritional evaluation, swallowing function assessment, and gastrointestinal function testing.
Current concept
Routine collaboration between pediatric surgeons and facility-based pediatricians enables continuous perioperative management. Preoperatively, patient background, nutritional status, and family preferences are recorded through structured communication and shared decision-making tools, such as the Ottawa Personal Decision Guide. During hospitalization, multidisciplinary evaluations include bioelectrical impedance analysis for nutritional assessment, endoscopic and pH impedance testing for swallowing function, and multichannel intraluminal impedance monitoring for gastroesophageal reflux. Postoperatively, periodic facility rounds ensure ongoing evaluation, with repeated assessments guiding nutritional optimization, early complication detection, and timely surgical consultation. This approach provides families and healthcare teams with detailed information on functional outcomes, strengthens trust, and enhances continuity of care. Sustained bedside engagement at facilities for neurologically impaired patients improves pre- and postoperative monitoring, promotes seamless collaboration between institutions, and ensures individualized evaluation of nutrition, swallowing, and gastrointestinal function.
Conclusion
By providing actionable data to families and multidisciplinary teams, this model strengthens shared decision-making and supports long-term outcomes. The system may serve as a framework for integrated perioperative care in similar high-risk patient populations.
- 576 View
- 18 Download

Editorial
- Adapting Enhanced Recovery After Surgery for hepatobiliary and pancreatic surgery: a Korean perspective
-
Sang Hyun Shin

- Ann Clin Nutr Metab 2026;18(1):1-2. Published online March 30, 2026
- DOI: https://doi.org/10.15747/ACNM.26.0043
- 746 View
- 15 Download

Original Articles
- Current practices and challenges in nutrition support team activities, 2025 in Korea: a multicenter cross-sectional descriptive study
-
So Hyun Nam

- Ann Clin Nutr Metab 2025;17(2):97-103. Published online August 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0026
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Purpose
This study aimed to evaluate the current practices, activities, and challenges of nutrition support teams (NSTs) in Korea. The assessment was conducted as part of the 4th NST Leadership Program of the Korean Society of Surgical Metabolism and Nutrition held in 2025, which seeks to foster leadership and enhance team functionality.
Methods
A nationwide survey was conducted in February 2025 among 54 NST members from 44 institutions. The survey explored team composition, consultation volume, educational programs, barriers to implementation, institutional support, and reimbursement challenges.
Results
Of the 44 participating hospitals, most (86.4%) operated a single NST, with multidisciplinary physician involvement from over three specialties in 77.2% of cases. Inpatient referrals to NSTs were generally low, with less than 10% at 63% of institutions. Only 40.9% had an individual office, and formal incentive systems were reported in 18.1% of hospitals. Educational programs for in-hospital staff were limited (29.5%), and less than half conducted regular academic meetings. Rates of adoption of NST recommendations varied widely, with barriers including a lack of engagement from attending physicians, failure to review the recommendations, and department-specific clinical policies. Efforts to promote NST activation included computerized prescription systems, automated referral workflows, staff education, and quality improvement initiatives. Participants focused on sharing effective NST cases, building incentives, exchanging clinical insights, clarifying team roles and leadership, and developing unified practice guidelines.
Conclusion
NSTs in Korea are well established but face ongoing challenges in collaboration and sustainability. Continued leadership and policy support are crucial for enhancing team performance and improving patient outcomes. -
Citations
Citations to this article as recorded by- Perioperative nutritional practices and pediatric nutrition support team implementation in Korea: a cross-sectional study
Dayoung Ko, Honam Hwang, Hee-Beom Yang, Joong Kee Youn, Hyun-Young Kim
Ann Clin Nutr Metab.2025; 17(3): 181. CrossRef
- Perioperative nutritional practices and pediatric nutrition support team implementation in Korea: a cross-sectional study
- 6,653 View
- 105 Download
- 1 Crossref

- Association of soy oil-based lipid injectable emulsion with early body weight loss after minimally invasive esophagectomy in Japan: a retrospective cohort study
-
Tomonori Narita
 , Kazuhiko Fukatsu
, Kazuhiko Fukatsu , Kenichi Kono
, Kenichi Kono , Satoshi Murakoshi
, Satoshi Murakoshi , Reo Inoue
, Reo Inoue , Midori Noguchi
, Midori Noguchi , Nana Matsumoto
, Nana Matsumoto , Shoh Yajima
, Shoh Yajima , Koichi Yagi
, Koichi Yagi , Yoshifumi Baba
, Yoshifumi Baba
- Ann Clin Nutr Metab 2026;18(1):34-43. Published online March 30, 2026
- DOI: https://doi.org/10.15747/ACNM.25.0030
-
 Graphical Abstract
Graphical Abstract
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material 
- Purpose
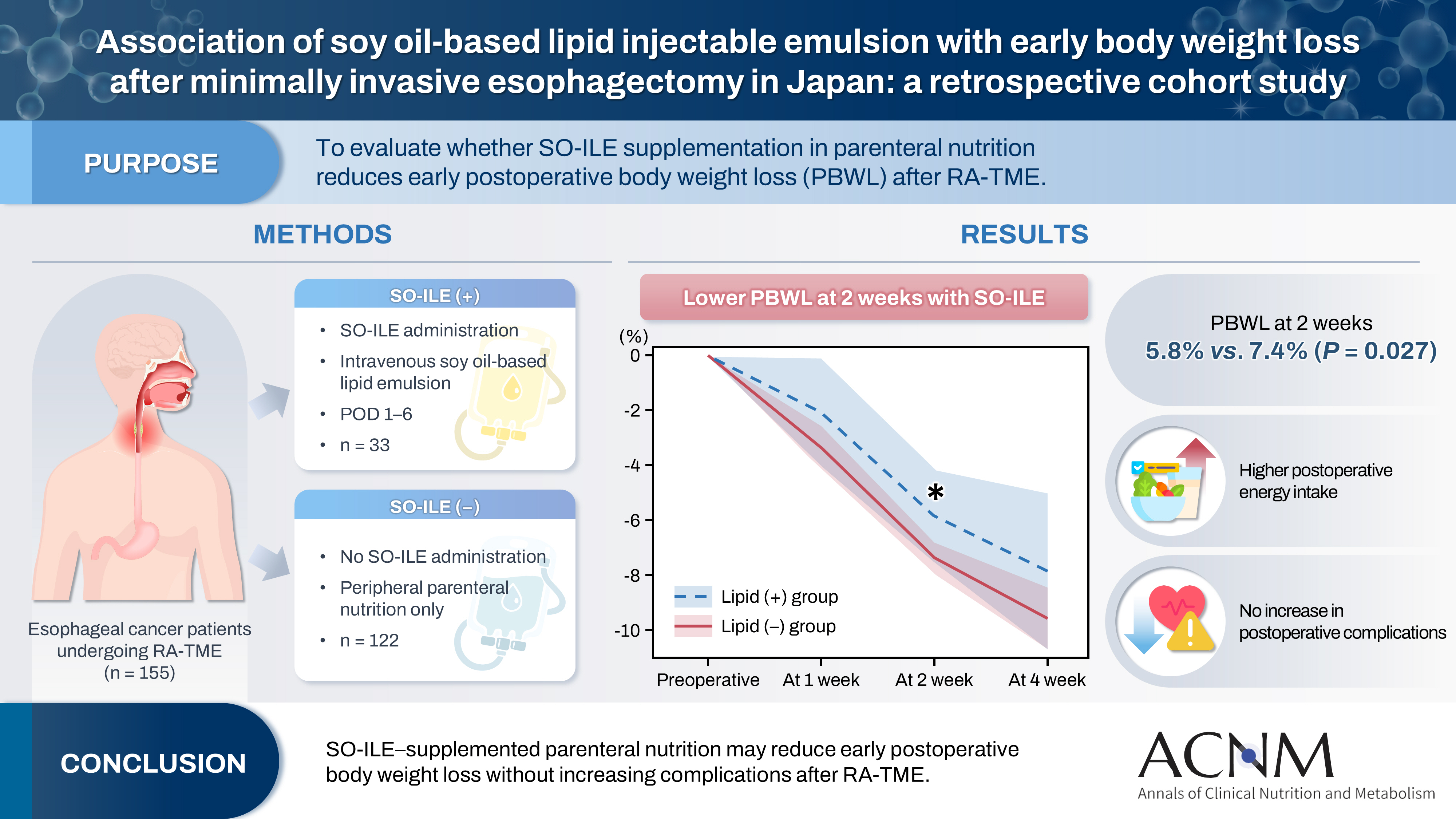
Postoperative body weight loss (PBWL) is associated with poor long-term outcomes following esophagectomy for esophageal cancer, underscoring the critical importance of perioperative nutritional management. Although minimally invasive procedures, such as robot-assisted radical transmediastinal esophagectomy (RA-TME), have become increasingly prevalent, perioperative nutritional strategies have received comparatively limited attention. This study evaluated the impact of soy oil-based injectable lipid emulsion (SO-ILE) on PBWL in patients undergoing RA-TME.
Methods
We retrospectively analyzed 155 patients who underwent RA-TME for esophageal or esophagogastric junction cancer at our hospital between 2011 and 2022. Patients were divided into two groups: the lipid (+) group (n=33), which received SO-ILE between postoperative days 1 and 6, and the lipid (–) group (n=122), which did not receive SO-ILE. Oral or enteral nutrition was withheld until postoperative day 6. Nutrient intake, postoperative outcomes, and nutritional status were compared between the two groups.
Results
Patient backgrounds, surgical outcomes, and postoperative complication rates were similar between the two groups. However, patients in the lipid (+) group received significantly greater total energy and nutrient intake. PBWL at 2 weeks after surgery was significantly lower in the lipid (+) group than in the lipid (–) group (5.8% vs. 7.4%; P=0.027). Univariate analysis showed that absence of SO-ILE administration was the only significant risk factor for PBWL greater than 5% at 2 weeks after RA-TME (P=0.038).
Conclusion
SO-ILE may have the potential to mitigate early PBWL after RA-TME.
- 774 View
- 13 Download

Review
- Perioperative nutritional management to improve long-term outcomes in critically ill perioperative organ transplant patients: a narrative review
-
Toshimi Kaido

- Ann Clin Nutr Metab 2025;17(1):18-24. Published online April 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0005
-
 Abstract
Abstract
 PDF
PDF - Purpose
This review examines the significance of perioperative nutritional management in organ transplantation, with a particular focus on liver transplantation. Organ transplant recipients often experience malnutrition and sarcopenia due to nutritional and metabolic abnormalities associated with organ dysfunction. Because transplantation is a highly invasive procedure, optimizing perioperative nutritional care is critical for improving short-term outcomes and reducing postoperative infection-related mortality.
Current concept
Recent clinical investigations have shown that liver transplant recipients, who are frequently afflicted with end-stage liver disease and uncompensated cirrhosis, are particularly vulnerable to protein-energy malnutrition and secondary sarcopenia. Our analysis identified low pre-transplant nutritional status and the absence of preoperative branched-chain amino acid supplementation as independent risk factors for post-transplant sepsis. In response, we developed a customized nutritional therapy protocol that incorporates precise body composition analysis, serial measurements of biochemical markers (including prealbumin, zinc, and the branched-chain amino acid/tyrosine ratio), and targeted supplementation with branched-chain amino acids, zinc acetate, and synbiotics. Early initiation of enteral nutrition coupled with postoperative rehabilitative interventions resulted in improved outcomes. In addition, stratified body composition parameters correlated with survival differences and informed revised transplantation criteria.
Conclusion
Tailored perioperative nutritional management and rehabilitative strategies are essential for improving early postoperative outcomes in liver transplantation. These findings underscore the need for proactive nutritional assessment and intervention, which may represent a breakthrough in transplant prognosis. Future research should refine nutritional protocols and integrate novel biomarkers, while education and interdisciplinary collaboration remain crucial for enhancing transplant outcomes and reducing complications. -
Citations
Citations to this article as recorded by- Strengthening collaboration: introducing the contributions of Japanese Society for Surgical Metabolism and Nutrition to Annals of Clinical Nutrition and Metabolism
Ye Rim Chang
Ann Clin Nutr Metab.2025; 17(2): 95. CrossRef
- Strengthening collaboration: introducing the contributions of Japanese Society for Surgical Metabolism and Nutrition to Annals of Clinical Nutrition and Metabolism
- 5,515 View
- 126 Download
- 1 Crossref

Original Articles
- Development of a pre- and re-habilitation protocol for gastrointestinal cancer surgery
-
Eun Young Kim
 , Jung Hoon Bae
, Jung Hoon Bae , Jiseon Kim
, Jiseon Kim , Eun Joo Yang
, Eun Joo Yang , Sang-Jae Park
, Sang-Jae Park , In Kyu Lee
, In Kyu Lee , on behalf of the Task Force Team for Development and Trial Application of Pre/Rehabilitation Protocol in GI Cancer Surgery
, on behalf of the Task Force Team for Development and Trial Application of Pre/Rehabilitation Protocol in GI Cancer Surgery - Ann Clin Nutr Metab 2025;17(1):25-40. Published online April 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0001
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Purpose
Surgical resection is the primary curative treatment for gastrointestinal (GI) cancer; however, it is associated with high postoperative complication rates and impaired recovery. Frailty, malnutrition, and sarcopenia increase morbidity and mortality, underscoring the need for perioperative rehabilitation programs. Standardized rehabilitation protocols during the perioperative period are currently lacking in Korea. We aimed to develop an evidence-based rehabilitation protocol for GI cancer patients to enhance postoperative outcomes and facilitate clinical implementation.
Methods
A multidisciplinary task force team comprising experts in surgery, clinical nutrition, and rehabilitation medicine conducted a systematic literature search and comprehensive review from 2012 to 2022 to develop a standardized pre- and re-habilitation protocol for GI cancer surgery. The protocol underwent external validation and subsequent refinements before being finalized through expert consensus.
Results
The protocol development process was organized into four consecutive phases: keyword selection, literature review and case report form development, initial protocol drafting, and external validation leading to the final version of the protocol. The final version of the rehabilitation protocol is presented in the main text and included as Supplements.
Conclusion
This protocol provides a standardized clinical guideline based on the latest evidence-based pre- and re-habilitation strategies and is designed for seamless integration into routine clinical practice. By facilitating proactive rehabilitation interventions, it aims to improve outcomes in GI cancer patients who are at high risk of postoperative complications, functional decline, and malnutrition.
- 4,631 View
- 135 Download

- Comparison of efficacy of enteral versus parenteral nutrition in patients after esophagectomy in Malaysia: a prospective cohort study
-
Ramizah Mohd Shariff
 , Sze Chee Tee
, Sze Chee Tee , Shukri Jahit Mohammad
, Shukri Jahit Mohammad , Khei Choong Khong
, Khei Choong Khong
- Ann Clin Nutr Metab 2025;17(1):41-49. Published online April 1, 2025
- DOI: https://doi.org/10.15747/ACNM.24.016
-
 Graphical Abstract
Graphical Abstract
 Abstract
Abstract
 PDF
PDF 
- Purpose
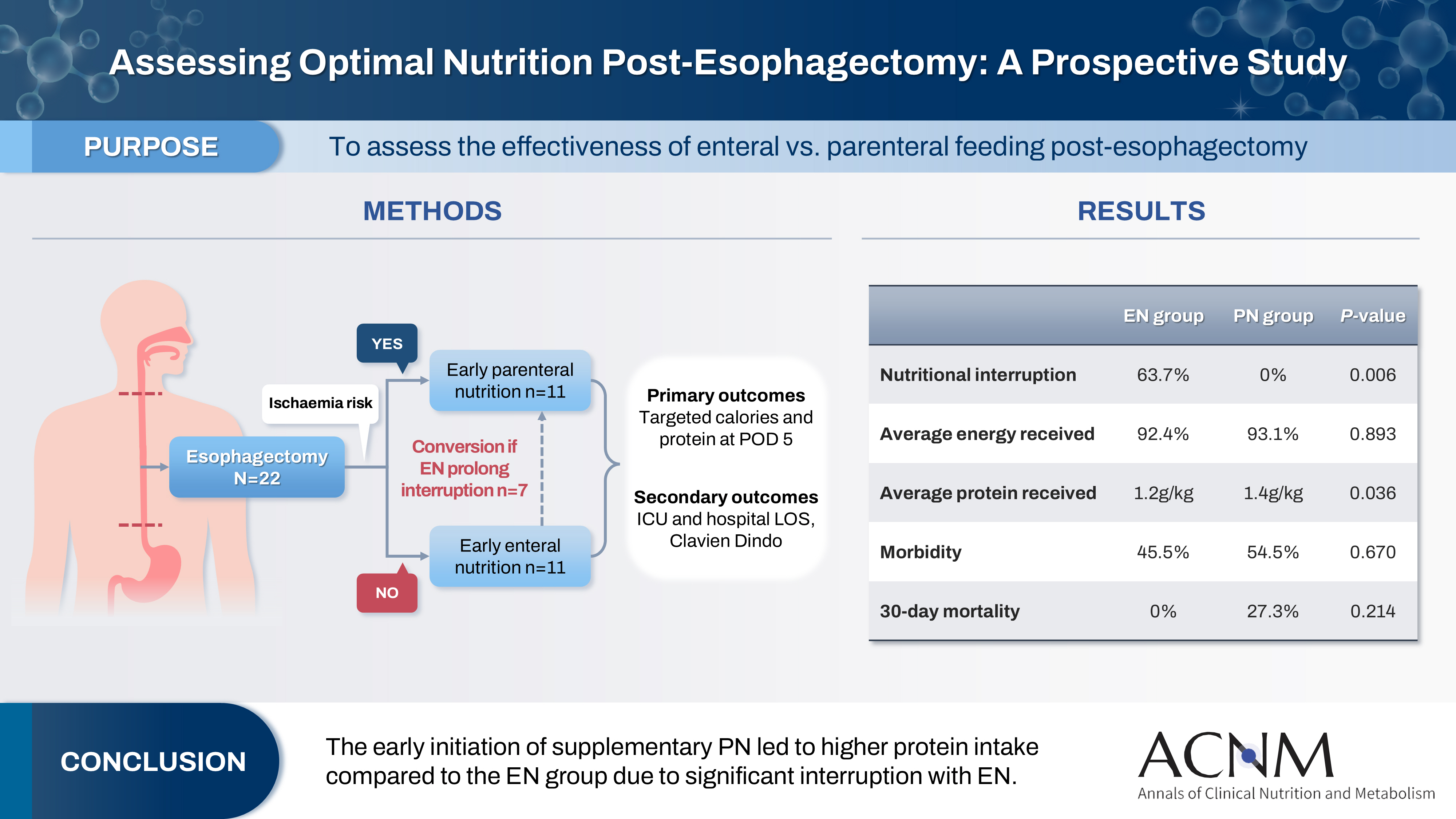
This study aims to assess the effectiveness of enteral versus parenteral feeding in patients after esophagectomy.
Methods
This a prospective cohort study of post-esophagectomy intensive care unit (ICU) patients over 12 months in the National Cancer Institute, Malaysia. Early enteral feeding followed the Enhanced Recovery After Surgery protocol, and parenteral nutrition (PN) was considered if there was a risk for conduit ischemia. It compared the effectiveness of enteral versus PN following esophagectomy, and assessed the correlations between biochemical nutritional markers and hospital lengths of stay or ventilation days.
Results
It included two cohorts receiving PN (n=11) or enteral nutrition (EN) (n=11) following elective esophagectomy. Preoperative weight, body mass index, and Subjective Global Assessment were higher in the EN group (P=0.033, P=0.021, P=0.031, respectively). Nutritional interruption occurred more frequently in the EN group (63.7%) compared to the PN group (P=0.001). Mean levels of energy and protein received were 93.1 kcal/kg and 1.4 g/kg for PN versus 92.4 kcal/kg and 1.2 g/kg for EN (P=0.893, P=0.036). The median lengths of ICU stay (P=0.688) and postoperative stay (P=0.947) between groups showed no significant difference. In addition, 30-day mortality (P=0.214) and other postoperative complications (P>0.05) were comparable in the two groups.
Conclusion
Early initiation of supplementary PN due to significant interruption in EN led to higher protein intake compared to the EN group. However, there were no significant differences in postoperative outcomes, including 30-day mortality, ICU length of stay, and ventilation days. PN ensures adequate nutritional intake, especially in terms of protein delivery, without adversely affecting postoperative recovery and clinical outcomes. -
Citations
Citations to this article as recorded by- Optimizing nutritional support in upper gastrointestinal surgery: A comprehensive review of feeding jejunostomy techniques and outcomes
Ioana Alexandra Prisacariu, Konstantinos Eleftherios Koumarelas, Konstantinos Argyriou, Alexandros Charalabopoulos, Grigorios Christodoulidis
World Journal of Gastrointestinal Surgery.2025;[Epub] CrossRef
- Optimizing nutritional support in upper gastrointestinal surgery: A comprehensive review of feeding jejunostomy techniques and outcomes
- 6,741 View
- 83 Download
- 1 Crossref

- Micronutrient deficiencies in copper, zinc, and vitamin D as predictors of clinical outcomes in critically ill surgical patients in Korea: a retrospective cohort study
-
Jiae Kim
 , Yanghee Jun
, Yanghee Jun , Ye Rim Chang
, Ye Rim Chang , Jong-Kwan Baek
, Jong-Kwan Baek , Hak-Jae Lee
, Hak-Jae Lee , Hyewon Han
, Hyewon Han , Suk-Kyung Hong
, Suk-Kyung Hong
- Ann Clin Nutr Metab 2024;16(3):158-167. Published online December 1, 2024
- DOI: https://doi.org/10.15747/ACNM.2024.16.3.158
-
 Abstract
Abstract
 PDF
PDF - Purpose: To investigate the prevalence of copper, zinc, and vitamin D deficiencies in surgical intensive care unit (SICU) patients and the associations between those deficiencies and clinical outcomes.
Methods: We conducted a retrospective study of 210 patients admitted to the SICU of Asan Medical Center between June 2020 and June 2022. Micronutrient levels were measured within 7 days of SICU admission. Primary outcomes were the mortality rate, length of SICU stay, hospital stay duration, and mechanical ventilation duration.
Results: Copper deficiency was found in 35% (68/193), zinc deficiency in 52% (100/193), and severe vitamin D deficiency in 46% (82/179) of patients. Copper-deficient patients showed a significantly higher mortality rate (25.0% vs. 12.8%, P=0.044), longer hospital stays (57.8±47.0 vs. 45.2±36.6 days, P=0.041), and extended mechanical ventilation duration (26.9±23.3 vs. 18.8±15.7 days, P=0.012). Zinc deficiency was associated with higher C-reactive protein levels (16.2±9.5 vs. 11.5±8.8 mg/dL, P=0.001) and lower prealbumin levels (6.5±2.8 vs. 9.9±5.6 mg/dL, P<0.001). Severe vitamin D deficiency (<10 ng/mL) was not significantly associated with mortality or other clinical outcomes (mortality: <10 ng/mL vs. ≥10 ng/mL, 13% vs. 18%, P=0.583).
Conclusion: Micronutrient deficiencies are prevalent in SICU patients. Copper deficiency significantly correlated with poor clinical outcomes, and zinc deficiency showed a strong association with inflammatory markers. Early assessment and supplementation of micronutrients could be beneficial for critically ill surgical patients.
- 7,182 View
- 85 Download

- Perioperative nutritional practices and pediatric nutrition support team implementation in Korea: a cross-sectional study
-
Dayoung Ko
 , Honam Hwang
, Honam Hwang , Hee-Beom Yang
, Hee-Beom Yang , Joong Kee Youn
, Joong Kee Youn , Hyun-Young Kim
, Hyun-Young Kim
- Ann Clin Nutr Metab 2025;17(3):181-187. Published online December 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0027
-
 Graphical Abstract
Graphical Abstract
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material 
- Purpose
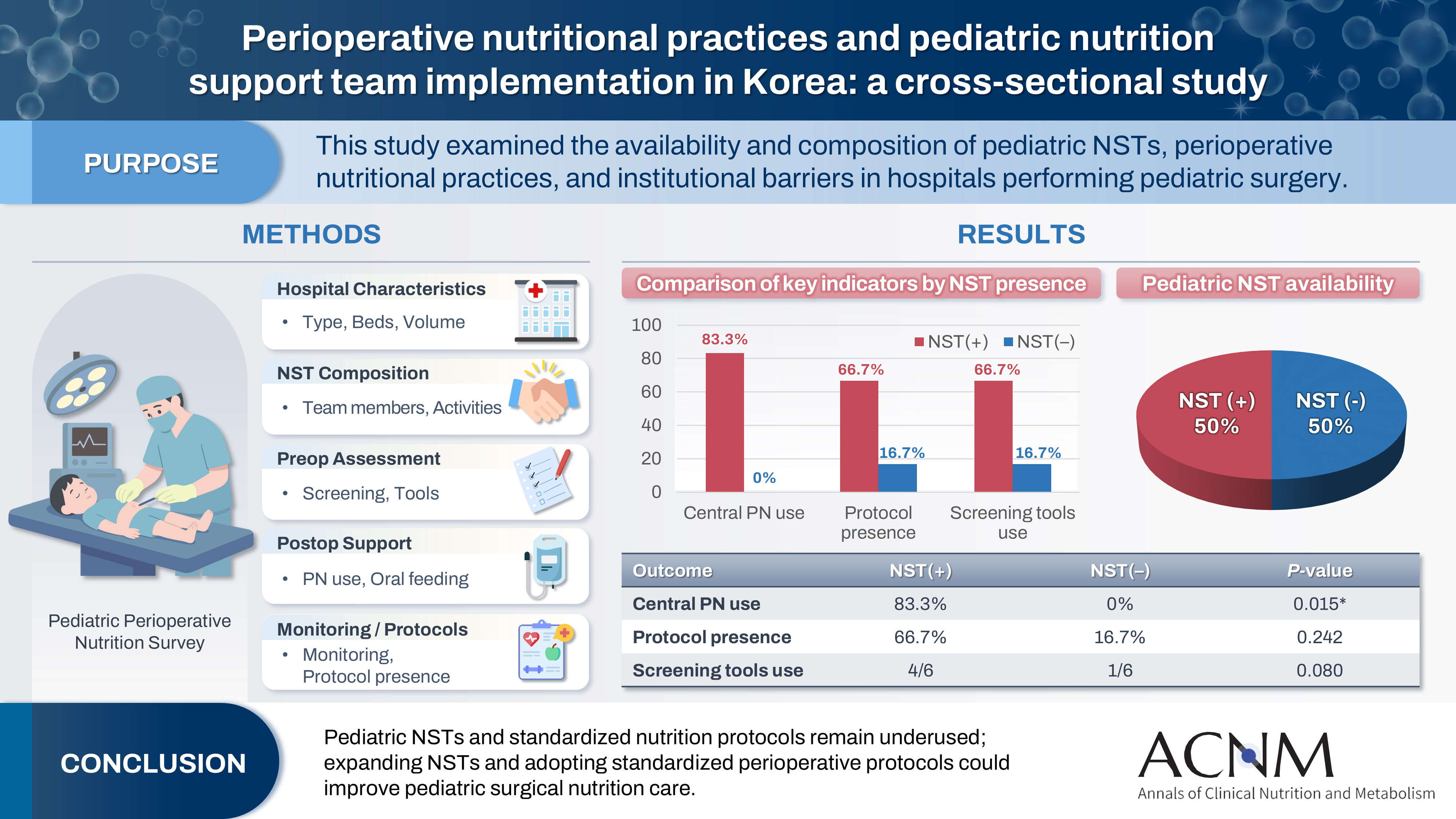
Pediatric surgical patients are vulnerable to perioperative malnutrition, yet standardized nutritional care and structured nutrition support team (NST) involvement remain inconsistent across institutions. Although multidisciplinary nutritional support has gained increasing attention, data on pediatric NST practices within surgical settings in Korea are limited. This study examined the availability and composition of pediatric NSTs, perioperative nutritional practices, and barriers in hospitals performing pediatric surgery.
Methods
A nationwide cross-sectional survey was conducted among tertiary and secondary hospitals that perform pediatric surgery in Korea. The questionnaire assessed hospital characteristics, the presence and composition of pediatric NSTs, perioperative nutritional screening and support practices, monitoring protocols.
Results
A total of 12 hospitals participated. Although all were high-capacity institutions, only half reported having a pediatric NST. Routine preoperative nutritional screening was performed in 50% of hospitals, and validated tools such as Screening Tool for the Assessment of Malnutrition in Pediatrics (STAMP) and Pediatric Yorkhill Malnutrition Score (PYMS) were used in 41.7%. Hospitals with a pediatric NST more frequently had institutional protocols for nutritional evaluation (66.7% vs. 16.7%) and were more likely to administer central venous parenteral nutrition postoperatively (83.3% vs. 0%, P=0.015). Enhanced Recovery After Surgery protocols were implemented in only two hospitals (16.7%). Major barriers to pediatric NST operation included insufficient staffing and time constraints.
Conclusion
Pediatric NSTs and standardized perioperative nutrition protocols remain underutilized in Korean surgical centers. Institutions with a pediatric NST demonstrated more structured nutritional practices. Expanding NST infrastructure and establishing standardized perioperative protocols for pediatric surgical patients may enhance the quality and consistency of nutritional care.
- 2,215 View
- 39 Download

Editorial
- Bridging evidence and clinical practice: a practical guide for enteral nutrition from the Korean Society for Parenteral and Enteral Nutrition
-
Suk-Kyung Hong

- Ann Clin Nutr Metab 2025;17(1):1-2. Published online April 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0008
- 2,907 View
- 97 Download

Original Articles
- Current status and short-term results regarding frailty in patients undergoing gastrointestinal cancer resection in Japan: a retrospective cohort study
-
Asuka Yasueda
 , Junichi Nishimura
, Junichi Nishimura , Seiji Ikeda
, Seiji Ikeda , Naotsugu Haraguchi
, Naotsugu Haraguchi , Hirofumi Akita
, Hirofumi Akita , Hiroshi Wada
, Hiroshi Wada , Chu Matsuda
, Chu Matsuda , Takeshi Omori
, Takeshi Omori , Masayoshi Yasui
, Masayoshi Yasui , Hironari Tamiya
, Hironari Tamiya , Hideaki Tahara
, Hideaki Tahara , Hiroshi Miyata
, Hiroshi Miyata
- Ann Clin Nutr Metab 2026;18(1):54-62. Published online March 30, 2026
- DOI: https://doi.org/10.15747/ACNM.25.0013
-
 Graphical Abstract
Graphical Abstract
 Abstract
Abstract
 PDF
PDF 
- Purpose
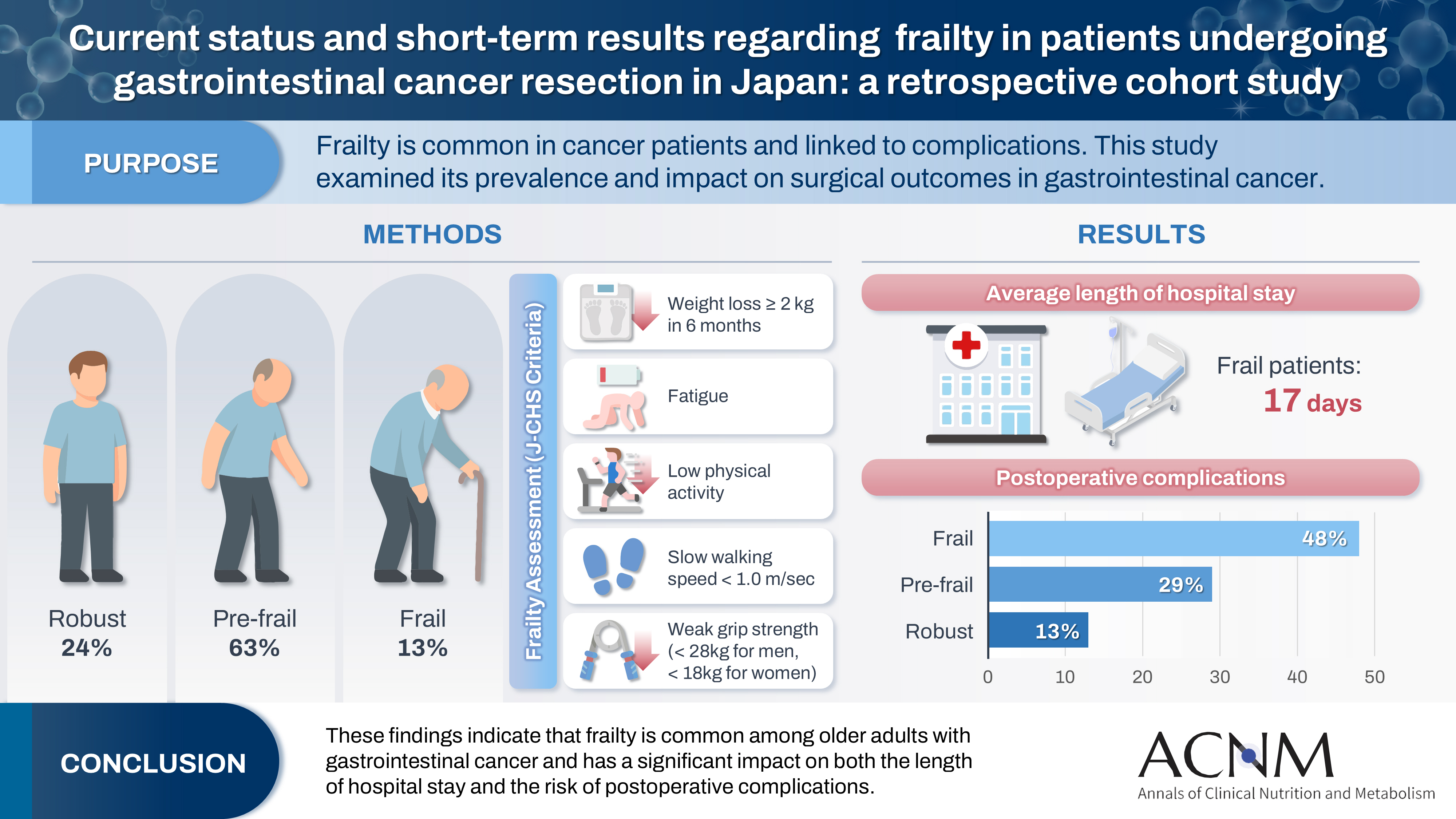
Frailty is a state of physical and cognitive decline that exists between robust health and the need for nursing care. Frailty is reported to occur at a high rate among patients with cancer and is associated with postoperative complications, such as delirium, infection, reduced survival, and rehospitalization. In this study, we investigated the incidence of frailty and surgical outcomes in patients who underwent surgery for gastrointestinal cancer.
Methods
A total of 201 patients who underwent preoperative physical assessment at Osaka International Cancer Institute between July and September 2021 were included. The Japanese version of the Cardiovascular Health Study (J-CHS) index was used to assess the frequency of frailty and related postoperative outcomes.
Results
Among the 201 patients, 27 (13%) were classified as frail and 126 (63%) as pre-frail. Of the 27 frail patients, 22 (81%) were older adults—a significantly higher proportion compared to the pre-frail/robust group (P=0.004). The median hospital stay for frail patients was 17 days (range, 5–98 days), which was significantly longer than that for robust patients (P<0.001). Postoperative complications occurred in 13 frail patients (48%), which was higher than in pre-frail (n=36, 29%) and robust (n=6, 13%) patients. Furthermore, multivariate analysis showed that frailty was an independent risk factor for postoperative complications.
Conclusion
These findings indicate that frailty is common among older adults with gastrointestinal cancer and has a significant impact on both the length of hospital stay and the risk of postoperative complications.
- 676 View
- 10 Download

- Impact of postoperative nutritional status on the patients’ clinical outcomes and knee biomechanics following total knee arthroplasty in Japan: a prospective cohort study
-
Kenichi Kono
 , Tetsuya Tomita
, Tetsuya Tomita , Takaharu Yamazaki
, Takaharu Yamazaki , Masashi Tamaki
, Masashi Tamaki , Shuji Taketomi
, Shuji Taketomi , Ryota Yamagami
, Ryota Yamagami , Reo Inoue
, Reo Inoue , Yuki Taniguchi
, Yuki Taniguchi , Sakae Tanaka
, Sakae Tanaka , Kazuhiko Fukatsu
, Kazuhiko Fukatsu
- Ann Clin Nutr Metab 2025;17(1):50-57. Published online April 1, 2025
- DOI: https://doi.org/10.15747/ACNM.24.019
-
 Graphical Abstract
Graphical Abstract
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material 
- Purpose
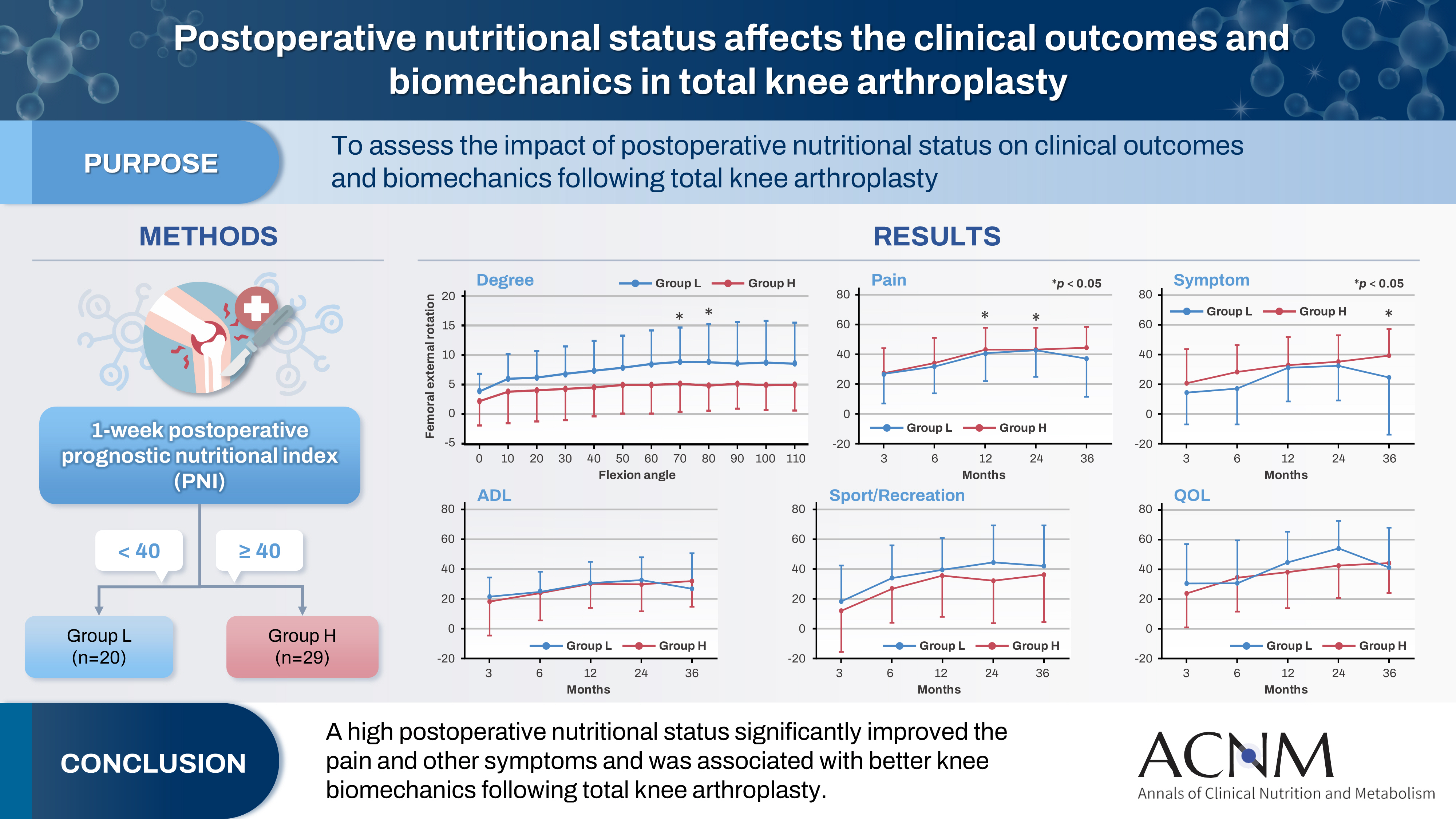
The impact of postoperative nutritional status on clinical outcomes and biomechanics following total knee arthroplasty remains largely unknown. This study aimed to assess this question using the prognostic nutritional index to evaluate the nutritional status of orthopedic participants.
Methods
Patients with knee osteoarthritis who underwent total knee arthroplasty (n=49) in Japan were divided into two groups based on their 1-week postoperative prognostic nutritional index. Group L patients had a prognostic nutritional index <40, whereas Group H comprised patients with a prognostic nutritional index ≥40. Postoperative improvements in Knee Injury and Osteoarthritis Outcome Score were evaluated. The patients performed squats under single-fluoroscopic surveillance in the sagittal plane for biomechanical evaluation. A two-dimensional/three-dimensional registration technique was employed to measure the tibiofemoral kinematics. The axial rotation of the femoral component relative to the tibial component and the anteroposterior translation of the medial and lateral femorotibial contact points were measured.
Results
Group H showed significantly higher pain scores than Group L at 12 and 36 months postoperatively and a significantly higher symptom score at 36 months postoperatively. The kinematic comparison revealed that the axial external rotation in Group L was larger than that in Group H from 70° to 80° with flexion. Moreover, in the medial anteroposterior translation, Group L was more anteriorly located than Group H, with flexion beyond 30°.
Conclusion
The results suggest that a high postoperative nutritional status significantly improved pain and other symptoms and was associated with better knee biomechanics following total knee arthroplasty.
- 3,935 View
- 53 Download

Editorial
- A comprehensive overview of enhanced recovery after surgery
-
Sang Hyun Shin

- Ann Clin Nutr Metab 2024;16(1):1-2. Published online April 1, 2024
- DOI: https://doi.org/10.15747/ACNM.2024.16.1.1
-
 PDF
PDF -
Citations
Citations to this article as recorded by- Effects of an Early Promoting Mobility Program on Postoperative Recovery Outcomes in People with Critical Illness after Major Abdominal Surgery: A Quasi-experimental Study
Tarrana Termkunanon, Piyawan Pokpalagon, Suchira Chaiviboontham
Pacific Rim International Journal of Nursing Research.2025; 29(4): 696. CrossRef
- Effects of an Early Promoting Mobility Program on Postoperative Recovery Outcomes in People with Critical Illness after Major Abdominal Surgery: A Quasi-experimental Study
- 6,329 View
- 72 Download
- 1 Crossref

Review
- Improving the usability of lipid emulsions and optimizing their user-friendliness: a narrative review
-
Keisuke Kubota
 , Natsuko Ichikawa
, Natsuko Ichikawa , Kazuhiro Isoda
, Kazuhiro Isoda , Misato Enomoto
, Misato Enomoto , Miyoko Kosugi
, Miyoko Kosugi , Mari Tanabe
, Mari Tanabe , Naoya Sakuraba
, Naoya Sakuraba , Sayuri Endo
, Sayuri Endo , Atsushi Suzuki
, Atsushi Suzuki , Masanori Hashimoto
, Masanori Hashimoto
- Ann Clin Nutr Metab 2025;17(2):104-113. Published online August 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0015
-
 Abstract
Abstract
 PDF
PDF - Purpose
Reluctance to administer lipid emulsions to patients receiving treatment, or as recommended by a nutritional support team, often stems from various restrictions or concerns about potential adverse effects. This paper aims to discuss the appropriate clinical use of lipid emulsions to enhance both patient safety and convenience.
Current concept
We conducted a literature review to assess the importance of nutritional therapy and nutritional intervention, the advantages and disadvantages of lipid-emulsion administration, the current situation in Japan, and differences between lipid formulations. Here, we address issues regarding lipid-emulsion use, including: administration rate, drug mixing, administration in critically ill patients, and early postoperative use. Our findings suggest the following solutions to each issue: although a rate below 0.1 g/kg/hr is generally recommended, faster administration is possible if needed, depending on the case; administration via a piggy tube to basic infusion formulations is unproblematic; second- and third-generation fat emulsions are safe for critically ill patients, though soybean oil should be used with caution; and while fat emulsion administration is feasible immediately after surgery, due to endogenous energy mobilization, it is preferable to initiate administration from the third to fourth postoperative day.
Conclusion
The provisional conclusions of this study are as follows: the introduction of medium-chain triglyceride formulations and fish oil (second- and third-generation lipid emulsions), which are not yet available in Japan, is urgently needed; and individualized administration is essential due to substantial interindividual variability in lipid emulsion usage. -
Citations
Citations to this article as recorded by- Impact of soybean oil lipid emulsion on clinical outcomes in critically ill pediatric patients
Yuki Yamano, Yoshiyuki Shimizu, Yu Inata, Takeshi Hatachi, Yuri Etani
Clinical Nutrition ESPEN.2026; 72: 102907. CrossRef
- Impact of soybean oil lipid emulsion on clinical outcomes in critically ill pediatric patients
- 6,816 View
- 51 Download
- 1 Crossref

Original Article
- Successful introduction of ERAS in pancreaticoduodenectomy: what is real minimally invasive surgery?
-
Toshimi Kaido
 , Yosuke Miyachi
, Yosuke Miyachi , Koichiro Mitsuoka
, Koichiro Mitsuoka , Mariko Sambommatsu
, Mariko Sambommatsu
- Ann Clin Nutr Metab 2025;17(2):156-161. Published online August 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0014

-
 Graphical Abstract
Graphical Abstract
 Abstract
Abstract
 PDF
PDF 
- Purpose
The introduction of Enhanced Recovery After Surgery (ERAS) protocols for pancreaticoduodenectomy (PD) has been considered challenging due to factors such as preexisting malnutrition, sarcopenia, the complexity of the surgery, and the high incidence of postoperative complications, including postoperative pancreatic fistula (POPF) and delayed gastric emptying (DGE). This study aimed to determine whether ERAS could be implemented in PD to achieve shorter postoperative hospital stays.
Methods
Our novel approach consists of three components. Preoperatively, we routinely assess patients' muscle strength and nutritional status and initiate exercise and nutritional interventions for those identified with sarcopenia or malnutrition. Intraoperatively, we perform pancreaticojejunostomy using a modified Blumgart’s technique with our stent placement policy and utilize new gastrojejunostomy methods to prevent DGE. Principles of postoperative management are early ambulation, early oral intake, and early drain removal. Since April 2020, we have employed this strategy and retrospectively evaluated its effectiveness. We enrolled 71 consecutive patients who underwent open PD with curative intent. Various surgical outcomes, including postoperative hospital stay, were analyzed.
Results
There were 41 men and 30 women, with a median age of 70 years. Preoperative diagnoses included pancreatic head cancer in 31, distal bile duct cancer in 12, and others. Median intraoperative blood loss was 310 mL. Grade B POPF occurred in four patients (6%). No cases of DGE were observed. The median postoperative hospital stay was 8 days (range, 6–26 days).
Conclusion
We successfully implemented ERAS protocols in PD and achieved a significantly reduced postoperative hospital stay. We propose that this approach is “real minimally invasive surgery," regardless of the surgical technique used.
- 4,735 View
- 29 Download

Interesting image
- Penetration of a nasogastric tube by a stylet during insertion
-
Akihide Takami
 , Haruka Tsuji
, Haruka Tsuji , Kazuya Omura
, Kazuya Omura
- Ann Clin Nutr Metab 2025;17(3):210-211. Published online December 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0029
- 794 View
- 16 Download

Original Articles
- A narrative inquiry into the disease adaptation experience of long-term follow-up patients with short bowel syndrome in Korea
-
Eun-Mi Seol
 , Eunjung Kim
, Eunjung Kim
- Ann Clin Nutr Metab 2025;17(3):188-195. Published online December 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0028
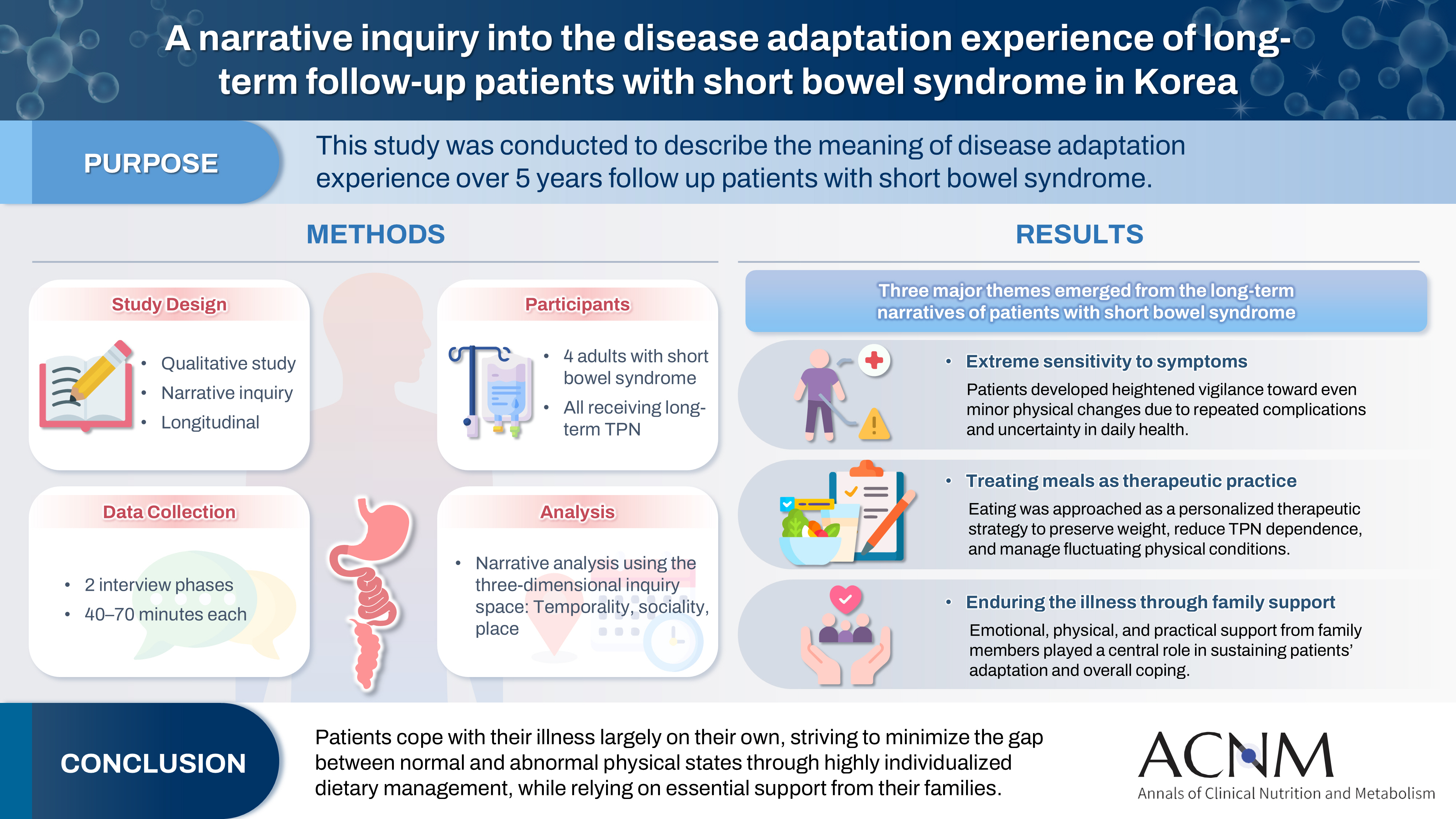
-
 Graphical Abstract
Graphical Abstract
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material 
- Purpose
This study was conducted to describe the meaning of disease adaptation experience over a 5-year long-term follow-up of patients with short bowel syndrome.
Methods
Four patients were recruited from a tertiary hospital in Korea. This study was conducted through first and second interviews from January 2019 to July 2022. The transcribed data were analyzed using narrative methods.
Results
The mean age of the participants was 64 years, and the mean treatment period after small bowel resection was 100 months. The participants lost a mean of 19.3 kg body weight and all were receiving home total parenteral nutrition 2–7 days a week. The meaning of the experience of adapting to the disease for patients was found to be “extremely sensitive to the symptoms,” “considering eating food as another effective treatment method,” and “enduring the disease through family affection.”
Conclusion
Patients are struggling alone to cope with physical symptoms and adapt to their disease. For this, they are doing their best to narrow the gap between normal and abnormal physical conditions by thoroughly implementing diet therapy according to their physical characteristics. This entire process is supported by their families.
- 2,154 View
- 35 Download

- The enteral feeding tube access route in esophageal cancer surgery in Japan: a retrospective cohort study
-
Hiroyuki Kitagawa
 , Keiichiro Yokota
, Keiichiro Yokota , Tsutomu Namikawa
, Tsutomu Namikawa , Kazuhiro Hanazaki
, Kazuhiro Hanazaki
- Ann Clin Nutr Metab 2025;17(1):58-65. Published online April 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0003
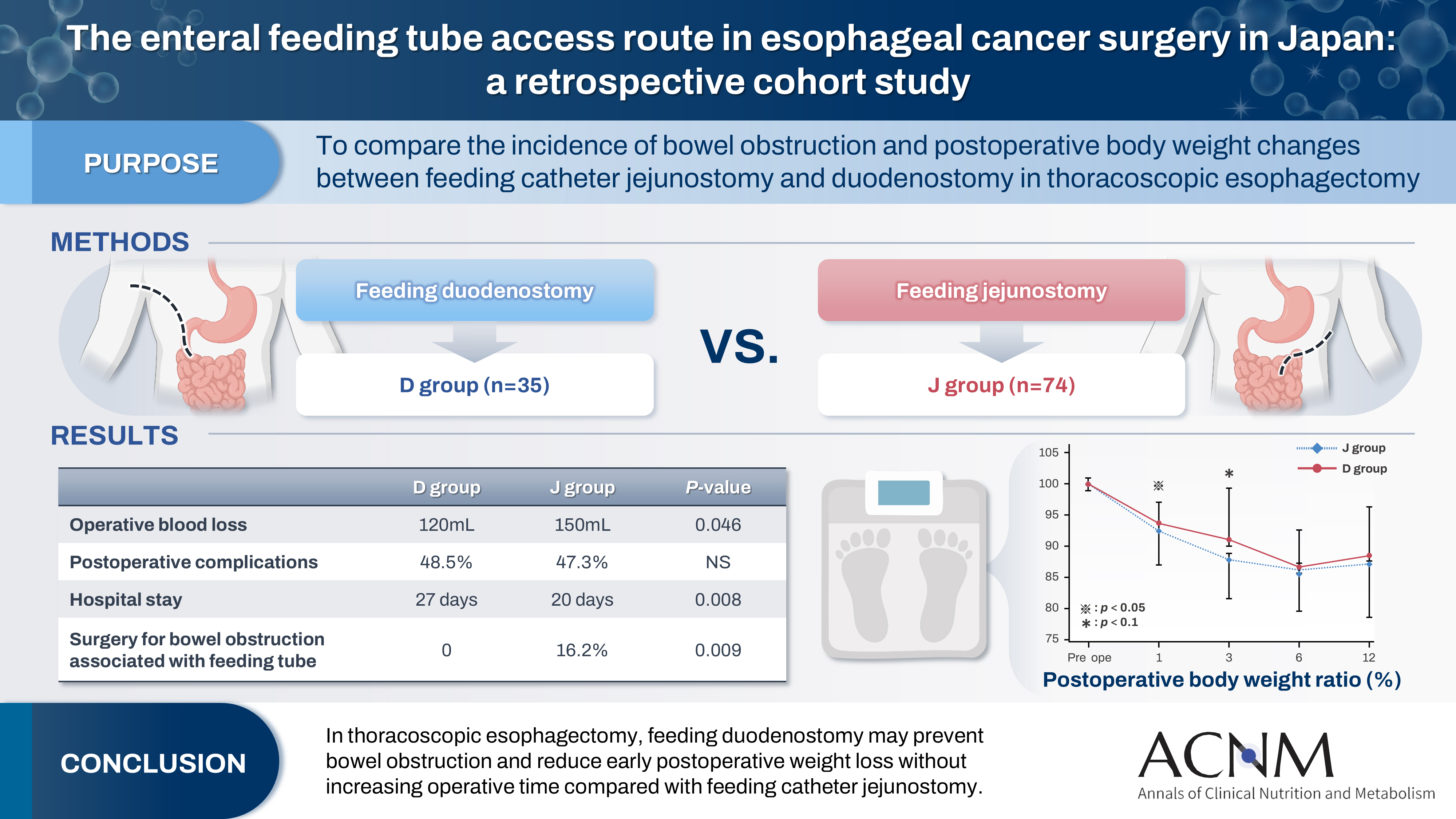
-
 Graphical Abstract
Graphical Abstract
 Abstract
Abstract
 PDF
PDF 
- Purpose
Feeding catheter jejunostomy is a useful access route for early enteral nutrition during esophageal cancer surgery. However, it may lead to postoperative bowel obstruction associated with feeding jejunostomy (BOFJ). To prevent BOFJ, we introduced feeding catheter duodenostomy via the round ligament in 2018. This study aimed to compare the incidence of BOFJ and postoperative body weight changes between feeding catheter jejunostomy and duodenostomy.
Methods
A total of 109 patients who underwent thoracoscopic esophagectomy and gastric tube reconstruction for esophageal cancer at Kochi Medical School Hospital between March 2013 and November 2020 were included. Preoperative patient characteristics (age, sex, preoperative weight, body mass index, cancer stage, and preoperative treatment), surgical outcomes (operative time, blood loss, and postoperative complications [wound infection, pneumonia, anastomotic leakage, BOFJ]), and body weight changes at 1, 3, 6, and 12 months post-surgery were compared between the jejunostomy (J) and duodenostomy (D) groups.
Results
The D group consisted of 35 patients. No significant differences were observed between the groups regarding age, sex, weight, body mass index, cancer stage, operative time, postoperative complications, or duration of tube placement. However, the D group had a significantly lower rate of preoperative chemotherapy (45.7% vs. 78.4%, P=0.001) and lower operative blood loss (120 mL vs. 150 mL, P=0.046) than the J group. All 12 cases of BOFJ occurred in the J group. Furthermore, the D group experienced a significantly lower weight loss ratio at 1 month postoperatively (93.9% vs. 91.8%, P=0.039).
Conclusion
In thoracoscopic esophagectomy, feeding duodenostomy may prevent bowel obstruction and reduce early postoperative weight loss without increasing operative time compared with feeding catheter jejunostomy. -
Citations
Citations to this article as recorded by- Strengthening collaboration: introducing the contributions of Japanese Society for Surgical Metabolism and Nutrition to Annals of Clinical Nutrition and Metabolism
Ye Rim Chang
Ann Clin Nutr Metab.2025; 17(2): 95. CrossRef
- Strengthening collaboration: introducing the contributions of Japanese Society for Surgical Metabolism and Nutrition to Annals of Clinical Nutrition and Metabolism
- 3,901 View
- 41 Download
- 1 Crossref

- Development of a Japanese version of the Short Bowel Syndrome-Quality of Life (SBS-QoL) scale
-
Yuko Tazuke
 , Mayu Suzuki
, Mayu Suzuki , Sae Kikuchi
, Sae Kikuchi , Kaori Ishiguro
, Kaori Ishiguro , Hiroomi Okuyama
, Hiroomi Okuyama
- Ann Clin Nutr Metab 2025;17(2):132-138. Published online August 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0016
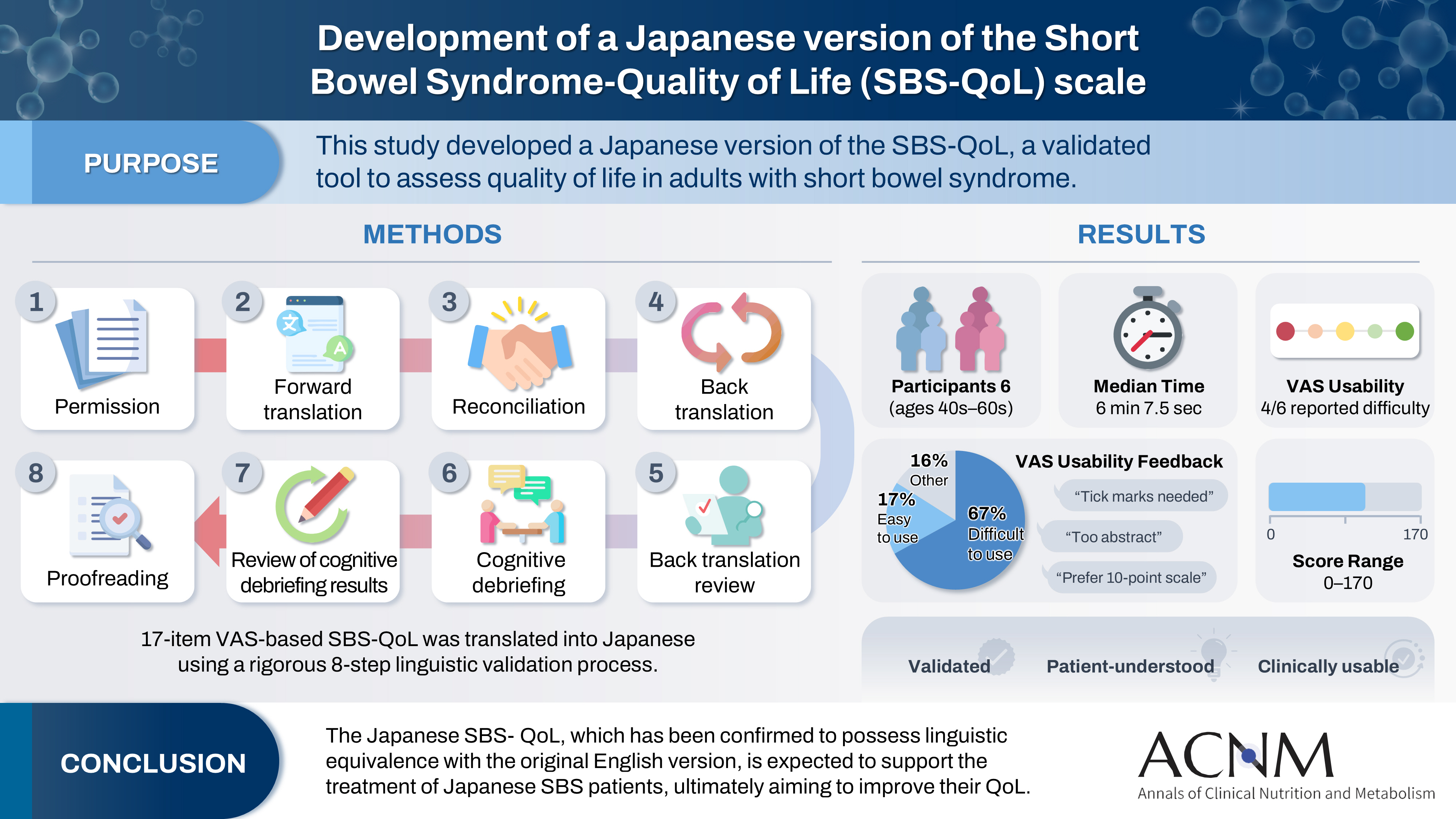
-
 Graphical Abstract
Graphical Abstract
 Abstract
Abstract
 PDF
PDF 
- Purpose
The Short Bowel Syndrome‐Quality of Life (SBS‐QoL) scale is a reliable and sensitive instrument developed to measure and evaluate the quality of life (QoL) in adult patients with short bowel syndrome (SBS). In Japan, increasing attention has been given to the assessment of QoL in patients with SBS; however, no Japanese‐language SBS‐specific scale is currently available. This study aimed to develop a Japanese version of the SBS‐QoL based on the original English version.
Methods
A provisional Japanese version was created in accordance with the guidelines of the International Society for Pharmacoeconomics and Outcomes Research (ISPOR) Task Force, utilizing a process of forward translation, adjustment, and back translation.
Results
Cognitive debriefing using the provisional Japanese version was conducted with six Japanese patients with SBS. Based on these results, the Japanese wording was evaluated and revised, leading to the creation of the final Japanese version.
Conclusion
The Japanese SBS‐QoL, which has been confirmed to possess linguistic equivalence with the original English version, is expected to support the treatment of Japanese SBS patients, ultimately aiming to improve their QoL.
- 4,769 View
- 26 Download

Editorial
- Annals of Clinical Nutrition and Metabolism (ACNM): a new milestone toward global recognition
-
Suk-Kyung Hong

- Ann Clin Nutr Metab 2025;17(3):163-164. Published online December 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0038
- 1,083 View
- 30 Download

Original Articles
- Preprocedural prognostic nutritional index predicts early gastrointestinal symptoms after percutaneous endoscopic gastrostomy or percutaneous radiologic gastrostomy in Korea: a retrospective cohort study
-
Yoonhong Kim
 , Jee Young Lee
, Jee Young Lee , Yeajin Moon
, Yeajin Moon , Seung Hun Lee
, Seung Hun Lee , Kyung Won Seo
, Kyung Won Seo , Ki Hyun Kim
, Ki Hyun Kim
- Ann Clin Nutr Metab 2025;17(3):196-202. Published online December 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0032
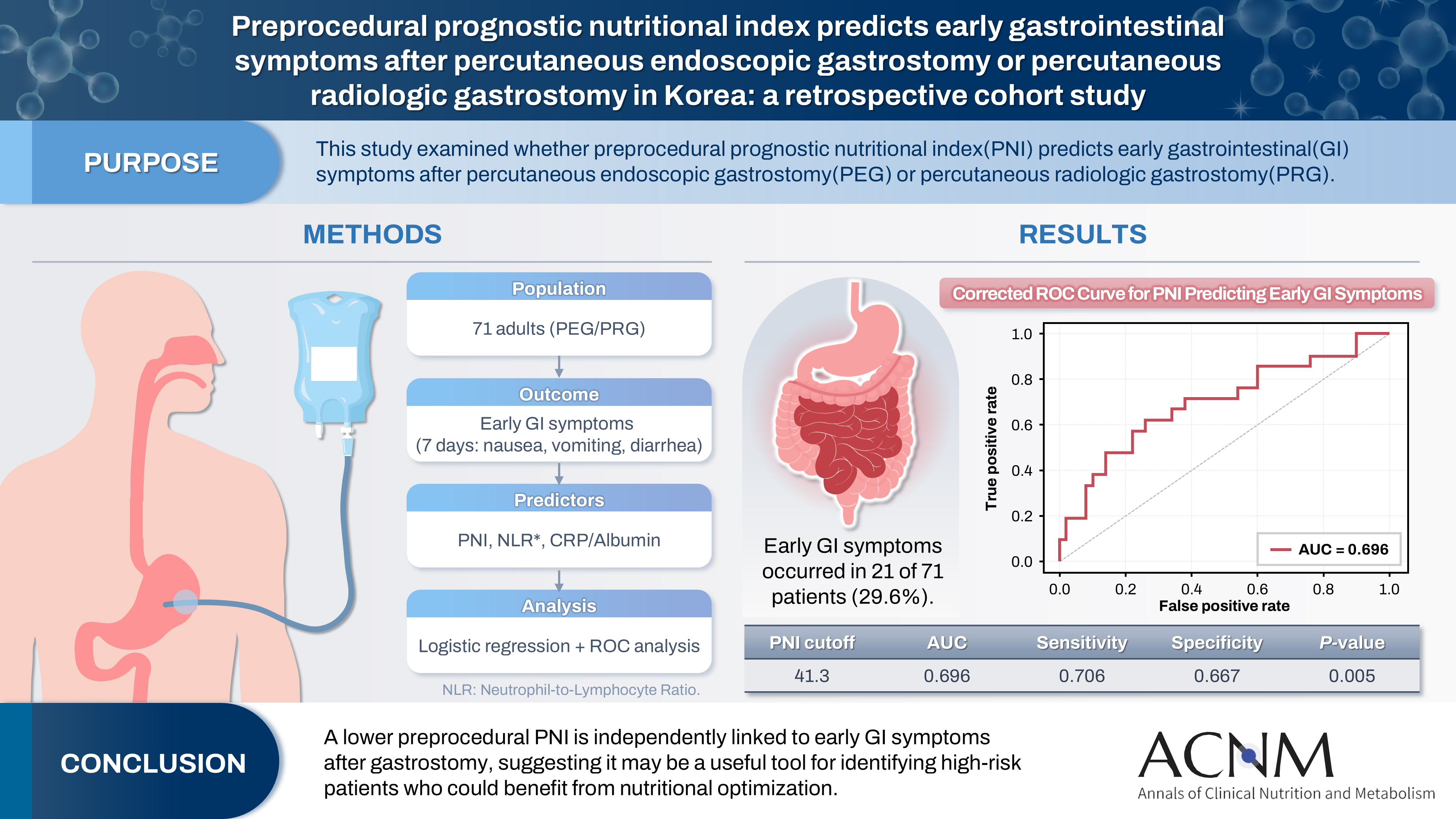
-
 Graphical Abstract
Graphical Abstract
 Abstract
Abstract
 PDF
PDF 
- Purpose
The prognostic nutritional index (PNI) reflects immunonutritional status and is a well-established predictor of surgical outcomes. Although its association with post-gastrostomy mortality has been documented, its relationship with early gastrointestinal (GI) symptoms remains unclear. This study aimed to evaluate whether the preprocedural PNI predicts early GI symptoms following percutaneous gastrostomy, including percutaneous endoscopic gastrostomy (PEG) and percutaneous radiologic gastrostomy (PRG).
Methods
This retrospective study included 71 adults who underwent PEG or PRG. Early GI symptoms, such as nausea, vomiting, and diarrhea, occurring within 7 days were recorded. The preprocedural PNI, neutrophil-to-lymphocyte ratio (NLR), and the C-reactive protein (CRP)-to-albumin ratio were analyzed using logistic regression to identify predictors. Receiver operating characteristic (ROC) analysis was performed to assess the PNI’s discriminative performance.
Results
Early GI symptoms occurred in 21 of 71 patients (29.6%). In univariate analysis, the PNI (P=0.009) and CRP-to-albumin ratio (P=0.018) were significant predictors, whereas NLR was not (P=0.125). After adjustment for potential confounders, including age, sex, body mass index, and NLR, the PNI remained an independent predictor of early GI symptoms (adjusted odds ratio, 0.90; 95% confidence interval, 0.83–0.98; P=0.021). ROC analysis for the PNI produced an area under the curve of 0.696, with an optimal cutoff value of 41.3 (sensitivity 70.6%, specificity 66.7%).
Conclusion
A lower preprocedural PNI is independently associated with the development of early GI symptoms after gastrostomy. The PNI may serve as a practical screening tool to identify high-risk patients who could benefit from preemptive nutritional optimization. -
Citations
Citations to this article as recorded by- Comment on “impact of percutaneous endoscopic gastrostomy (PEG) timing on mortality in intensive care unit patients: The modifying role of the prognostic nutritional index (PNI)”
M. Ganesan, K. Suresh Babu, K. Srinivasa Galu, Ponazhagan
Clinical Nutrition ESPEN.2026; : 103361. CrossRef
- Comment on “impact of percutaneous endoscopic gastrostomy (PEG) timing on mortality in intensive care unit patients: The modifying role of the prognostic nutritional index (PNI)”
- 1,499 View
- 27 Download
- 1 Crossref

- Impact of tube feeding after pancreaticoduodenectomy on nutritional intake and status: a retrospective cohort study in Japan
-
Masaharu Ishida
 , Masahiro Iseki
, Masahiro Iseki , Shuichiro Hayashi
, Shuichiro Hayashi , Aya Noguchi
, Aya Noguchi , Hideaki Sato
, Hideaki Sato , Shingo Yoshimachi
, Shingo Yoshimachi , Akiko Kusaka
, Akiko Kusaka , Mitsuhiro Shimura
, Mitsuhiro Shimura , Shuichi Aoki
, Shuichi Aoki , Daisuke Douchi
, Daisuke Douchi , Takayuki Miura
, Takayuki Miura , Shimpei Maeda
, Shimpei Maeda , Masamichi Mizuma
, Masamichi Mizuma , Kei Nakagawa
, Kei Nakagawa , Takashi Kamei
, Takashi Kamei , Michiaki Unno
, Michiaki Unno
- Ann Clin Nutr Metab 2025;17(3):203-209. Published online December 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0020
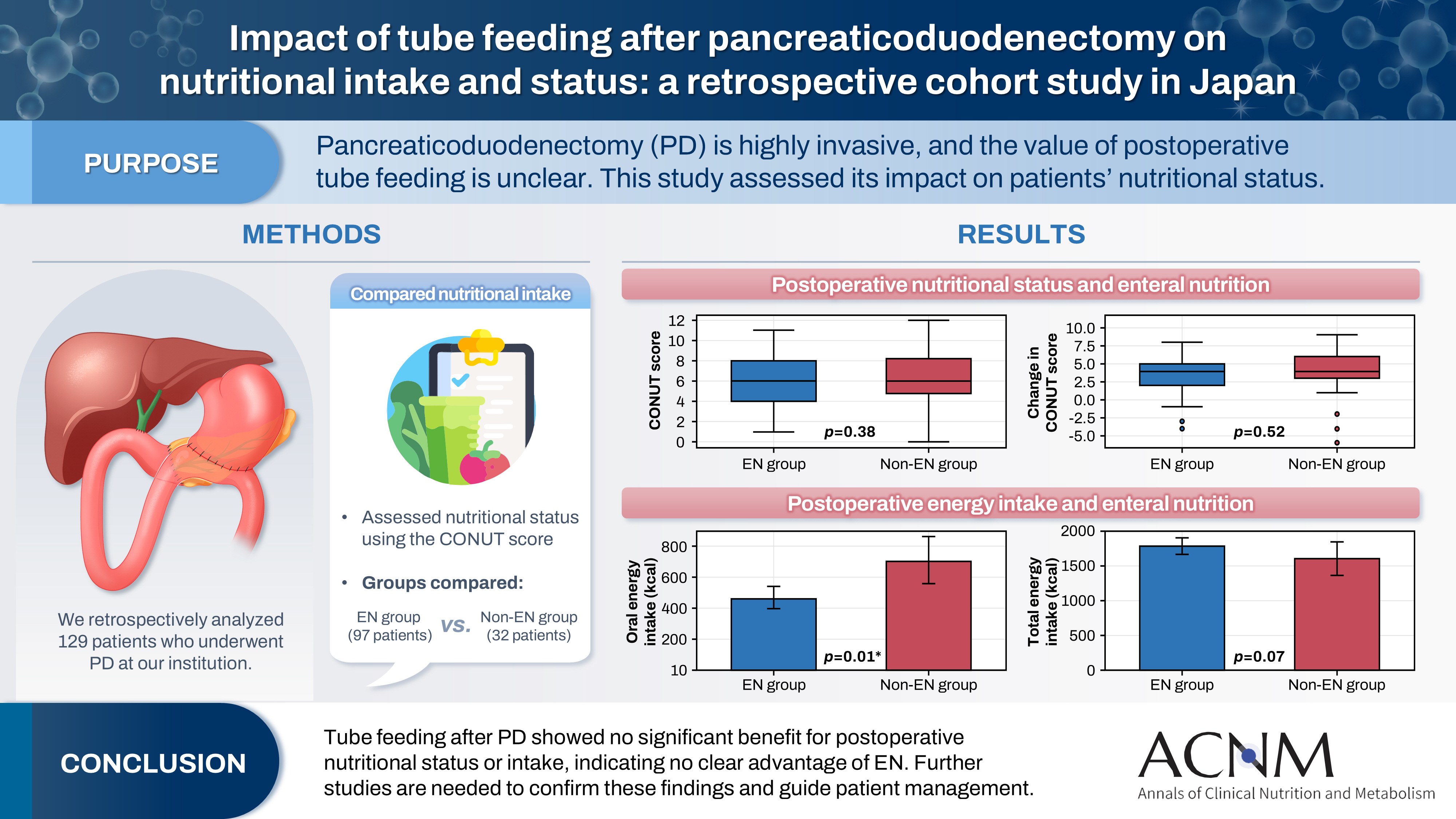
-
 Graphical Abstract
Graphical Abstract
 Abstract
Abstract
 PDF
PDF 
- Purpose
Pancreaticoduodenectomy (PD) is one of the most invasive procedures in gastrointestinal surgery. However, the clinical significance of postoperative tube feeding remains unclear. This study investigated the impact of enteral nutrition (EN) on the postoperative nutritional status of patients undergoing PD.
Methods
We retrospectively analyzed 129 patients who underwent PD at Tohoku University Hospital. Nutritional intake and status, evaluated using the Controlling Nutritional Status score, were compared between two groups: an EN group (97 patients) and a non-EN group (32 patients).
Results
There were no significant differences between the two groups in age, sex, body mass index, underlying diseases, operative duration, blood loss, postoperative pancreatic fistula, postoperative complications, delayed gastric emptying, or length of hospital stay. Although the EN group showed improvements in nutritional status both at discharge and compared with preoperative values, none of these changes reached statistical significance. Oral caloric intake was significantly higher in the non-EN group (P=0.01). In contrast, total energy intake was higher in the EN group, but this difference did not reach statistical significance (P=0.07).
Conclusion
Tube feeding after PD did not significantly influence postoperative nutritional status or overall nutritional intake. These findings suggest that EN offers no clear advantage over other approaches; however, further research is warranted to validate these results, refine existing guidelines, and optimize postoperative patient management.
- 1,280 View
- 20 Download

Editorial
- Strengthening collaboration: introducing the contributions of Japanese Society for Surgical Metabolism and Nutrition to Annals of Clinical Nutrition and Metabolism
-
Ye Rim Chang

- Ann Clin Nutr Metab 2025;17(2):95-96. Published online August 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0022
- 1,466 View
- 19 Download

Original Articles
- Peripheral vein infusions of amino acids prevent early postoperative weight loss after robot-assisted radical transmediastinal esophagectomy: a retrospective study in Japan
-
Tomonori Narita
 , Kazuhiko Fukatsu
, Kazuhiko Fukatsu , Satoshi Murakoshi
, Satoshi Murakoshi , Reo Inoue
, Reo Inoue , Kenichi Kono
, Kenichi Kono , Midori Noguchi
, Midori Noguchi , Nana Matsumoto
, Nana Matsumoto , Shoh Yajima
, Shoh Yajima , Koichi Yagi
, Koichi Yagi , Yoshifumi Baba
, Yoshifumi Baba
- Ann Clin Nutr Metab 2025;17(2):149-155. Published online August 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0012
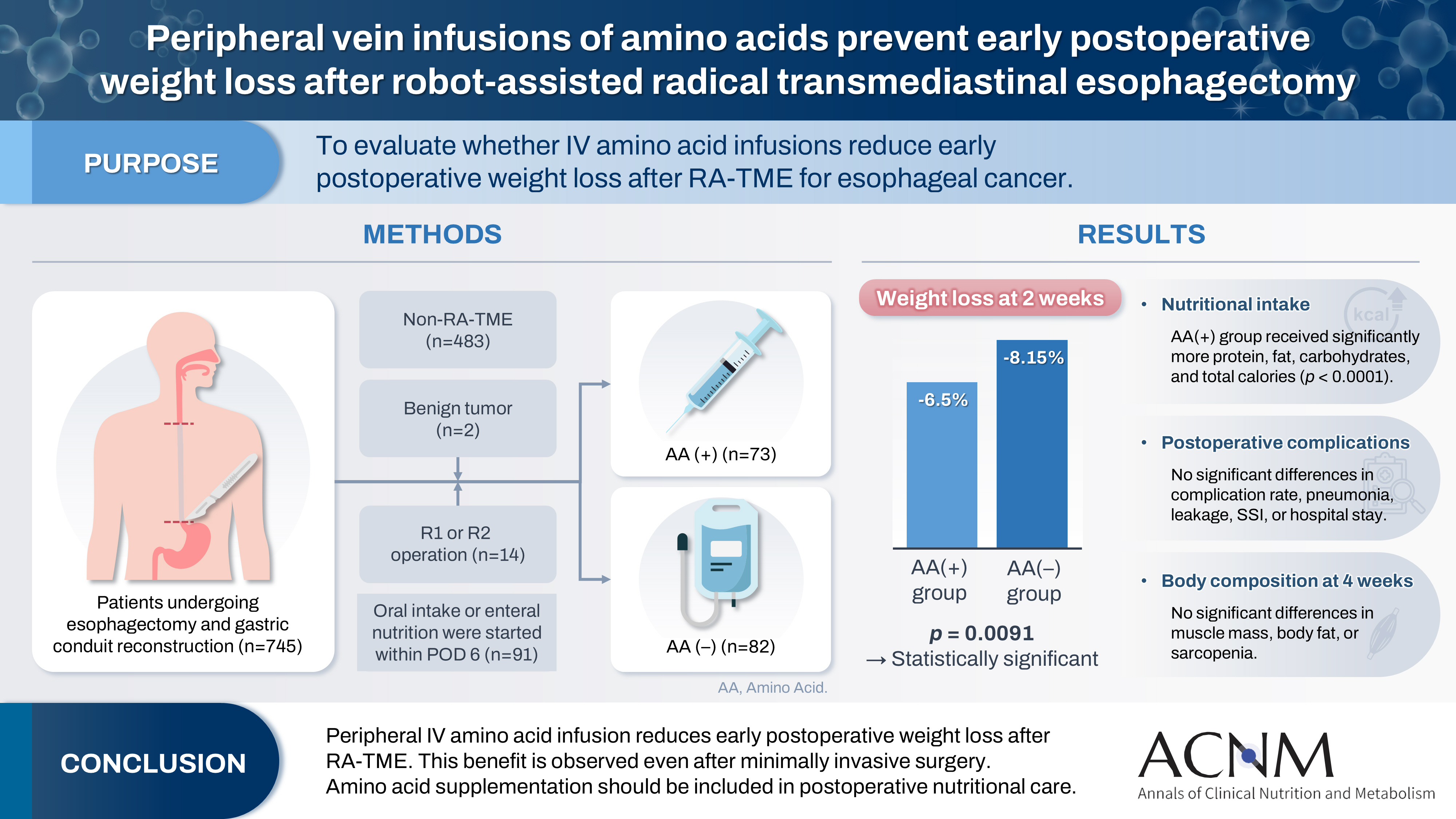
-
 Graphical Abstract
Graphical Abstract
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material 
- Purpose
Postoperative body weight loss (PBWL) is linked to poor long-term outcomes following esophagectomy for esophageal cancer, making perioperative nutrition critically important. Although minimally invasive procedures such as robot-assisted radical transmediastinal esophagectomy (RA-TME) have become more prevalent, less attention has been paid to perioperative nutritional management. This study evaluates the impact of intravenous (IV) amino acid infusions on PBWL in patients undergoing RA-TME.
Methods
We retrospectively analyzed 155 patients who underwent RA-TME for esophageal or esophagogastric junction cancer at our hospital between 2011 and 2022. Patients were divided into two groups: AA(+) (n=73, received IV amino acids between postoperative days 1–6) and AA(–) (n=82, did not receive IV amino acids). Oral or enteral nutrition was withheld until postoperative day 6. We compared nutrient intake, postoperative outcomes, and nutritional status between groups.
Results
Patient backgrounds, surgical outcomes, and complication rates were similar in both groups. However, the AA(+) group received significantly greater energy and nutrient intake. PBWL at 2 weeks post-surgery was significantly lower in the AA(+) group than in the AA(–) group (6.50% vs. 8.15%, P=0.0091).
Conclusion
IV amino acid infusion may help mitigate early PBWL after RA-TME.
- 1,860 View
- 25 Download

- Evaluation of the modified Nutrition Risk in Critically Ill score in Korean critically ill patients with COVID-19: a retrospective cohort study
-
Won Ho Han
 , Jong-Mog Lee
, Jong-Mog Lee , Jae Hoon Lee
, Jae Hoon Lee , Hyun Mi Lee
, Hyun Mi Lee , Ji-Yeon Kim
, Ji-Yeon Kim , Mok Young Jang
, Mok Young Jang , Sung-Sik Han
, Sung-Sik Han
- Ann Clin Nutr Metab 2025;17(2):125-131. Published online August 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0009
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Purpose
We evaluated the efficacy of the modified Nutrition Risk in Critically Ill (mNUTRIC) score for malnutrition screening and its association with mortality in intensive care unit (ICU) patients with COVID-19.
Methods
The nutritional status of 129 COVID-19 ICU patients admitted between February 2021 and May 2022 was assessed using American Society for Parenteral and Enteral Nutrition/Academy of Nutrition and Dietetics (ASPEN/AND) criteria. The sensitivity, specificity, and clinical correlations of the mNUTRIC score were analyzed.
Results
Of the 129 patients, 35 (27.1%) met the ASPEN/AND malnutrition criteria. Multivariable analysis identified the mNUTRIC score, underlying malignancy, and mechanical ventilation as significant factors associated with malnutrition. The mNUTRIC score had a sensitivity of 77.1% and specificity of 63.8% (area under the curve [AUC], 0.71; 95% confidence interval [CI], 0.62–0.79) for diagnosing malnutrition, improving to 88.6% and 80.9%, respectively, after adjusting for malignancy and ventilation (AUC, 0.89; 95% CI, 0.82–0.95). Patients with a low mNUTRIC score had a mortality rate of 2.9% and a median ICU stay of 7.7 days (range, 0–84.2 days), whereas those with a high score (≥5) had a mortality rate of 13.1% and a median ICU stay of 10.2 days (range, 1.4–88.5 days) (P=0.046 and P=0.011, respectively).
Conclusion
The mNUTRIC score is an effective screening tool for malnutrition in ICU patients with COVID-19, especially those with malignancy or requiring mechanical ventilation, and is strongly associated with mortality and length of ICU stay.
- 3,855 View
- 37 Download

- Perioperative outcomes of older adult patients with pancreatic cancer based on nutritional status: a retrospective cohort study
-
Takanori Morikawa
 , Masaharu Ishida
, Masaharu Ishida , Masamichi Mizuma
, Masamichi Mizuma , Kei Nakagawa
, Kei Nakagawa , Takashi Kamei
, Takashi Kamei , Michiaki Unno
, Michiaki Unno
- Ann Clin Nutr Metab 2025;17(1):66-74. Published online April 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.001
-
 Abstract
Abstract
 PDF
PDF - Purpose
This study investigated the effects of preoperative nutritional status on postoperative outcomes in older adult patients with pancreatic adenocarcinoma.
Methods
The background and perioperative factors of patients who underwent pancreatectomy for pancreatic adenocarcinoma between 2007 and 2020 were retrospectively analyzed.
Results
Patients aged 75 years or over (older adults) were significantly associated with hypertension, upfront surgery, and lower prognostic nutritional index. In addition, these patients had a significantly lower rate of portal vein resection, less blood loss, and shorter operation time than patients aged less than 75 years (non-older adults). During the postoperative course, older adult patients had a higher rate of pneumonia and lower overall survival than younger patients, although recurrence‐free survival was comparable. In addition, older adult patients showed preoperative malnutrition as a risk factor for postoperative in‐hospital death.
Conclusion
Surgical treatment for pancreatic cancer in older adult patients was performed safely. However, preoperative malnutrition is a risk factor for in‐hospital death and such patients require nutritional support and less‐invasive surgery. -
Citations
Citations to this article as recorded by- Strengthening collaboration: introducing the contributions of Japanese Society for Surgical Metabolism and Nutrition to Annals of Clinical Nutrition and Metabolism
Ye Rim Chang
Ann Clin Nutr Metab.2025; 17(2): 95. CrossRef
- Strengthening collaboration: introducing the contributions of Japanese Society for Surgical Metabolism and Nutrition to Annals of Clinical Nutrition and Metabolism
- 2,910 View
- 29 Download
- 1 Crossref

- Association between decreased dietary intake during hospitalization and long-term weight loss in postoperative gastric cancer patients over 75 years of age: a retrospective cohort study
-
Daiki Tabe
 , Isao Miyajima
, Isao Miyajima , Akira Tsukada
, Akira Tsukada
- Ann Clin Nutr Metab 2025;17(1):75-84. Published online April 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0004
-
 Abstract
Abstract
 PDF
PDF - Purpose
Weight loss following gastrectomy is a significant concern, and maintaining adequate nutrition is necessary, especially given the growing number of older adult patients. This study examined the relationship between postoperative food intake and long-term weight loss in postgastrectomy patients aged ≥75 years.
Methods
Out of 88 patients who underwent gastrectomy for gastric cancer at our institute, 46 were aged ≥75 years. These patients were divided into two groups: one with an average energy intake exceeding 50% of the basal metabolic rate and one with an intake below 50% of the basal metabolic rate. The percentage change in body weight up to 6 months post-surgery was compared between the groups.
Results
In the group with higher dietary intake, the rate of weight change at 3 and 6 months postoperatively was lower, and fewer patients received postoperative adjuvant chemotherapy.
Conclusion
Poor postoperative food intake may serve as a predictor of weight loss up to 3 months following surgery in postgastrectomy patients aged ≥75 years. -
Citations
Citations to this article as recorded by- Strengthening collaboration: introducing the contributions of Japanese Society for Surgical Metabolism and Nutrition to Annals of Clinical Nutrition and Metabolism
Ye Rim Chang
Ann Clin Nutr Metab.2025; 17(2): 95. CrossRef
- Strengthening collaboration: introducing the contributions of Japanese Society for Surgical Metabolism and Nutrition to Annals of Clinical Nutrition and Metabolism
- 1,818 View
- 33 Download
- 1 Crossref

Review
- Changes in perceptions of taste after bariatric surgery: a narrative review
-
Young Suk Park

- Ann Clin Nutr Metab 2024;16(3):120-124. Published online December 1, 2024
- DOI: https://doi.org/10.15747/ACNM.2024.16.3.120
-
 Abstract
Abstract
 PDF
PDF - Purpose: Bariatric surgery effectively treats severe obesity, leading to significant weight loss and improved comorbidities. However, many patients experience postoperative alterations in taste perception, affecting food selection and eating behavior. This narrative review examines the current understanding of taste perception changes following bariatric surgery, including patterns, potential mechanisms, impact on weight loss outcomes, and implications for patient care.
Current concept: Changes in taste perception are frequently reported after bariatric procedures, with prevalence rates from 36% to 72%. Common alterations involve decreased preference and increased sensitivity to sweet and fatty tastes, potentially leading to reduced calorie intake and healthier food choices. Persistence of these changes varies and may depend on surgery type, with Roux-en-Y gastric bypass patients often experiencing more substantial effects than sleeve gastrectomy patients. Potential mechanisms include alterations in gut hormone secretion (e.g., GLP-1, peptide YY, ghrelin), modifications in neural pathways (e.g., vagus nerve), and shifts in the gut microbiome. These factors may collectively influence taste sensitivity and preferences, contributing to weight loss outcomes. Altered reward processing may reduce the appeal of high-calorie foods.
Conclusion: Alterations in taste perception are common after bariatric surgery and may significantly impact dietary behaviors, weight loss, and quality of life. While exact mechanisms are not fully understood, changes in gut hormones, neural pathways, and microbiota are likely involved. Patient counseling and postoperative management of bariatric surgery patients should address potential changes in taste. Further research is needed to elucidate the long-term impacts of taste alterations on weight-loss maintenance and nutritional status.
- 7,654 View
- 69 Download

Interesting image
- Pneumothorax due to malpositioned nasogastric enteral feeding tube
-
Hyebeen Kim
 , Suk-Kyung Hong
, Suk-Kyung Hong
- Ann Clin Nutr Metab 2024;16(2):87-88. Published online August 1, 2024
- DOI: https://doi.org/10.15747/ACNM.2024.16.2.87
-
 PDF
PDF -
Citations
Citations to this article as recorded by- Bilateral Pneumothoraces During Nasogastric Tube Placement: A Case Report
Gideon Asaolu, Martin Aaron Tan, Jay Narula, Rajat Gupta, Sana Ahmed, Hardeep Singh, Dhaval Patel, Amr A. Arafat
Case Reports in Medicine.2026;[Epub] CrossRef
- Bilateral Pneumothoraces During Nasogastric Tube Placement: A Case Report
- 2,926 View
- 34 Download
- 1 Crossref

Original Article
- Prognostic significance of serum creatinine and sarcopenia for 5-year overall survival in patients with colorectal cancer in Korea: a comparative study
-
Jiahn Choi
 , Hye Sun Lee
, Hye Sun Lee , Jeonghyun Kang
, Jeonghyun Kang
- Ann Clin Nutr Metab 2024;16(2):66-77. Published online August 1, 2024
- DOI: https://doi.org/10.15747/ACNM.2024.16.2.66
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Purpose: Previous studies have demonstrated that the serum creatinine level and skeletal muscle index (SMI) (correlated with the overall survival [OS] of patients with colorectal cancer [CRC]). However, the combined significance of these 2 factors is not fully understood. The goal of this study was to investigate the prognostic potential of the combination of these two factors in patients with CRC.
Methods: The patients were categorized into subgroups based on preoperative serum creatinine level, with a cut-off value of 1.01 mg/dL for males and 0.80 mg/dL for females. The patients were further categorized into 4 groups based on SMI. Data were analyzed using the Cox proportional hazards model and Harrell’s concordance index (C-index).
Results: Poor 5-year OS was observed in patients with high SMI and high serum creatinine levels (hazard ratio [HR]=1.676, 95% confidence interval [CI]=1.110–2.529, P=0.013), low SMI and low serum creatinine levels (HR=1.916, 95% CI=1.249–2.938, P=0.002), and low SMI and high serum creatinine levels (HR=2.172, 95% CI=1.279–3.687, P=0.004) compared to those of patients with high SMI and low serum creatinine levels. Grouping patients based on both SMI and serum creatinine levels led to improved prognostic stratification (C-index, 0.626; 95% CI=0.587–0.666) compared to grouping based on SMI (CI difference=0.062, 95% CI=0.031–0.103, P=0.0011) or serum creatinine (CI difference=0.043, 95% CI=0.017–0.081, P=0.0072) alone.
Conclusion: Incorporating both SMI and serum creatinine levels enhances the prognostic stratification for 5-year OS in patients with CRC, surpassing the prognostic power of grouping solely based on SMI or creatinine.
- 4,087 View
- 22 Download

Correction
- Correction: article type revision
- Editorial Office, Annals of Clinical Nutrition and Metabolism
- Ann Clin Nutr Metab 2025;17(3):212-212. Published online December 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0033
- Corrects: Ann Clin Nutr Metab 2025;17(1):3
- 651 View
- 13 Download

Original Articles
- Effects of enteral nutrition formulas with varying carbohydrate amounts on glycemic control in diabetic mice
-
Yukari Miki
 , Kazuo Hino
, Kazuo Hino
- Ann Clin Nutr Metab 2025;17(1):85-93. Published online April 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0006
-
 Abstract
Abstract
 PDF
PDF - Purpose
This study evaluated the effects of an 8‑week liquid diets with different carbohydrate contents–64% energy in HINE E‑Gel (ST) and 50% energy in HINE E‑Gel LC (LC)–on glycemic control and nutritional status in a mouse model of type 2 diabetes mellitus (db/db mice). The objective was to determine whether reducing carbohydrate intake within the Dietary Reference Intakes for Japanese people improves glycemic control indices, addressing the evidence gap in regarding the long‑term safety and efficacy of low‑carbohydrate enteral nutrition in patients with diabetes.
Methods
db/db mice (n=10 per group) and non‑diabetic db/m mice (n=4) as controls were fed ST, LC, or AIN‑93G diets ad libitum for 8 weeks. The diets primarily differed in carbohydrate content (64% in ST vs. 50% in LC). Blood glucose and glycated hemoglobin (HbA1c), plasma glucose and glycoalbumin, organ weights, and renal function markers were measured weekly or at 4 and 8 weeks. Histopathological examinations of the liver and kidneys were performed at 8 weeks.
Results
At 8 weeks, the LC group showed significantly lower plasma glucose (P=0.0051) and glycoalbumin (P=0.0013) levels compared to the ST group, with a trend toward lower HbA1c (P=0.0514). Although body weight was significantly higher in the LC group (P=0.0038), there were no significant differences between the ST and LC groups in caloric intake, renal function, or histopathological findings.
Conclusion
Reducing carbohydrate intake to 50% of total energy within dietary guidelines may improve glycemic control in diabetic mice, suggesting the need for further long‑term evaluation for clinical applications. -
Citations
Citations to this article as recorded by- Strengthening collaboration: introducing the contributions of Japanese Society for Surgical Metabolism and Nutrition to Annals of Clinical Nutrition and Metabolism
Ye Rim Chang
Ann Clin Nutr Metab.2025; 17(2): 95. CrossRef
- Strengthening collaboration: introducing the contributions of Japanese Society for Surgical Metabolism and Nutrition to Annals of Clinical Nutrition and Metabolism
- 2,483 View
- 34 Download
- 1 Crossref

- The impact of nutritional intervention by a nutrition support team on extrauterine growth restriction in very low birth weight infants in Korea: a retrospective cohort study
-
Seung Yun Lee
 , Hye Su Hwang
, Hye Su Hwang , Waonsun Im
, Waonsun Im , Hyojoung Kim
, Hyojoung Kim , Mi Lim Chung
, Mi Lim Chung
- Ann Clin Nutr Metab 2024;16(3):149-157. Published online December 1, 2024
- DOI: https://doi.org/10.15747/ACNM.2024.16.3.149
-
 Abstract
Abstract
 PDF
PDF - Purpose: Achieving proper weight gain through adequate nutrition is critically important in very low birth weight (VLBW) infants. Despite recent active nutritional interventions, growth restriction is still common in VLBW infants. We aimed to determine whether nutritional intervention by a nutrition support team (NST) mitigated extrauterine growth restriction (EUGR) in VLBW infants.
Methods: We retrospectively reviewed the medical records of VLBW infants admitted to Haeundae Paik Hospital between March 2010 and February 2024. EUGR was defined as a decrease in the weight-for-age-z-score>1.2 from birth to the postconceptional age of 36 weeks, using Fenton growth charts.
Results: Among the 603 enrolled VLBW infants, 434 (72.0%) were diagnosed with EUGR. When comparing the control and nutritional intervention groups, the incidence of EUGR was significantly lower in infants in the intervention group (80.6% vs. 62.8%, P<0.00). Intervention group infants started enteral feeding earlier and reached half and full enteral feeding earlier (P<0.05). In addition, intravenous protein and lipid supply started sooner, increased at a faster rate, and reached peak concentrations sooner in the intervention group (P<0.05).
Conclusion: Nutritional intervention by an NST resulted in a significant decrease in the development of EUGR in VLBW infants.
- 3,573 View
- 61 Download


 E-submission
E-submission KSPEN
KSPEN KSSMN
KSSMN ASSMN
ASSMN JSSMN
JSSMN
 First
First Prev
Prev


