Scopus, KCI, KoreaMed

Search
- Page Path
- HOME > Search
- Effectiveness of perioperative rehabilitation and nutrition in esophageal cancer: a narrative review
-
Ryoma Haneda
 , Yuki Sakai
, Yuki Sakai , Kenichi Sekimori
, Kenichi Sekimori , Tomohiro Murakami
, Tomohiro Murakami , Eisuke Booka
, Eisuke Booka , Tomohiro Matsumoto
, Tomohiro Matsumoto , Hirotoshi Kikuchi
, Hirotoshi Kikuchi , Yoshihiro Hiramatsu
, Yoshihiro Hiramatsu , Hiroya Takeuchi
, Hiroya Takeuchi
- Ann Clin Nutr Metab 2026;18(1):18-26. Published online March 30, 2026
- DOI: https://doi.org/10.15747/ACNM.25.0021
-
 Abstract
Abstract
 PDF
PDF - Purpose
Esophageal cancer surgery requires robust perioperative management to reduce its high rate of complications. This review evaluates the clinical utility of comprehensive exercise and nutritional therapy, with a specific focus on initiatives led by the multidisciplinary Hamamatsu Perioperative Care Team (HOPE), established at Hamamatsu University Hospital to optimize patient safety and postoperative recovery outcomes.
Current concept
The HOPE protocol involves a diverse team, including surgeons, nurses, pharmacists, and dietitians, who collaboratively implement a multifaceted perioperative care bundle. These interventions include strict smoking cessation, intensive oral care, and immunonutrition incorporating n-3 fatty acids. A distinctive feature of this program is the integration of patient-reported treatment diaries and wearable fitness tracking devices (WFTs) to visualize daily activity, thereby helping to sustain patient motivation. Preoperative rehabilitation focuses on preventing sarcopenia through combined aerobic and resistance training, while postoperative care emphasizes immediate enteral nutrition and early mobilization. Retrospective analyses demonstrated that HOPE implementation reduced Clavien-Dindo grade III or higher infectious complications, pneumonia and surgical site infections, compared with historical controls. In addition, a propensity score–matched analysis showed that WFT users experienced lower pneumonia rates, shorter hospital stays, and better preservation of nutritional markers, including albumin and transthyretin, during the recovery phase compared with non-users.
Conclusion
The HOPE strategy illustrates that combining standard nutritional support and exercise therapy with digital tools enables individualized rehabilitation. This integrated approach reduces morbidity and preserves function, strongly suggesting that incorporation of wearable technology into established surgical care protocols represents a strategy for improving long-term outcomes in high-risk cancer patients.
- 617 View
- 15 Download

- Impact of tube feeding after pancreaticoduodenectomy on nutritional intake and status: a retrospective cohort study in Japan
-
Masaharu Ishida
 , Masahiro Iseki
, Masahiro Iseki , Shuichiro Hayashi
, Shuichiro Hayashi , Aya Noguchi
, Aya Noguchi , Hideaki Sato
, Hideaki Sato , Shingo Yoshimachi
, Shingo Yoshimachi , Akiko Kusaka
, Akiko Kusaka , Mitsuhiro Shimura
, Mitsuhiro Shimura , Shuichi Aoki
, Shuichi Aoki , Daisuke Douchi
, Daisuke Douchi , Takayuki Miura
, Takayuki Miura , Shimpei Maeda
, Shimpei Maeda , Masamichi Mizuma
, Masamichi Mizuma , Kei Nakagawa
, Kei Nakagawa , Takashi Kamei
, Takashi Kamei , Michiaki Unno
, Michiaki Unno
- Ann Clin Nutr Metab 2025;17(3):203-209. Published online December 1, 2025
- DOI: https://doi.org/10.15747/ACNM.25.0020
-
 Graphical Abstract
Graphical Abstract
 Abstract
Abstract
 PDF
PDF 
- Purpose
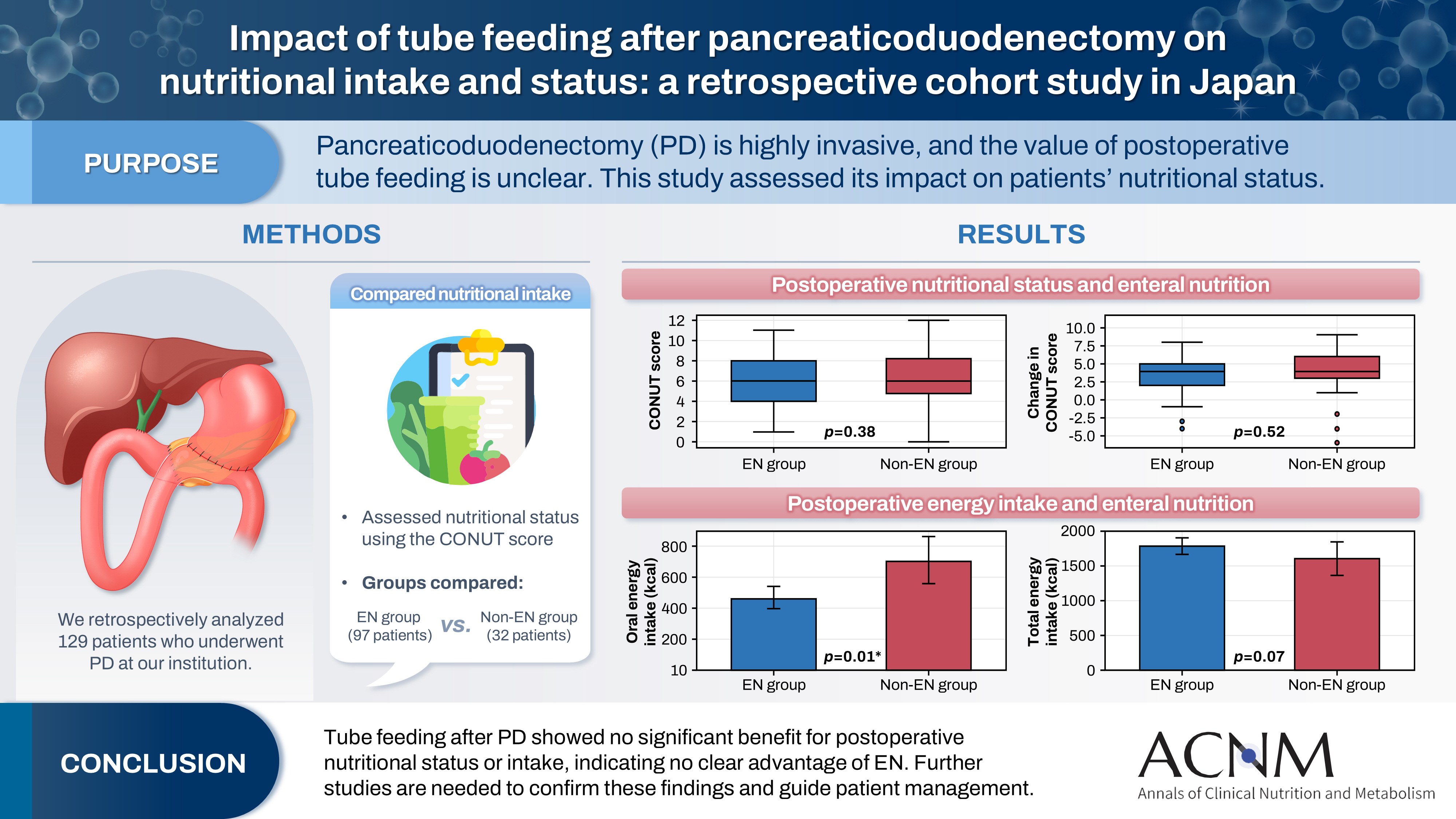
Pancreaticoduodenectomy (PD) is one of the most invasive procedures in gastrointestinal surgery. However, the clinical significance of postoperative tube feeding remains unclear. This study investigated the impact of enteral nutrition (EN) on the postoperative nutritional status of patients undergoing PD.
Methods
We retrospectively analyzed 129 patients who underwent PD at Tohoku University Hospital. Nutritional intake and status, evaluated using the Controlling Nutritional Status score, were compared between two groups: an EN group (97 patients) and a non-EN group (32 patients).
Results
There were no significant differences between the two groups in age, sex, body mass index, underlying diseases, operative duration, blood loss, postoperative pancreatic fistula, postoperative complications, delayed gastric emptying, or length of hospital stay. Although the EN group showed improvements in nutritional status both at discharge and compared with preoperative values, none of these changes reached statistical significance. Oral caloric intake was significantly higher in the non-EN group (P=0.01). In contrast, total energy intake was higher in the EN group, but this difference did not reach statistical significance (P=0.07).
Conclusion
Tube feeding after PD did not significantly influence postoperative nutritional status or overall nutritional intake. These findings suggest that EN offers no clear advantage over other approaches; however, further research is warranted to validate these results, refine existing guidelines, and optimize postoperative patient management.
- 1,228 View
- 20 Download

- Role of preoperative immunonutrition in patients with colorectal cancer: a narrative review
-
Soo Young Lee
 , Hyeung-min Park
, Hyeung-min Park , Chang Hyun Kim
, Chang Hyun Kim , Hyeong Rok Kim
, Hyeong Rok Kim
- Ann Clin Nutr Metab 2023;15(2):46-50. Published online August 1, 2023
- DOI: https://doi.org/10.15747/ACNM.2023.15.2.46
-
 Abstract
Abstract
 PDF
PDF - Purpose: Colorectal cancer surgery presents challenges due to surgical stress and immunosuppression, leading to postoperative complications. Nutrition is crucial for colorectal cancer patients who are prone to malnutrition. This study aims to provide a comprehensive review of the role of preoperative immunonutrition in colorectal cancer surgery.
Current concept: Preoperative immunonutrition, consisting of immunonutrients such as arginine, ω-3 fatty acids, and nucleotides, has emerged as a potential strategy to enhance surgical outcomes by modulating immune responses and reducing complications. Current guidelines recommend preoperative oral nutritional supplements for major abdominal surgery and immunonutrition for nutritionally high-risk patients. Meta-analysis have demonstrated significant decreases in infectious complications and hospital stay durations with preoperative immunonutrition. However, limitations such as publication bias and heterogeneity in the previous studies should be considered. Further research should focus on the optimal timing, duration, and amount of immunonutrition; the patient populations that would benefit most; and the integration of immunonutrition into enhanced recovery after surgery protocols.
Conclusion: While preoperative immunonutrition shows promise, additional research is crucial to refine protocols and establish optimal clinical practice utilization. -
Citations
Citations to this article as recorded by- The 2024 Korean Enhanced Recovery After Surgery (ERAS) guidelines for colorectal cancer: a secondary publication
Kil-yong Lee, Soo Young Lee, Miyoung Choi, Moonjin Kim, Ji Hong Kim, Ju Myung Song, Seung Yoon Yang, In Jun Yang, Moon Suk Choi, Seung Rim Han, Eon Chul Han, Sang Hyun Hong, Do Joong Park, Sang-Jae Park
Annals of Coloproctology.2025; 41(1): 3. CrossRef - Efficacy of preoperative immunonutrition in malnourished patients undergoing colorectal cancer surgery: a study protocol for a multicenter randomized clinical trial
Soo Young Lee, Chang Hyun Kim, Gi Won Ha, Soo Yeun Park, In Jun Yang, Jin Soo Kim, Gyung Mo Son, Sung Il Kang, Sung Uk Bae
Trials.2025;[Epub] CrossRef - The 2024 Korean Enhanced Recovery After Surgery guidelines for colorectal cancer
Kil-yong Lee, Soo Young Lee, Miyoung Choi, Moonjin Kim, Ji Hong Kim, Ju Myung Song, Seung Yoon Yang, In Jun Yang, Moon Suk Choi, Seung Rim Han, Eon Chul Han, Sang Hyun Hong, Do Joong Park, Sang-Jae Park
Annals of Clinical Nutrition and Metabolism.2024; 16(2): 22. CrossRef
- The 2024 Korean Enhanced Recovery After Surgery (ERAS) guidelines for colorectal cancer: a secondary publication
- 17,510 View
- 126 Download
- 3 Crossref

- Preoperative consumption of a carbohydrate drink before laparoscopic cholecystectomy is safe and beneficial in Korea: a non-randomized controlled study
-
Yoo Jin Choi
 , Yoonhyeong Byun
, Yoonhyeong Byun , Seong Mi Yang
, Seong Mi Yang , Ho-Jin Lee
, Ho-Jin Lee , Hongbeom Kim
, Hongbeom Kim
- Ann Clin Nutr Metab 2023;15(1):15-21. Published online April 1, 2023
- DOI: https://doi.org/10.15747/ACNM.2023.15.1.15
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Purpose: Overnight fasting prior to elective surgery is the traditional way of avoiding the risk of aspiration during anesthesia induction. However, it causes mental and metabolic stress to patients. Therefore, we investigated the safety and potential benefits of the preoperative consumption of a carbohydrate drink.
Methods: This was a single-center prospective, nonrandomized study with questionnaire. Patients scheduled for elective laparoscopic cholecystectomy were included. There was no restriction on age, underlying diseases, and biliary drainage prior to surgery. They were preoperatively given either a carbohydrate drink or were instructed to fast from midnight before surgery. Perioperative emotional status was measured using the visual analog scale.
Results: The 132 patients completed the questionnaire, with 68 receiving the carbohydrate drink and 64 following nil per oral after-midnight instruction. There were no postoperative complications related to preoperative drink consumption or the cholecystectomy procedure itself in both groups. There were no significant differences in all the assessed feelings postoperatively except that preoperative discomforts, such as hunger and thirst, were significantly more alleviated in the group of preoperative consumption of a carbohydrate drink.
Conclusion: Preoperative consumption of a carbohydrate drink was found to be safe and effective in alleviating preoperative discomfort in elective surgery patients, including older patients and those with underlying comorbidities, who were at greater risk for aspiration. Therefore, we recommend considering preoperative drink consumption as an alternative to traditional overnight fasting in elective surgery patients. -
Citations
Citations to this article as recorded by- MODERN CONCEPT OF POSTOPERATIVE ANALGESIA IN PATIENTS UNDERGOING URGENT LAPAROSCOPIC CHOLECYSTECTOMY
O. PYLYPENKO, O. KRAVETS
Pain anesthesia and intensive care.2024; (4(109)): 55. CrossRef
- MODERN CONCEPT OF POSTOPERATIVE ANALGESIA IN PATIENTS UNDERGOING URGENT LAPAROSCOPIC CHOLECYSTECTOMY
- 9,299 View
- 92 Download
- 1 Crossref

- Effect of Probiotics/Synbiotics on Postoperative Outcomes in Patients Undergoing Abdominal Surgery
-
In Ja Park

- Ann Clin Nutr Metab 2022;14(1):10-19. Published online June 1, 2022
- DOI: https://doi.org/10.15747/ACNM.2022.14.1.10
-
 Abstract
Abstract
 PDF
PDF - Environmental factors, drugs, diet, and surgery alter the composition of the gut microbiota leading to the production of different metabolites or toxins that can cause disease or delay postoperative recovery. Surgical damage leads to gut barrier disruption, increased intestinal permeability, gut microbial imbalance, and immunologic compromise of the host with subsequent bacterial translocation from the gastrointestinal tract to systemic circulation. Therefore, perioperative stabilization of the intestinal microbiota is a potential method of reducing postoperative complication rates. Probiotics have been proposed as a viable option for prophylaxis of postoperative infections through increased intestinal motility to prevent bacterial overgrowth, improve gut barrier function, and modulate immune response. This review investigates microbial changes after surgery and the influence of probiotics on postoperative microbial composition. Infectious postoperative complications and immunologic changes related to probiotics/synbiotics were also reviewed in patients who underwent abdominal surgery.
-
Citations
Citations to this article as recorded by- The gut microbiome in colorectal anastomotic leakage: from mechanisms to precision
Songlin Sun, Feng Long, Bowen Su, Jiahan Chen, Yihuan Luo, Yang Zhong, Guangjun Zhang
Frontiers in Medicine.2026;[Epub] CrossRef - Postoperative gut dysbiosis and its clinical implications, with an emphasis on probiotic strategies in gastric cancer patients undergoing gastrectomy: a narrative review
Cheong Ah Oh
Ann Clin Nutr Metab.2025; 17(2): 114. CrossRef - Formoterol promotes mitochondrial biogenesis, improves liver regeneration, and suppresses liver injury and inflammation after liver resection in mice with endotoxemia
Amir K Richardson
International Journal of Physiology, Pathophysiology and Pharmacology.2025; 17(4): 131. CrossRef - Probiotics in the Management of Surgery- Induced Diarrhea: Efficacy and Clinical Applications
P. Dhivyaprasath, Gayathri R, Poovitha M, Rabiyath Riswana M, Sabithra P, Susitha R
International Journal of Innovative Science and Research Technology.2024; : 1482. CrossRef
- The gut microbiome in colorectal anastomotic leakage: from mechanisms to precision
- 14,406 View
- 141 Download
- 4 Crossref

- Preoperative Neutrophil to Lymphocyte Ratio and Albumin Level as Predictors for Postoperative Complication in Patients with Colorectal Cancer
-
Kyung Pil Kang
 , Young Hun Kim
, Young Hun Kim , Kyung Jong Kim PhD.
, Kyung Jong Kim PhD.
- Surg Metab Nutr 2020;11(2):66-72. Published online December 30, 2020
- DOI: https://doi.org/10.18858/smn.2020.11.2.66
-
 Abstract
Abstract
 PDF
PDF - Purpose: Systematic inflammatory response biomarkers are recognized as potential prognostic factors for colorectal cancer (CRC). Recently, the neutrophil-to-lymphocyte ratio (NLR) has emerged as a possible marker for predicting the outcomes of patients with CRC. The purpose of the current study was to determine if NLR could function as a predictive marker of postoperative complications in patients with colorectal cancer who were treated surgically.
Materials and Methods: One hundred and seven patients who underwent radical surgery for colorectal cancer were enrolled in the study. The NLR values were determined from the complete blood counts within one month before surgery. Values of less than or greater than 3 were defined as low (NLR-low) or high (NLR-high), respectively. Statistical comparisons were made between the NLR and the clinical-pathological variables.
Results: Sixty-eight patients met the criteria of NLR-low, and 39 patients were categorized as NLR-high. The NLR status was significantly correlated with T-stage, perineural invasion, and an increased likelihood of complications. Univariate analysis indicated that both low albumin and meeting the criteria for the NLR-high group correlated with an increased occurrence of complications (P=0.004, P=0.004, respectively). Multivariate analysis identified NLR-high and low albumin levels as independent predictors for complications (P=0.007, odd ratio=6.405, P=0.016, odd ratio=9.641, respectively)
Conclusion: The current results suggest that the preoperative NLR levels could be useful tools for predicting the occurrence of postoperative complications.
- 1,889 View
- 9 Download

- Risk of Malnutrition after Gastrointestinal Cancer Surgery: A Propensity Score Matched Retrospective Cohort Study
- Sung-Hoon Yoon, Bong-Hyeon Kye, Hyung-Jin Kim, Kyong-Hwa Jun, Hyeon-Min Cho, Hyung-Min Chin
- Surg Metab Nutr 2018;9(1):16-25. Published online June 30, 2018
- DOI: https://doi.org/10.18858/smn.2018.9.1.16
-
 Abstract
Abstract
 PDF
PDF Purpose:
Patients with cancers arising from the gastrointestinal tract can suffer from nutritional inadequacies caused by various factors. This study investigated the risk of malnutrition after curative surgery in patients with gastric cancer (GC) or colorectal cancer (CRC) using various preoperative and postoperative nutritional screening tools.
Materials and Methods:
In the authors’ hospital, 407 patients (206 patients with GC and 201 patients with CRC) underwent surgery between July 2011 and June 2012. The patients from the two groups were matched using the propensity score and then analyzed the nutritional data from 170 patients (85 patients in each group), retrospectively.
Results:
In both groups, the postoperative nutritional status was impaired significantly compared to the preoperative status. The postoperative risk of undernutrition in CRC patients was significantly lower than that of the GC patients according to the Malnutrition Universal Screening Tool (P=0.007). At the time of hospital discharge after surgery, the incidence of a lower serum albumin level (P=0.002) and more than 5% weight loss (P=0.013) were higher in the GC group than in the CRC group. A comparison of the postoperative nutritional status among the types of surgery in each group, total gastrectomy in the GC group (P=0.015) and proctectomy with diverting stoma in the CRC group (P=0.06), were related to more than 5% weight loss.
Conclusion:
Gastrointestinal cancer surgery might increase the patients’ postoperative risk of malnutrition, particularly in GC surgery. Therefore, consecutive assessments of the nutritional status and appropriate nutritional support are necessary after surgery for GC and CRC.
-
Citations
Citations to this article as recorded by- Feasibility and Safety of Early Oral Feeding After Radical Gastrectomy in Patients With Gastric Carcinoma: A Systematic Review
Wahida Ali, Wahidullah Dost, Mohammad Nazir Zaman, Mohammad Qaher Rasully , Jamaluddin Niazi, Farzad Qasemi, Raisa Dost, Wahida Dost, Danyal Bakht, Syed Faqeer Hussain Bokhari
Cureus.2024;[Epub] CrossRef - Preoperative Body Mass Index, Waist Circumference, and Mortality After Major Cancer Surgery: A Nationwide Cohort Study in Korea
Tak Kyu Oh, In-Ae Song
Journal of Korean Medical Science.2023;[Epub] CrossRef - Nutritional Counseling Protocol for Colorectal Cancer Patients after Surgery Improves Outcome
Isabelle R. Novelli, Bruno A. D. Araújo, Laura F. Grandisoli, Elianete C. G. Furtado, Evelyn K. N. Aguchiku, Marina C. G. Bertocco, Tassiane P. Sudbrak, Isabel C. de Araújo, Ana C. F. Bosko, Nágila R. T. Damasceno
Nutrition and Cancer.2021; 73(11-12): 2278. CrossRef
- Feasibility and Safety of Early Oral Feeding After Radical Gastrectomy in Patients With Gastric Carcinoma: A Systematic Review
- 2,656 View
- 14 Download
- 3 Crossref

- Role of Postoperative Parenteral Nutrition in Elective Surgery; Selection of Patients and Conditions for Postoperative Parenteral Nutrition
- Jong Won Kim
- Surg Metab Nutr 2018;9(1):1-4. Published online June 30, 2018
- DOI: https://doi.org/10.18858/smn.2018.9.1.1
-
 Abstract
Abstract
 PDF
PDF Postoperative early enteral nutrition or early oral ingestion is recommended in surgical patients. In this situation, this study examined the role of parenteral nutrition in the postoperative period in patients undergoing elective surgery. The nutritional status should be assessed before surgery and in the case of malnutrition, nutritional support should be provided before surgery to obtain good results. More than 2 weeks of insufficient nutritional support after surgery may worsen the patient’s progress. Therefore, it is recommended to start nutritional care if the oral intake is not appropriate until 7 days or 5 to 7 days after surgery. Enteral nutrition is related to the quick restoration of the bowel function and reduction of infection-related complications. Therefore, enteral nutrition has priority. On the other hand, depending on the patient’s condition, it may not be possible to perform enteral nutrition, and the uniform implementation of the early enteral nutrition may be a burden to the patient. Parenteral nutrition has the advantage that it can supply nutrition without being affected by the intestinal condition, and it can be calculated to supply as much energy as required. The situation, where parenteral nutrition is required after elective surgery, could be summarized as 1) the patients who underwent nutritional therapy before surgery and could not tolerate oral intake or enteral nutrition after surgery. or 2) in the case where enteral nutrition did not satisfy 50% of the demand at 7 days after surgery, and it is judged that this situation should continue for 7 days.
- 836 View
- 3 Download

- Analysis of Current Status and Predisposing Factors for Nutritional Support of Patients in Surgical Intensive Care Unit
- Byung Chul Kim, In Kyu Lee, Eun Young Kim
- Surg Metab Nutr 2016;7(2):32-38. Published online December 30, 2016
- DOI: https://doi.org/10.18858/smn.2016.7.2.32
-
 Abstract
Abstract
 PDF
PDF Purpose:
Enteral feeding is strongly recommended for critically ill patients since it can enhance the immunologic function, which serves as a host defense mechanism against inflammation or metabolic response to stress. Herein, we investigated nutritional status and estimated the adequacy of the nutritional supply for acutely ill patients admitted to the surgical intensive care unit (SICU) after a major operation.
Materials and Methods:
From February to October 2016, patients admitted and stayed over 48 hours after major surgical procedures at SICU in Seoul St. Mary’s Hospital were reviewed. The nutritional parameters and surgical outcomes were compared according to the status of nutritional support.
Results:
A total of 220 patients composed of 130 males (59.1%) and 90 females (40.9%) were enrolled, and mean age was 61.4±13.6 years. All patients were classified into two groups according to nutritional status, which was assessed by the ratio of total delivered calories to total required calories (D/R); group A (54 cases, 24.5%, D/R≥0.7) versus group B (166 cases, 75.5%, D/R<0.7). In multivariate analysis, incision in the lower abdomen (Odds Ratio 2.277, P=0.078), absence of NST consultation (Odds Ratio 2.728, P=0.011), and not receive minimal invasive surgery (Odds Ratio 3.518, P=0.001) were independent risk factors associated with poor nutritional status.
Conclusion:
Clinicians should pay more attention to patients who had an incision in the lower abdomen or did not receive minimal invasive surgery or NST consultation, which would be predisposing factors for nutritional insufficiency resulting in postoperative morbidities.
-
Citations
Citations to this article as recorded by- Provision of Enteral Nutrition in the Surgical Intensive Care Unit: A Multicenter Prospective Observational Study
Chan-Hee Park, Hak-Jae Lee, Suk-Kyung Hong, Yang-Hee Jun, Jeong-Woo Lee, Nak-Jun Choi, Kyu-Hyouck Kyoung
Annals of Clinical Nutrition and Metabolism.2022; 14(2): 66. CrossRef
- Provision of Enteral Nutrition in the Surgical Intensive Care Unit: A Multicenter Prospective Observational Study
- 1,439 View
- 0 Download
- 1 Crossref

- Evaluation of Postoperative Nutrition Support with Commercial Peripheral Parenteral Nutrition after an Ivor-Lewis Esophagectomy in Patients with Esophageal Cancer
- Sun-woo Lee, Na-ri Lim, Hyo Jung Park, Yong-won In, Jeong-meen Seo, Young-mee Lee
- J Clin Nutr 2015;7(3):87-92. Published online December 31, 2015
- DOI: https://doi.org/10.15747/jcn.2015.7.3.87
-
 Abstract
Abstract
 PDF
PDF Purpose:
Deteriorated nutritional status is common during a hospital stay for esophagectomy in patients with esophageal cancer. Malnutrition in those patients is often marked compared with other gastrointestinal cancer. The purpose of this study is to evaluate the appropriateness of commercial peripheral parenteral nutrition (CPPN) use in patients who underwent Ivor-Lewis esophagectomy (I-L op).
Methods:
Patients who were provided with CPPN after I-L op were enrolled in this study from January to May 2015. Body weight, height, nutritional status, length of hospital stay, duration of CPPN therapy, and parenteral nutrition (PN) induced complications were assessed, respectively, using electronic medical records.
Results:
Thirty-nine patients were enrolled. Average age was 65.9 years and 36 patients were male. All patients were provided with the same CPPN. The duration of fasting and CPPN use was 5.8±1.4 days and 7.5±1.8 days, respectively. Calorie supported by CPPN was 22.6±3.5 kcal/kg/day and only 20.5% of patients (n=8) reached the daily target calories. Most frequent PN induced complication was phlebitis which occurred in 8 patients (20.5%). Calcium, magnesium, and transthyretin levels in serum were not monitored during the PN support period.
Conclusion:
The indications for CPPN were appropriate because the fasting duration in patients with I-L op was 5 to 10 days. Although a large portion of patients could not be supplied daily target calories, their nutrition status was not significantly changed on admission and at discharge. We did not find it necessary to individualize PN support for a short period after an I-L op in patients with esophageal cancer. Further study will be needed to determine why the incidence of phlebitis was dominant.
- 1,105 View
- 1 Download


 E-submission
E-submission KSPEN
KSPEN KSSMN
KSSMN ASSMN
ASSMN JSSMN
JSSMN
 First
First Prev
Prev


