Scopus, KCI, KoreaMed

Search
- Page Path
- HOME > Search
- Penetration of a nasogastric tube by a stylet during insertion
-
Akihide Takami
 , Haruka Tsuji
, Haruka Tsuji , Kazuya Omura
, Kazuya Omura
- Ann Clin Nutr Metab 2025;17(3):210-211. Published online December 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0029
- 740 View
- 16 Download

- Impact of tube feeding after pancreaticoduodenectomy on nutritional intake and status: a retrospective cohort study in Japan
-
Masaharu Ishida
 , Masahiro Iseki
, Masahiro Iseki , Shuichiro Hayashi
, Shuichiro Hayashi , Aya Noguchi
, Aya Noguchi , Hideaki Sato
, Hideaki Sato , Shingo Yoshimachi
, Shingo Yoshimachi , Akiko Kusaka
, Akiko Kusaka , Mitsuhiro Shimura
, Mitsuhiro Shimura , Shuichi Aoki
, Shuichi Aoki , Daisuke Douchi
, Daisuke Douchi , Takayuki Miura
, Takayuki Miura , Shimpei Maeda
, Shimpei Maeda , Masamichi Mizuma
, Masamichi Mizuma , Kei Nakagawa
, Kei Nakagawa , Takashi Kamei
, Takashi Kamei , Michiaki Unno
, Michiaki Unno
- Ann Clin Nutr Metab 2025;17(3):203-209. Published online December 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0020
-
 Graphical Abstract
Graphical Abstract
 Abstract
Abstract
 PDF
PDF 
- Purpose
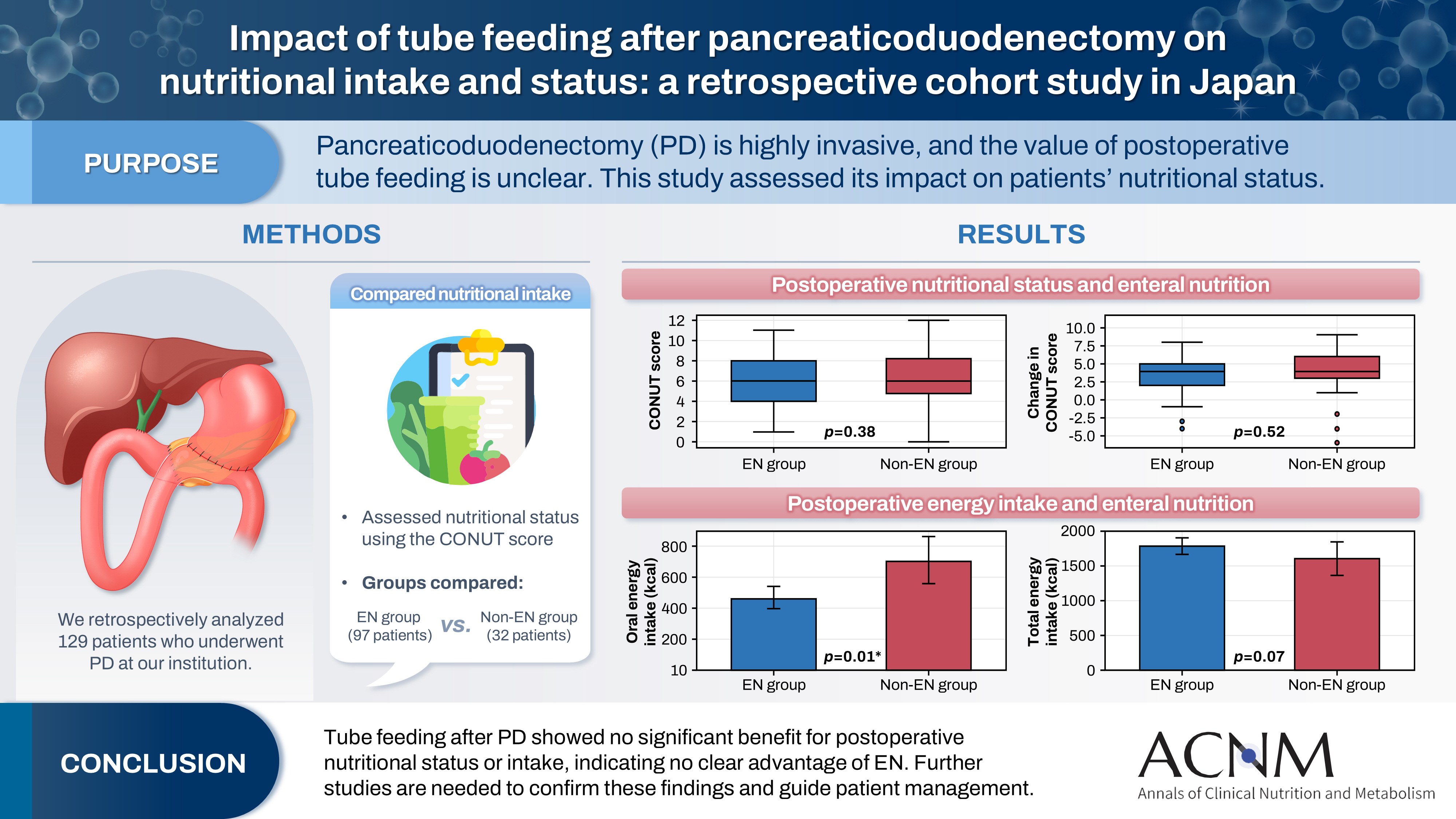
Pancreaticoduodenectomy (PD) is one of the most invasive procedures in gastrointestinal surgery. However, the clinical significance of postoperative tube feeding remains unclear. This study investigated the impact of enteral nutrition (EN) on the postoperative nutritional status of patients undergoing PD.
Methods
We retrospectively analyzed 129 patients who underwent PD at Tohoku University Hospital. Nutritional intake and status, evaluated using the Controlling Nutritional Status score, were compared between two groups: an EN group (97 patients) and a non-EN group (32 patients).
Results
There were no significant differences between the two groups in age, sex, body mass index, underlying diseases, operative duration, blood loss, postoperative pancreatic fistula, postoperative complications, delayed gastric emptying, or length of hospital stay. Although the EN group showed improvements in nutritional status both at discharge and compared with preoperative values, none of these changes reached statistical significance. Oral caloric intake was significantly higher in the non-EN group (P=0.01). In contrast, total energy intake was higher in the EN group, but this difference did not reach statistical significance (P=0.07).
Conclusion
Tube feeding after PD did not significantly influence postoperative nutritional status or overall nutritional intake. These findings suggest that EN offers no clear advantage over other approaches; however, further research is warranted to validate these results, refine existing guidelines, and optimize postoperative patient management.
- 1,228 View
- 20 Download

- Comparison of efficacy of enteral versus parenteral nutrition in patients after esophagectomy in Malaysia: a prospective cohort study
-
Ramizah Mohd Shariff
 , Sze Chee Tee
, Sze Chee Tee , Shukri Jahit Mohammad
, Shukri Jahit Mohammad , Khei Choong Khong
, Khei Choong Khong
- Ann Clin Nutr Metab 2025;17(1):41-49. Published online April 1, 2025
- DOI: https://doi.org/10.15747/ACNM.24.016
-
 Graphical Abstract
Graphical Abstract
 Abstract
Abstract
 PDF
PDF 
- Purpose
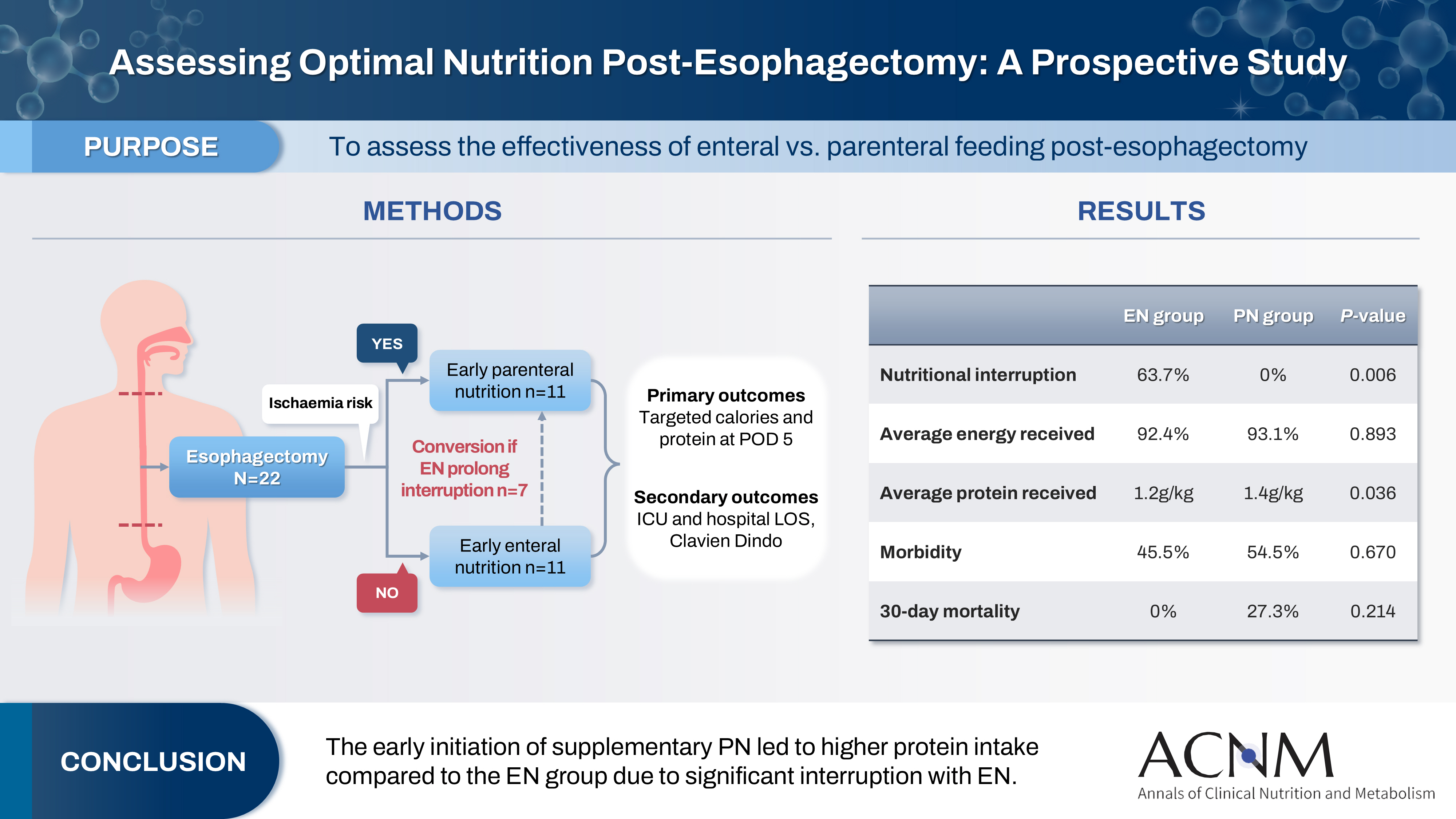
This study aims to assess the effectiveness of enteral versus parenteral feeding in patients after esophagectomy.
Methods
This a prospective cohort study of post-esophagectomy intensive care unit (ICU) patients over 12 months in the National Cancer Institute, Malaysia. Early enteral feeding followed the Enhanced Recovery After Surgery protocol, and parenteral nutrition (PN) was considered if there was a risk for conduit ischemia. It compared the effectiveness of enteral versus PN following esophagectomy, and assessed the correlations between biochemical nutritional markers and hospital lengths of stay or ventilation days.
Results
It included two cohorts receiving PN (n=11) or enteral nutrition (EN) (n=11) following elective esophagectomy. Preoperative weight, body mass index, and Subjective Global Assessment were higher in the EN group (P=0.033, P=0.021, P=0.031, respectively). Nutritional interruption occurred more frequently in the EN group (63.7%) compared to the PN group (P=0.001). Mean levels of energy and protein received were 93.1 kcal/kg and 1.4 g/kg for PN versus 92.4 kcal/kg and 1.2 g/kg for EN (P=0.893, P=0.036). The median lengths of ICU stay (P=0.688) and postoperative stay (P=0.947) between groups showed no significant difference. In addition, 30-day mortality (P=0.214) and other postoperative complications (P>0.05) were comparable in the two groups.
Conclusion
Early initiation of supplementary PN due to significant interruption in EN led to higher protein intake compared to the EN group. However, there were no significant differences in postoperative outcomes, including 30-day mortality, ICU length of stay, and ventilation days. PN ensures adequate nutritional intake, especially in terms of protein delivery, without adversely affecting postoperative recovery and clinical outcomes. -
Citations
Citations to this article as recorded by- Optimizing nutritional support in upper gastrointestinal surgery: A comprehensive review of feeding jejunostomy techniques and outcomes
Ioana Alexandra Prisacariu, Konstantinos Eleftherios Koumarelas, Konstantinos Argyriou, Alexandros Charalabopoulos, Grigorios Christodoulidis
World Journal of Gastrointestinal Surgery.2025;[Epub] CrossRef
- Optimizing nutritional support in upper gastrointestinal surgery: A comprehensive review of feeding jejunostomy techniques and outcomes
- 6,623 View
- 82 Download
- 1 Crossref

- Role of preoperative immunonutrition in patients with colorectal cancer: a narrative review
-
Soo Young Lee
 , Hyeung-min Park
, Hyeung-min Park , Chang Hyun Kim
, Chang Hyun Kim , Hyeong Rok Kim
, Hyeong Rok Kim
- Ann Clin Nutr Metab 2023;15(2):46-50. Published online August 1, 2023
- DOI: https://doi.org/10.15747/ACNM.2023.15.2.46
-
 Abstract
Abstract
 PDF
PDF - Purpose: Colorectal cancer surgery presents challenges due to surgical stress and immunosuppression, leading to postoperative complications. Nutrition is crucial for colorectal cancer patients who are prone to malnutrition. This study aims to provide a comprehensive review of the role of preoperative immunonutrition in colorectal cancer surgery.
Current concept: Preoperative immunonutrition, consisting of immunonutrients such as arginine, ω-3 fatty acids, and nucleotides, has emerged as a potential strategy to enhance surgical outcomes by modulating immune responses and reducing complications. Current guidelines recommend preoperative oral nutritional supplements for major abdominal surgery and immunonutrition for nutritionally high-risk patients. Meta-analysis have demonstrated significant decreases in infectious complications and hospital stay durations with preoperative immunonutrition. However, limitations such as publication bias and heterogeneity in the previous studies should be considered. Further research should focus on the optimal timing, duration, and amount of immunonutrition; the patient populations that would benefit most; and the integration of immunonutrition into enhanced recovery after surgery protocols.
Conclusion: While preoperative immunonutrition shows promise, additional research is crucial to refine protocols and establish optimal clinical practice utilization. -
Citations
Citations to this article as recorded by- The 2024 Korean Enhanced Recovery After Surgery (ERAS) guidelines for colorectal cancer: a secondary publication
Kil-yong Lee, Soo Young Lee, Miyoung Choi, Moonjin Kim, Ji Hong Kim, Ju Myung Song, Seung Yoon Yang, In Jun Yang, Moon Suk Choi, Seung Rim Han, Eon Chul Han, Sang Hyun Hong, Do Joong Park, Sang-Jae Park
Annals of Coloproctology.2025; 41(1): 3. CrossRef - Efficacy of preoperative immunonutrition in malnourished patients undergoing colorectal cancer surgery: a study protocol for a multicenter randomized clinical trial
Soo Young Lee, Chang Hyun Kim, Gi Won Ha, Soo Yeun Park, In Jun Yang, Jin Soo Kim, Gyung Mo Son, Sung Il Kang, Sung Uk Bae
Trials.2025;[Epub] CrossRef - The 2024 Korean Enhanced Recovery After Surgery guidelines for colorectal cancer
Kil-yong Lee, Soo Young Lee, Miyoung Choi, Moonjin Kim, Ji Hong Kim, Ju Myung Song, Seung Yoon Yang, In Jun Yang, Moon Suk Choi, Seung Rim Han, Eon Chul Han, Sang Hyun Hong, Do Joong Park, Sang-Jae Park
Annals of Clinical Nutrition and Metabolism.2024; 16(2): 22. CrossRef
- The 2024 Korean Enhanced Recovery After Surgery (ERAS) guidelines for colorectal cancer: a secondary publication
- 17,509 View
- 126 Download
- 3 Crossref

- Effect of Probiotics/Synbiotics on Postoperative Outcomes in Patients Undergoing Abdominal Surgery
-
In Ja Park

- Ann Clin Nutr Metab 2022;14(1):10-19. Published online June 1, 2022
- DOI: https://doi.org/10.15747/ACNM.2022.14.1.10
-
 Abstract
Abstract
 PDF
PDF - Environmental factors, drugs, diet, and surgery alter the composition of the gut microbiota leading to the production of different metabolites or toxins that can cause disease or delay postoperative recovery. Surgical damage leads to gut barrier disruption, increased intestinal permeability, gut microbial imbalance, and immunologic compromise of the host with subsequent bacterial translocation from the gastrointestinal tract to systemic circulation. Therefore, perioperative stabilization of the intestinal microbiota is a potential method of reducing postoperative complication rates. Probiotics have been proposed as a viable option for prophylaxis of postoperative infections through increased intestinal motility to prevent bacterial overgrowth, improve gut barrier function, and modulate immune response. This review investigates microbial changes after surgery and the influence of probiotics on postoperative microbial composition. Infectious postoperative complications and immunologic changes related to probiotics/synbiotics were also reviewed in patients who underwent abdominal surgery.
-
Citations
Citations to this article as recorded by- The gut microbiome in colorectal anastomotic leakage: from mechanisms to precision
Songlin Sun, Feng Long, Bowen Su, Jiahan Chen, Yihuan Luo, Yang Zhong, Guangjun Zhang
Frontiers in Medicine.2026;[Epub] CrossRef - Postoperative gut dysbiosis and its clinical implications, with an emphasis on probiotic strategies in gastric cancer patients undergoing gastrectomy: a narrative review
Cheong Ah Oh
Ann Clin Nutr Metab.2025; 17(2): 114. CrossRef - Formoterol promotes mitochondrial biogenesis, improves liver regeneration, and suppresses liver injury and inflammation after liver resection in mice with endotoxemia
Amir K Richardson
International Journal of Physiology, Pathophysiology and Pharmacology.2025; 17(4): 131. CrossRef - Probiotics in the Management of Surgery- Induced Diarrhea: Efficacy and Clinical Applications
P. Dhivyaprasath, Gayathri R, Poovitha M, Rabiyath Riswana M, Sabithra P, Susitha R
International Journal of Innovative Science and Research Technology.2024; : 1482. CrossRef
- The gut microbiome in colorectal anastomotic leakage: from mechanisms to precision
- 14,405 View
- 141 Download
- 4 Crossref

- Preoperative Neutrophil to Lymphocyte Ratio and Albumin Level as Predictors for Postoperative Complication in Patients with Colorectal Cancer
-
Kyung Pil Kang
 , Young Hun Kim
, Young Hun Kim , Kyung Jong Kim PhD.
, Kyung Jong Kim PhD.
- Surg Metab Nutr 2020;11(2):66-72. Published online December 30, 2020
- DOI: https://doi.org/10.18858/smn.2020.11.2.66
-
 Abstract
Abstract
 PDF
PDF - Purpose: Systematic inflammatory response biomarkers are recognized as potential prognostic factors for colorectal cancer (CRC). Recently, the neutrophil-to-lymphocyte ratio (NLR) has emerged as a possible marker for predicting the outcomes of patients with CRC. The purpose of the current study was to determine if NLR could function as a predictive marker of postoperative complications in patients with colorectal cancer who were treated surgically.
Materials and Methods: One hundred and seven patients who underwent radical surgery for colorectal cancer were enrolled in the study. The NLR values were determined from the complete blood counts within one month before surgery. Values of less than or greater than 3 were defined as low (NLR-low) or high (NLR-high), respectively. Statistical comparisons were made between the NLR and the clinical-pathological variables.
Results: Sixty-eight patients met the criteria of NLR-low, and 39 patients were categorized as NLR-high. The NLR status was significantly correlated with T-stage, perineural invasion, and an increased likelihood of complications. Univariate analysis indicated that both low albumin and meeting the criteria for the NLR-high group correlated with an increased occurrence of complications (P=0.004, P=0.004, respectively). Multivariate analysis identified NLR-high and low albumin levels as independent predictors for complications (P=0.007, odd ratio=6.405, P=0.016, odd ratio=9.641, respectively)
Conclusion: The current results suggest that the preoperative NLR levels could be useful tools for predicting the occurrence of postoperative complications.
- 1,889 View
- 9 Download

- Postoperative Weight Changes, Nutritional Status and Clinical Significance of Colorectal Cancer Patients
- Sun Young Kim, Ji Sun Kim, Eon Chul Han
- Surg Metab Nutr 2019;10(2):46-53. Published online December 30, 2019
- DOI: https://doi.org/10.18858/smn.2019.10.2.46
-
 Abstract
Abstract
 PDF
PDF Purpose:
Although weight loss is an important factor for assessing the nutritional status, patient counselling or management is limited due to fewer studies on weight loss after colorectal cancer surgery.
Materials and Methods:
Totally, 374 patients were included in the analysis (between August 2010 to December 2016). Patients’ weight was determined before surgery, and at 1 week, 6 weeks, 3 months, and 6 months after surgery. Change in weight was reviewed based on the gender and administration of chemotherapy. Severe weight loss is defined as greater than 5% weight loss after surgery.
Results:
The weight changes post-surgery at 1 week (−2.56±2.62 vs. −3.36±2.68, P<0.005), 6 weeks (−3.23±3.82 vs. −4.57±3.96, P=0.001), and 3 months (−0.93±5.01 vs. −2.79±4.86, P<0.001) were significantly greater in male subjects, as compared to female patients. However, at 6 months post-surgery, most patients showed weight gain with no statistical significance between the genders (1.11±4.64 vs. 1.94±6.26, P=0.143). Weight change based on treatment (with or without chemotherapy) reveal significant differences between the genders at 3 months post-surgery only (−1.33±4.65 vs. −2.52 ±5.15, P=0.027). Multivariate analysis for factors of severe weight loss show that the male gender [adjusted odds ratio (OR): 1.83, P=0.027)], adjuvant chemotherapy (adjusted OR 2.11, P=0.008), and presence of post-operative complications (adjusted OR 2.12, P=0.029) were significant factors.
Conclusion:
In postoperative colorectal cancer patients, the weight and nutritional status require careful monitoring for at least 2 months after surgery, in order to prevent hindrance to chemotherapy. (Surg Metab Nutr 2019;10:-53)
-
Citations
Citations to this article as recorded by- The impact of pre‐surgery nutrition intervention on weight loss, nutrition status, and quality of life in colorectal cancer patients with elective surgery
Wen Lynn Teong, Wei Yee Wong, Su Lin Lim, Choon Hui Low, Cassandra Lim Duan Qi, Ruochen Du
Malignancy Spectrum.2025; 2(2): 74. CrossRef - Serial measurements of body composition using bioelectrical impedance and clinical usefulness of phase angle in colorectal cancer
Seung‐Rim Han, Jung Hoon Bae, Chul Seung Lee, Abdullah Al‐Sawat, Soo Ji Park, Hyo Jin Lee, Mi Ran Yoon, Hyeong Yong Jin, Yoon Suk Lee, Do Sang Lee, In Kyu Lee
Nutrition in Clinical Practice.2022; 37(1): 153. CrossRef
- The impact of pre‐surgery nutrition intervention on weight loss, nutrition status, and quality of life in colorectal cancer patients with elective surgery
- 3,238 View
- 16 Download
- 2 Crossref

- Nutrition Support for Pediatric Surgical Patients
- Jun Beom Park
- Surg Metab Nutr 2019;10(1):9-14. Published online June 30, 2019
- DOI: https://doi.org/10.18858/smn.2019.10.1.9
-
 Abstract
Abstract
 PDF
PDF Pediatric patients have characteristics such as a low capacity for storing energy/nutrients and high energy metabolism as compared those of adults. Because of the inherent characteristics that they are continually growing, supplying both rapid and adequate nutrition is of the utmost importance. In the case of children undergoing surgery (and particularly gastrointestinal surgery), there is a high possibility of a restricted supply of nutrition, and so active intervention to supply sufficient nutrition must be carried out. Of course, enteral nutrition is preferred, but continuous monitoring of nutrition is of paramount importance; thus, parenteral nutrition should be provided when necessary. Nutritional support requires continuous monitoring when and if complications arise. The complications of parenteral nutrition have yet to be overcome, so further research on this topic is certainly warranted.
- 1,133 View
- 6 Download

- Major Surgery in Sarcopenic Patients
- Kyung Won Seo
- Surg Metab Nutr 2019;10(1):5-8. Published online June 30, 2019
- DOI: https://doi.org/10.18858/smn.2019.10.1.5
-
 Abstract
Abstract
 PDF
PDF Sarcopenia refers to reduced muscle mass in the elderly population, and this malady is of great interest in clinical course, including postoperative complications and mortality when treating major cancer in the elderly. The definition of sarcopenia varies according to the method of measuring muscle mass, and the skeletal muscle index (SMI) tends to be extensively used in retrospective studies. In many reports, sarcopenia has been reported to be a poor prognostic factor after gastrectomy, colectomy, pancreatectomy and liver transplantation, with regards to complications and the length of the hospital stay. Additionally, patients suffering from sarcopenia have a higher medical burden due to their poor clinical outcome after surgery. To overcome these difficulties, nutritional support and exercise training to improve sarcopenia before surgery is helpful, and so further studies that focus on these treatments need to be conducted.
- 1,121 View
- 2 Download

- Nutritional Therapy Related Complications in Hospitalized Adult Patients: A Korean Multicenter Trial
- Eun-Mi Seol, Kye Sook Kwon, Jeong Goo Kim, Jung-Tae Kim, Jihoon Kim, Sun-Mi Moon, Do Joong Park, Jung Hyun Park, Je Hoon Park, Ji Young Park, Jung-Min Bae, Seung Wan Ryu, Ji-Young Sul, Dong Woo Shin, Cheung Soo Shin, Byung Kyu Ahn, Soo Min Ahn, Hee Chul Yu, Gil Jae Lee, Sanghoon Lee, A Ran Lee, Jae Young Jang, Hyun Jeong Jeon, Sung Min Jung, Sung-Sik Han, Suk-Kyung Hong, Sun-Hwi Hwang, Yunhee Choi, Hyuk-Joon Lee
- J Clin Nutr 2019;11(1):12-22. Published online June 30, 2019
- DOI: https://doi.org/10.15747/jcn.2019.11.1.12
-
 Abstract
Abstract
 PDF
PDF Purpose:
Nutritional therapy (NT), such as enteral nutrition (EN) or parenteral nutrition (PN), is essential for the malnourished patients. Although the complications related to NT has been well described, multicenter data on symptoms in the patients with receiving NT during hospitalization are still lacking.
Methods:
Nutrition support team (NST) consultations, on which NT-related complications were described, were collected retrospectively for one year. The inclusion criteria were patients who were (1) older than 18 years, (2) hospitalized, and (3) receiving EN or PN at the time of NST consultation. The patients’ demographics (age, sex, body mass index [BMI]), type of NT and type of complication were collected. To compare the severity of each complication, the intensive care unit (ICU) admission, hospital stay, and type of discharge were also collected.
Results:
A total of 14,600 NT-related complications were collected from 13,418 cases from 27 hospitals in Korea. The mean age and BMI were 65.4 years and 21.8 kg/m2. The complications according to the type of NT, calorie deficiency (32.4%, n=1,229) and diarrhea (21.6%, n=820) were most common in EN. Similarly, calorie deficiency (56.8%, n=4,030) and GI problem except for diarrhea (8.6%, n=611) were most common in PN. Regarding the clinical outcomes, 18.7% (n=2,158) finally expired, 58.1% (n=7,027) were admitted to ICU, and the mean hospital days after NT-related complication were 31.3 days. Volume overload (odds ratio [OR]=3.48) and renal abnormality (OR=2.50) were closely associated with hospital death; hyperammonemia (OR=3.09) and renal abnormality (OR=2.77) were associated with ICU admission; “micronutrient and vitamin deficiency” (geometric mean [GM]=2.23) and volume overload (GM=1.61) were associated with a longer hospital stay.
Conclusion:
NT may induce or be associated with several complications, and some of them may seriously affect the patient’s outcome. NST personnel in each hospital should be aware of each problem during nutritional support.
-
Citations
Citations to this article as recorded by- Provision of Enteral Nutrition in the Surgical Intensive Care Unit: A Multicenter Prospective Observational Study
Chan-Hee Park, Hak-Jae Lee, Suk-Kyung Hong, Yang-Hee Jun, Jeong-Woo Lee, Nak-Jun Choi, Kyu-Hyouck Kyoung
Annals of Clinical Nutrition and Metabolism.2022; 14(2): 66. CrossRef - Pathophysiology and protective approaches of gut injury in critical illness
Chang Yeon Jung, Jung Min Bae
Yeungnam University Journal of Medicine.2021; 38(1): 27. CrossRef - Nutrition Support Team Reconsultation During Nutrition Therapy in Korea
Eun‐Mi Seol, Yun‐Suhk Suh, Dal Lae Ju, Hye Jung Bae, Eunjung Kim, Hyuk‐Joon Lee
Journal of Parenteral and Enteral Nutrition.2021; 45(2): 357. CrossRef
- Provision of Enteral Nutrition in the Surgical Intensive Care Unit: A Multicenter Prospective Observational Study
- 1,702 View
- 10 Download
- 3 Crossref

- Quality Improvement Activities to Facilitate the Filing of Complexity Payment Claims for Patients with Malnutrition
- Kuk Hwan Kwon, Hyung Soon Lee, Jee Hyoung Yoo, Soo Na Chi, Hyun Hee Park, So Won Kim, Kyung Ran Kim, Nan Hee Yun, Kyoung Taek Ra, Hyun Jung Song
- J Clin Nutr 2018;10(1):20-24. Published online June 30, 2018
- DOI: https://doi.org/10.15747/jcn.2018.10.1.20
-
 Abstract
Abstract
 PDF
PDF Purpose:
The grade of complexity in the diagnosis related group (DRG) payment system is influenced by the secondary diagnosis of specific complication and comorbidity level, in which moderate or severe malnutrition is included. This study examined an existing proportion of patients with malnutrition who were supposed to be qualified for the complexity level and devised quality improvement measures to increase the proportion of qualifying complexity payments.
Methods:
The goal of the activities was to increase the rate of complexity payment claims for patients with malnutrition (%). Cases ineligible for the DRG payment system and cases with no diagnosis of malnutrition were excluded. We established a collaborative system between the nutrition support team and departments related to each improvement factor (
i.e ., patient care, medical records, insurance review, and medical information).Results:
Before implementing the activities, this study investigated the current level of complexity payment claims for malnutrition patients who were discharged within a specific period (June 1, 2015∼August 31, 2015). The results showed that complexity payment claims were filed in 10.00% (2 of the 20 malnutrition cases). After the activities, the rate of complexity payment claims for the patients with malnutrition within the study period (June 1, 2016∼August 31, 2016) was 46.43% (26 out of 56), showing an approximately 364% increase from the pre activity rate. This change was statistically significant according to the chi-square test on Microsoft Excel 2010 (P<0.01).
Conclusion:
Collaborative efforts by the related departments enabled the smooth implementation of each activity. In addition, moderate or severe malnutrition was revealed to be a variable in the complexity-specific payment system. In the future, hospital-wide awareness and effort are crucial to promot the steady practice of these activities and expand their implementation.
- 1,120 View
- 2 Download


 E-submission
E-submission KSPEN
KSPEN KSSMN
KSSMN ASSMN
ASSMN JSSMN
JSSMN
 First
First Prev
Prev


