Scopus, KCI, KoreaMed

Articles
- Page Path
- HOME > Ann Clin Nutr Metab > Volume 16(3); 2024 > Article
- Review Changes in perceptions of taste after bariatric surgery: a narrative review
-
Young Suk Park1,2

-
Annals of Clinical Nutrition and Metabolism 2024;16(3):120-124.
DOI: https://doi.org/10.15747/ACNM.2024.16.3.120
Published online: December 1, 2024
1Department of Surgery, Seoul National University Bundang Hospital, Seongnam, Korea
2Department of Surgery, Seoul National University College of Medicine, Seoul, Korea
- Corresponding author: Young Suk Park, email: youngsukmd@gmail.com
© 2024 The Korean Society of Surgical Metabolism and Nutrition · The Korean Society for Parenteral and Enteral Nutrition
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
- 7,473 Views
- 68 Download
- Abstract
- Introduction
- Bariatric procedures
- Patterns and persistence of changes in taste perception after bariatric surgery
- Potential mechanisms of changes in the perception of taste
- Do changes in the perception of taste contribute to weight loss after bariatric surgery?
- Importance of addressing changes in the perception of taste in preoperative patient counseling
- Conclusion
- Acknowledgments
- Notes
- References
Abstract
-
Purpose Bariatric surgery effectively treats severe obesity, leading to significant weight loss and improved comorbidities. However, many patients experience postoperative alterations in taste perception, affecting food selection and eating behavior. This narrative review examines the current understanding of taste perception changes following bariatric surgery, including patterns, potential mechanisms, impact on weight loss outcomes, and implications for patient care.
-
Current concept Changes in taste perception are frequently reported after bariatric procedures, with prevalence rates from 36% to 72%. Common alterations involve decreased preference and increased sensitivity to sweet and fatty tastes, potentially leading to reduced calorie intake and healthier food choices. Persistence of these changes varies and may depend on surgery type, with Roux-en-Y gastric bypass patients often experiencing more substantial effects than sleeve gastrectomy patients. Potential mechanisms include alterations in gut hormone secretion (e.g., GLP-1, peptide YY, ghrelin), modifications in neural pathways (e.g., vagus nerve), and shifts in the gut microbiome. These factors may collectively influence taste sensitivity and preferences, contributing to weight loss outcomes. Altered reward processing may reduce the appeal of high-calorie foods.
-
Conclusion Alterations in taste perception are common after bariatric surgery and may significantly impact dietary behaviors, weight loss, and quality of life. While exact mechanisms are not fully understood, changes in gut hormones, neural pathways, and microbiota are likely involved. Patient counseling and postoperative management of bariatric surgery patients should address potential changes in taste. Further research is needed to elucidate the long-term impacts of taste alterations on weight-loss maintenance and nutritional status.
Introduction
Bariatric procedures
Patterns and persistence of changes in taste perception after bariatric surgery
Potential mechanisms of changes in the perception of taste
Do changes in the perception of taste contribute to weight loss after bariatric surgery?
Importance of addressing changes in the perception of taste in preoperative patient counseling
Conclusion
Acknowledgments
Conflict of interest
The author of this manuscript has no conflicts of interest to disclose.
Funding
This work was supported by grant from Seoul National University Bundang Hospital research fund (No. 02-2016-0036).
Data availability
None.
Supplementary materials
None.
| Potential mechanisms | Summary | References |
|---|---|---|
| Alterations in gut hormones | Bariatric procedures alter gut hormone secretion, including GLP-1, PYY, and ghrelin, impacting appetite and taste perception | [12,13] |
| Neural pathway modifications | Vagus nerve and other neural pathways involved in taste perception may be affected, leading to changes in taste sensitivity and preferences | [14-16] |
| Changes in gut microbiome | Shifts in oral and gut microbiota composition after surgery can impact taste perception and influence dietary habits | [17,19,20] |
- 1. Bueter M, Miras AD, Chichger H, Fenske W, Ghatei MA, Bloom SR, et al. Alterations of sucrose preference after Roux-en-Y gastric bypass. Physiol Behav 2011;104:709-21. ArticlePubMed
- 2. Behary P, Miras AD. Food preferences and underlying mechanisms after bariatric surgery. Proc Nutr Soc 2015;74:419-25. ArticlePubMed
- 3. Miras AD, le Roux CW. Mechanisms underlying weight loss after bariatric surgery. Nat Rev Gastroenterol Hepatol 2013;10:575-84. ArticlePubMedPDF
- 4. Mozaffar B, Mozaffar H, Alkharaiji M, Elbahrawy A, Idris I. Associations between zinc deficiency, taste changes, and salivary flow rates following gastric bypass and sleeve gastrectomy surgeries. J Nutr Metab 2024;2024:1197571. ArticlePubMedPMCPDF
- 5. Walmsley R, Chong L, Hii MW, Brown RM, Sumithran P. 2024;The effect of bariatric surgery on the expression of gastrointestinal taste receptors: a systematic review. Rev Endocr Metab Disord 25:421-46. ArticlePubMedPMCPDF
- 6. Van Vuuren MAJ, Strodl E, White KM, Lockie PD. Taste, enjoyment, and desire of flavors change after sleeve gastrectomy-short term results. Obes Surg 2017;27:1466-73. ArticlePubMedPDF
- 7. Miras AD, Jackson RN, Jackson SN, Goldstone AP, Olbers T, Hackenberg T, et al. Gastric bypass surgery for obesity decreases the reward value of a sweet-fat stimulus as assessed in a progressive ratio task. Am J Clin Nutr 2012;96:467-73. ArticlePubMed
- 8. Mathes CM, Spector AC. Food selection and taste changes in humans after Roux-en-Y gastric bypass surgery: a direct-measures approach. Physiol Behav 2012;107:476-83. ArticlePubMed
- 9. Smith KR, Aghababian A, Papantoni A, Veldhuizen MG, Kamath V, Harris C, et al. One year follow-up of taste-related reward associations with weight loss suggests a critical time to mitigate weight regain following bariatric surgery. Nutrients 2021;13:3943.ArticlePubMedPMC
- 10. Schiavo L, Aliberti SM, Calabrese P, Senatore AM, Severino L, Sarno G, et al. Changes in food choice, taste, desire, and enjoyment 1 year after sleeve gastrectomy: a prospective study. Nutrients 2022;14:2060.ArticlePubMedPMC
- 11. Nance K, Acevedo MB, Pepino MY. Changes in taste function and ingestive behavior following bariatric surgery. Appetite 2020;146:104423. ArticlePubMedPMC
- 12. Beckman LM, Beckman TR, Earthman CP. 2010;Changes in gastrointestinal hormones and leptin after Roux-en-Y gastric bypass procedure: a review. J Am Diet Assoc 110:571-84. ArticlePubMedPMC
- 13. Martin B, Dotson CD, Shin YK, Ji S, Drucker DJ, Maudsley S, et al. Modulation of taste sensitivity by GLP-1 signaling in taste buds. Ann N Y Acad Sci 2009;1170:98-101. ArticlePubMedPMC
- 14. Berthoud HR. Vagal and hormonal gut-brain communication: from satiation to satisfaction. Neurogastroenterol Motil 2008;20 Suppl 1:64-72. ArticlePubMedPMC
- 15. Sperling W, Biermann T, Spannenberger R, Clepce M, Padberg F, Reulbach U, et al. Changes in gustatory perceptions of patients with major depression treated with vagus nerve stimulation (VNS). Pharmacopsychiatry 2011;44:67-71. ArticlePubMed
- 16. Felizardo R, Boucher Y, Braud A, Carstens E, Dauvergne C, Zerari-Mailly F. Trigeminal projections on gustatory neurons of the nucleus of the solitary tract: a double-label strategy using electrical stimulation of the chorda tympani and tracer injection in the lingual nerve. Brain Res 2009;1288:60-8. ArticlePubMed
- 17. Schamarek I, Anders L, Chakaroun RM, Kovacs P, Rohde-Zimmermann K. The role of the oral microbiome in obesity and metabolic disease: potential systemic implications and effects on taste perception. Nutr J 2023;22:28.ArticlePubMedPMCPDF
- 18. Adawi H, Aggarwal A, Jain S, Othman MA, Othman AAA, Zakri RA, et al. Influence of bariatric surgery on oral microbiota: a systematic review. Eur J Dent 2023;17:602-14. ArticlePubMedPMC
- 19. Gardner A, So PW, Carpenter GH. Intraoral microbial metabolism and association with host taste perception. J Dent Res 2020;99:739-45. ArticlePubMedPMCPDF
- 20. Cattaneo C, Riso P, Laureati M, Gargari G, Pagliarini E. Exploring associations between interindividual differences in taste perception, oral microbiota composition, and reported food intake. Nutrients 2019;11:1167.ArticlePubMedPMC
- 21. Berthoud HR, Zheng H. Modulation of taste responsiveness and food preference by obesity and weight loss. Physiol Behav 2012;107:527-32. ArticlePubMedPMC
- 22. Smith KR, Papantoni A, Veldhuizen MG, Kamath V, Harris C, Moran TH, et al. Taste-related reward is associated with weight loss following bariatric surgery. J Clin Invest 2020;130:4370-81. ArticlePubMedPMC
- 23. Fathi M, Javid AZ, Mansoori A. Effects of weight change on taste function; a systematic review. Nutr J 2023;22:22.ArticlePubMedPMCPDF
- 24. Gradaschi R, Molinari V, Sukkar SG, De Negri P, Adami GF, Camerini G. Effects of the postoepartive dietetic/behavioral counseling on the weight loss after bariatric surgery. Obes Surg 2020;30:244-8. ArticlePubMedPDF
- 25. Koffman L, Levis AW, Haneuse S, Johnson E, Bock S, McSperitt D, et al. Evaluation of intensive telephonic nutritional and lifestyle counseling to enhance outcomes of bariatric surgery. Obes Surg 2022;32:133-41. ArticlePubMedPDF
References
Figure & Data
REFERENCES
Citations

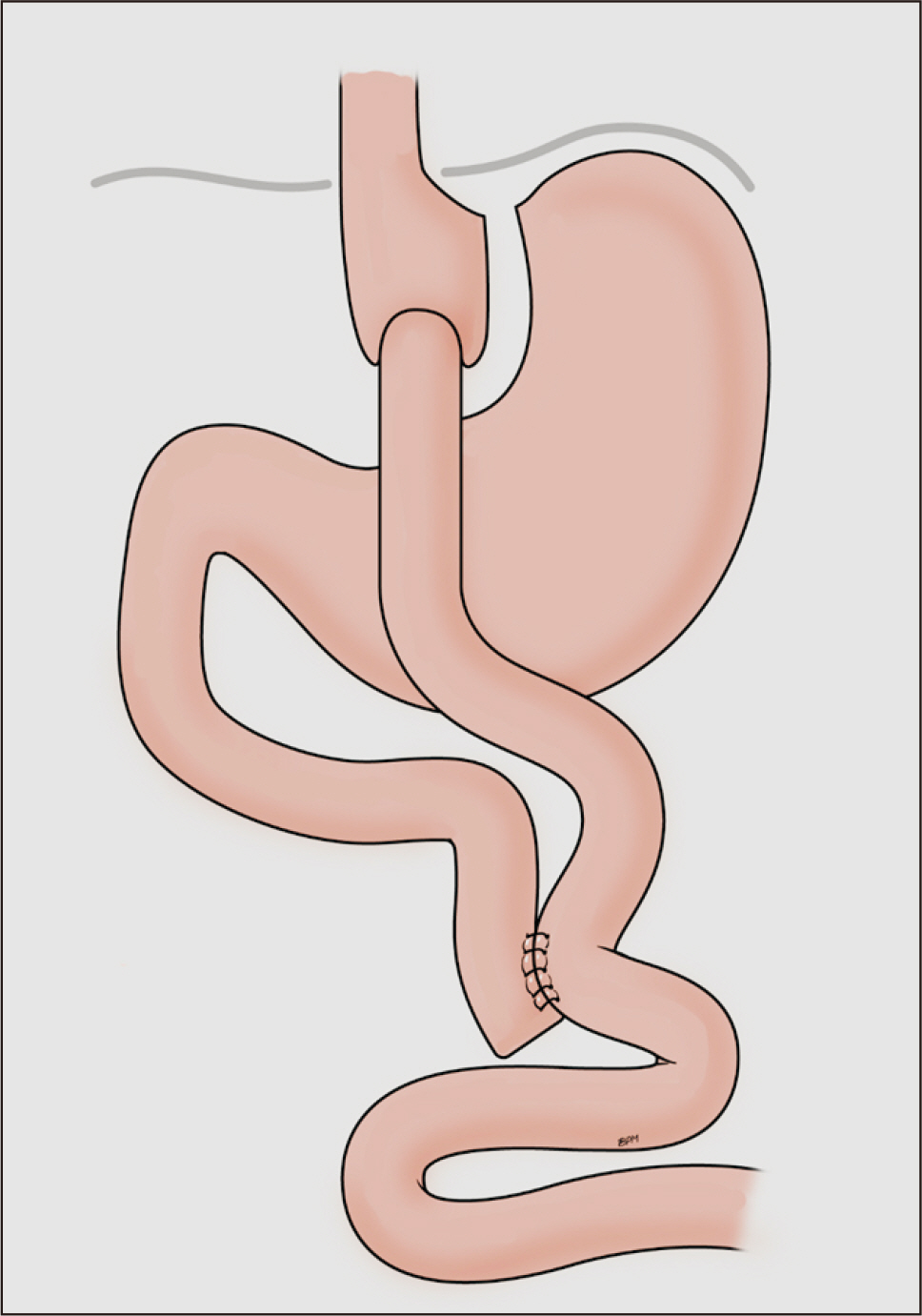
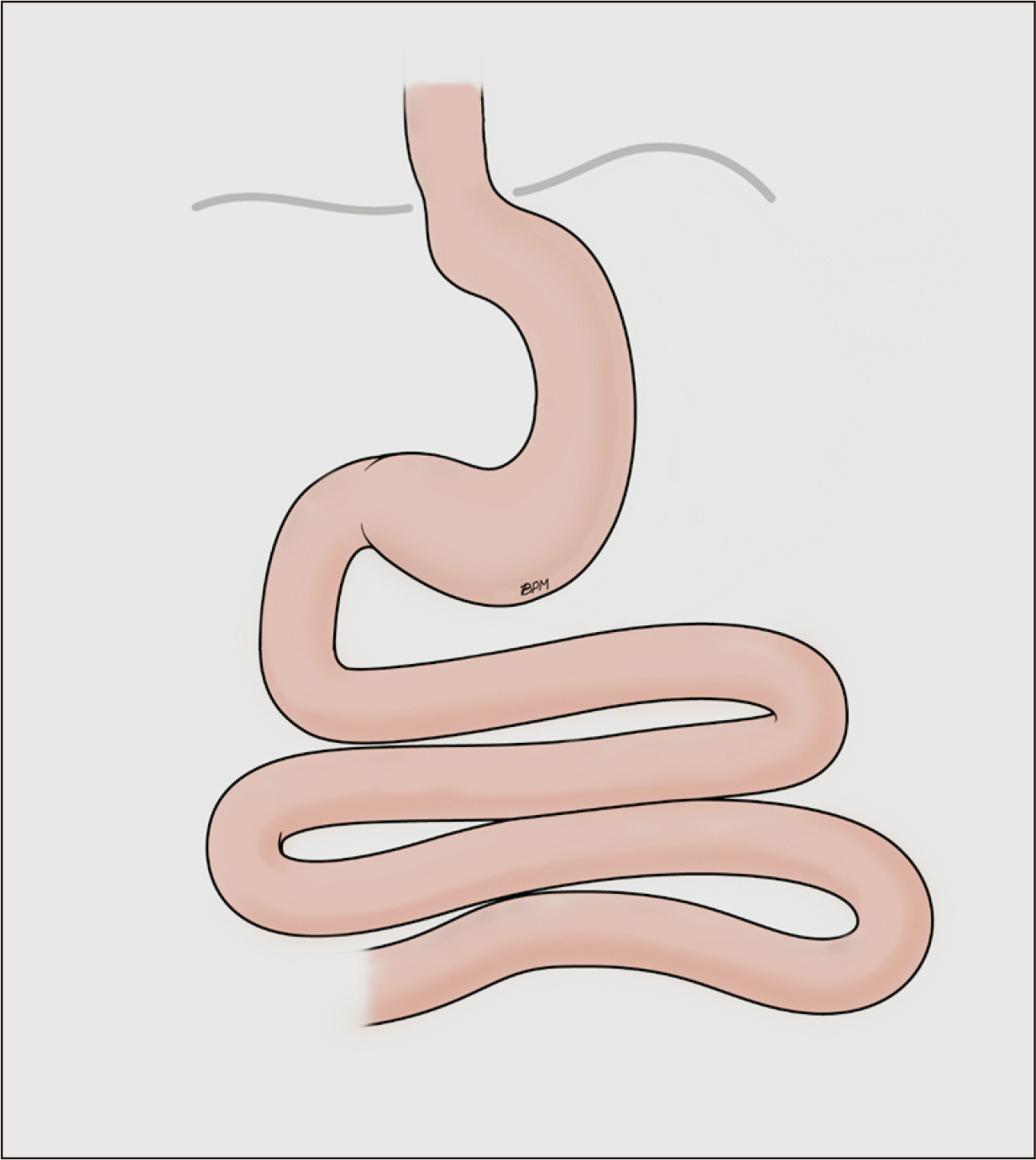
Fig. 1
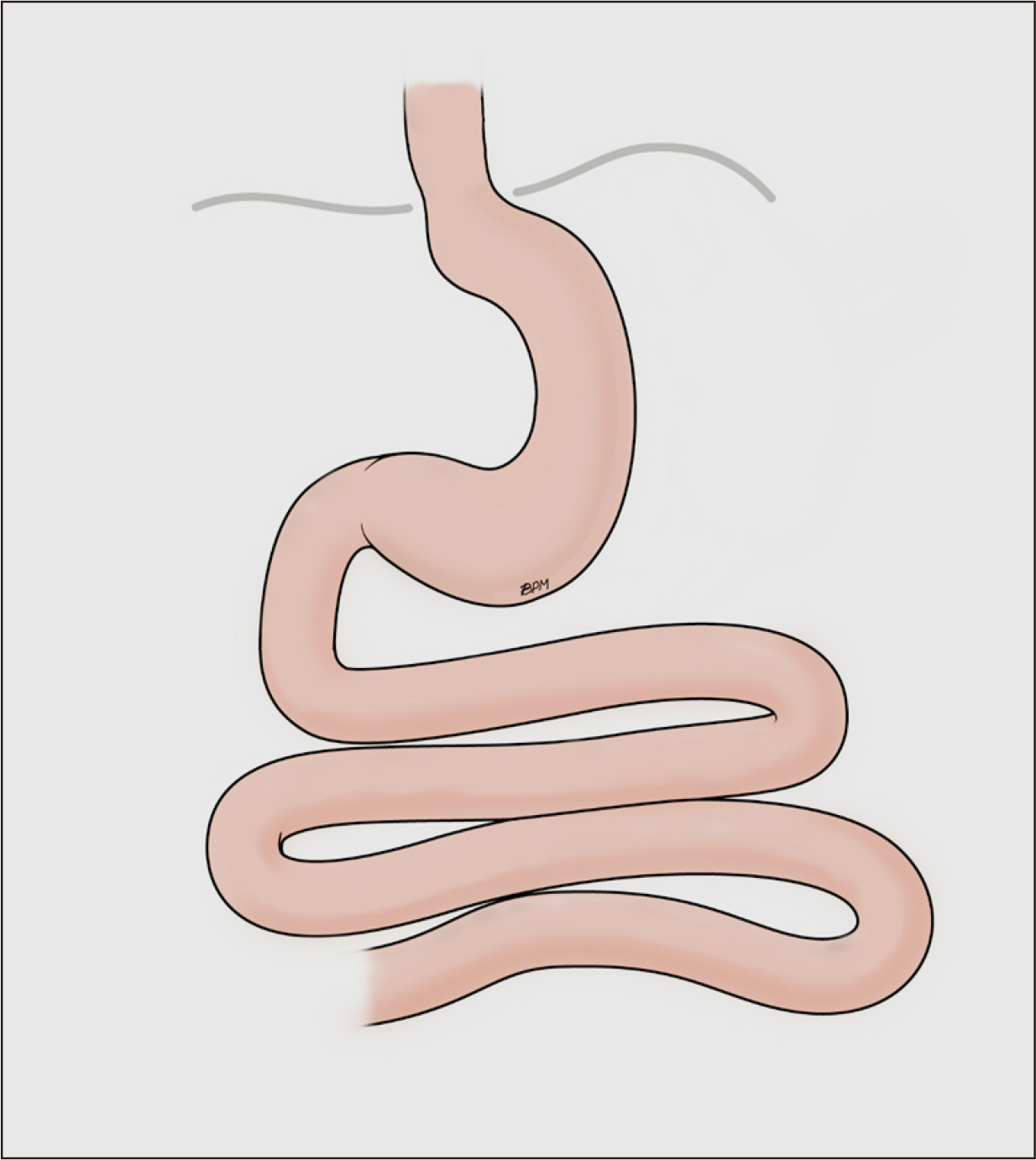
Fig. 2
Potential mechanisms underlying changes in taste perception after bariatric surgery
| Potential mechanisms | Summary | References |
|---|---|---|
| Alterations in gut hormones | Bariatric procedures alter gut hormone secretion, including GLP-1, PYY, and ghrelin, impacting appetite and taste perception | [ |
| Neural pathway modifications | Vagus nerve and other neural pathways involved in taste perception may be affected, leading to changes in taste sensitivity and preferences | [ |
| Changes in gut microbiome | Shifts in oral and gut microbiota composition after surgery can impact taste perception and influence dietary habits | [ |
GLP-1 = glucagon-like peptide-1; PYY = peptide YY.
GLP-1 = glucagon-like peptide-1; PYY = peptide YY.

 E-submission
E-submission KSPEN
KSPEN KSSMN
KSSMN ASSMN
ASSMN JSSMN
JSSMN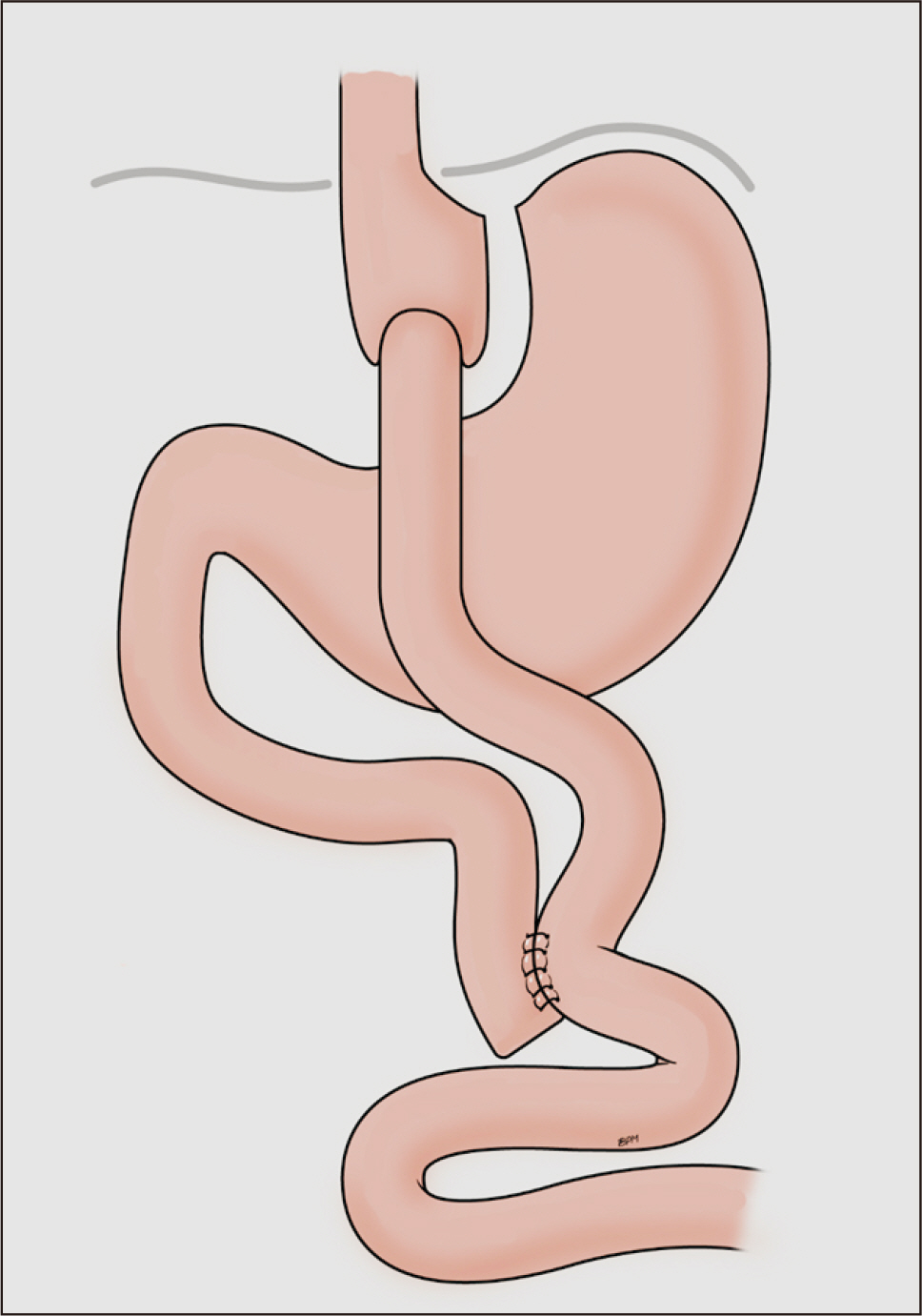
 Cite
Cite

